1.TAVI Procedure
1.1 Objective, to obtain:
-An aortic calcium score
-An optimal view from aortic valve/root and left ventricle outflow tract.
-A complete description of the entire aorta and iliac vessels.
-The best vascular approach ( femoral vs subclavian).
1.2 Protocol/CTA planning:
a. An initial non-contrast prospective cardiac study to achieve aortic valve calcification
b. A second ECG-gated retrospective CTA study encompassing the entire chest from supraclavicular regions ( modified from a conventional Coronary CTA protocol)
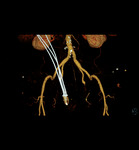
c. A third non-ECG-gated helical study including abdominopelvic regions is obtained( Fig.6 ).
Injection: Double injection, 70ml of iodinated contrast agent for cardiothoracic scan and 40 ml for the abdominal scan. A volume of 30 ml of saline is finally added. Beta-blocker, be carefully administered. No vasodilators used unless coronary anatomy is required.
1.3 Basic findings.
The aim of the study is to achieve a good anatomic approach to the aortic annulus ( Fig. 7 ) and valve, its morphology, and diameters, and to choose the best prosthetic dimensions for the replacement surgery. Hence, the landing zone must be well depicted.
Measurements:
· Aortic valve calcium score ( Fig.8 )
· Annulus area, perimeter, and diameter both for 40% and 60% of the R-R cycle. Description of anomalous cusps, if present.
· The vertical distance between the annulus level and both coronary ostia.
· Thoracic aortic diameters from root to descending aorta.
· Subdiaphragmatic aortoiliac diameters with atheroma and tortuosity description. Femoral arteries diameters with atheroma description.
2. Infective endocarditis (IE)
2.1 Objectives, to determine:
-A correlation with the patient´s prior examinations
-Valve structures.
-Anomalous densities that could represent an endocarditis focus.
2.2 Protocol/CTA planning
a. Arterial phase scan acquisition covering heart anatomy from the middle aortic arch. No pre-i.v.contrast cardiac imaging is obtained
b. Venous phase scan acquisition: Coronary CTA protocol with same anatomic coverage, 70-80 seconds after injection
For this study, a unique injection system is used, 80-100ml of iodinated contrast with a second injection with 30 ml of saline. Beta-blocker is carefully administered when necessary.
2.3 Findings
Due to its spatial resolution and contrast capabilities, cardiac CT is an accepted complementary tool to echocardiography ( TTE-TEE ) and Nuclear Medicine (PET) examinations.
Main cardiac CTA findings:
· Vegetations: well depicted with TTE-TEE, can be observed as filling defects attaching to valves or cavity walls (Fig.9)
· Paravalvular abscess: soft tissue density, mainly hypodense with peripheral enhancement in the venous phase. (Fig.10)
· Paravalvular leak: filled contrast space outside the margin of a prosthetic valve annulus, creating anomalous communication between cavities (Fig.11).
· Pseudoaneurysm: simple or multiloculated focal outpouching of contrast material, in perivalvular región (Fig.12)
· Leaflet perforation. Better depicted with cardiac echocardiography .
· Peripheral findings with additional scans. Secondary lung lesions or perfusion defects in abdominal viscera ( Fig.9, right).
Sometimes follow up CTA is required, in order to confirm changes or progression, especially in cases of a new pseudoaneurysm, as well as correlation with PET-CT studies (Fig.13).
3. Thrombus/pannus
3.1 Objectives, to confirm
-The presence of soft tissue covering or attached to valvular structures.
-Reliable density measurements of observed lesions.
3.2 Protocol/CTA planning
a. Same protocol as coronary CTA protocol without previous non-contrast heart examination.
b. When thrombus in a heart cavity is suspected, a pre-contrast acquisition is obtained.
3.3 Findings
Valvular pannus ( Fig.14 ) is a well-known complication of aortic valve replacement. . Differentiation with thrombus ( Fig.15) is not always easy and is mainly related to the measured densities, suggesting pannus when higher than 145 UH and thrombus when lower tan 90UH.
Other conditions, like cardiac fibroelastoma ( Fig.16 ), can resemble the image of a thrombus.
Thrombus can also be observed in heart cavities as an attached filling defect.
4. Tricuspid valve procedures
4.1 Objectives
-To obtain well-opacified right chambers in CTA imaging, minimizing IV contrast streak artifact as much as possible (Fig.17).
-To obtain precise images of the right atrioventricular junction, so as to practice measurements.
4.2 Protocol/CTA planning
A modified cardiac CTA protocol is used, with an initial bolus of 65 ml of IV iodinated contrast at the rate of 4 ml/s, followed by a second bolus of 35 ml at 3 ml/s. 30 ml of saline is afterwards injected. ROI is positioned in the right ventricle´s central cavity before the de bolus-tracking scan.
A subsequent venous phase for peripheral veins' depiction, such as jugular vein access may be necessary.
4.3 Basic findings
As the tricuspid annulus is a 3D-shaped structure, the multiplanar capabilities of CTA turn out to be well-suited for this purpose. It is important to achieve data, such as:
- Diameter and the atrial inlet of both superior and inferior venae cavae.
- The angle between the venae cavae and the tricuspid annulus plane.
- Perimeter, area and orthogonal diameters of tricuspid annulus (Fig.18).
- Distance between the annulus and right coronary artery (Fig.19). It´s important to avoid coronary artery impingement during the interventional procedure.
5. Left atrial appendage percutaneous occlusion
5.1 Objectives
-To determine permeability/occlusion of the left appendage cavity after occlusion procedure.
-To assess the anatomy of left appendage (Fig.20) and pre-procedure absence of intracavitary thrombus.
5.2 Protocol/CTA planning
We use a cardiac CTA protocol with no prior non-contrast study. Both the arterial phase CTA and the subsequent venous phase scan, are obtained with the patient in left lateral decubitus.
5.3 Findings
An alternative to anticoagulation in patients with atrial fibrillation is percutaneous procedures, using left atrial occlusion devices. The main findings are collected:
- Areas of persistence/absence of IV contrast filling in the left appendage cavity after occlusion procedure (Fig.21). Adherence of discs.
- Morphologic type and dimensions of the appendage cavity in pre-procedure studies. ( Wang´s classification ).