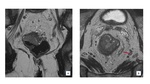
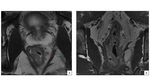
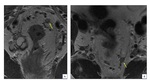
Importance of EMVI in prognosis:
The prognosis in colorectal cancer is predicted by the extent of the local tumor spread (T), the involvement of the lymphatic system (N), and/or metastasis to other organs (M) that are incorporated in TNM staging [13].
(Fig 6).
The survival rate of rectal cancer patients depends on the disease stage and the status of surgical margins, nevertheless, new features, such as venous invasion, perineural invasion and tumor grade also have prognostic value. Currently, great importance has been given to EMVI.
Beyond these standard staging criteria, EMVI is a crucial predictor of tumor recurrence or metastasis, which is an independent indicator of poor prognosis in colorectal carcinoma[14].
Although it does not influence the overall tumor stage, the presence of EMVI does give high-risk disease status.
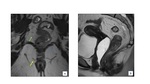
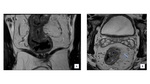
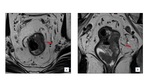
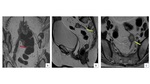
Venous invasion allows tumor cells to embolize through the hematogenous spread. As a result, distant metastasis in rectal cancer, via the portal circulation, is formed. (Fig 7).
EMVI is an independent prognostic predictor of unfavorable results in rectal cancer such as local tumor recurrence, synchronous and metachronous distant metastases, and increased mortality[15].
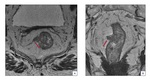
The identification of EMVI before surgery can support the patients triaging process towards preoperative CRT, selecting which patients will get benefits from the neoadjuvant treatment[16]. (Fig 8).
Anatomy of rectum drainage:
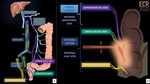
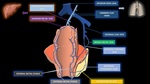
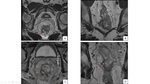
Rectum and anus drainage occurs via both the portal and systemic systems by the superior, middle and inferior rectal veins. (Fig 9 and Fig 13).
There are many anastomoses between these vessels. The rectal venous plexus consists of two parts:
(1) an internal rectal, immediately the rectal epithelium;
(2) an external rectal, external to the muscle layers of the rectum wall [17]. (Fig 10).
MRI protocol:
Recent studies have addressed features and technical aspects that are important or not in EMVI detection[18]. (FIG 11).
Pitfalls:
MRI has restricted accuracy in the identification of extramural and intramural vascular invasion in vessels smaller than 3 mm, in which tumor signal may not be identifiable.
EMVI misinterpretation as an enlarged lymph node, and vice versa, is a potential source of error. However, the multiplanar capability of MRI should enable radiologists to follow the suspicious lesion in different planes, resulting in a more accurate distinction.
Exuberant peritumoral inflammatory reactions can simulate tumor invasion and produce potential false-positive EMVI in rectal cancer.
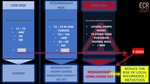
Scoring system of EMVI:
There is a MRI extramural vascular invasion (EMVI) scoring system which is the most best-defined criteria in EMVI graduation[19]. (Fig 12).