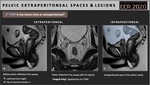
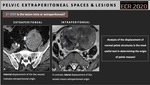
1st STEP: Is the lesion intra or extraperitoneal?
· The pelvis is divided into extra-peritoneal and intra-peritoneal spaces by the anterior peritoneal reflection line.
· This line can be identified on T2-weighted images in the midsagittal plane as a thin hypointense line of
· The tip of the seminal vesicles in men and uterocervical angle in women are anatomical landmarks for the most inferior point of the peritoneal membrane (Fig.2).
· Analysis of the displacement of normal anatomic structures is one of the most useful tools in determining the origin of pelvic masses (Figs.3-6)
2nd STEP: In which retroperitoneal space is it localized?
· The pelvic extraperitoneal space include 3 intercommunicating potential spaces: Prevesical space/ Space of Retzius, Paravesical space and Perirectal space (Figs.7-13)
3rd STEP: What is the composition of the lesion? (Fig.14)
1. CYSTIC LESIONS
1.1 TAILGUT CYST
· Most common presacral lesion incidentally found in adults
· Congenital lesions - incomplete regression of a portion of the gut distal to the yet undeveloped anus
· ++ middle-aged women
· Presacral space or ischioanal fossa
· Well-defined,thin-walled, often multilocular cystic lesions (Fig.15)
· Without any internal enhancement
· Thick enhancing walls or air-fluid levels suggest infection
· Treatment of choice is surgical excision due to the risk of malignization
1.2 DERMOID CYST
· Mature teratoma - contains elements derived from at least 2 of 3 embryological layers
· Most common presacral mass in children, ++women
· CT and MRI depict a well-circumscribed complex lesion containing fat and calcifications
· The presence of hypoattenuating fat within the cyst and/or wall calcifications are suggestive features (Fig.16)
1.3 CYSTIC LYMPHANGIOMA
· Rare, congenital lesions that may be found at any age
· Failure of communication between the pelvic and the main lymphatic channels
· Pelvic location is uncommon (95% in the head and neck)
· CT/ MRI: Uni/multilocular cystic lesions, well-defined and thin-walled. Calcifications are rare (Fig.17). No significant enhancement
· Classically cross more than one anatomical compartment, reflecting the pathway of developing lymphatic vessels
1.4 LYMPHOCELE
· Occur in 12-24% of patients after pelvic lymphadenectomy or renal transplantation
· CT and MRI reveal a thin-walled, unilocular cyst (Fig.18)
· Negative attenuation values can be seen due to the presence of fat are highly suggestive
· Wall calcifications on long-standing lesions
2. SOLID LESIONS
A. FAT-CONTAINING - These lesions demonstrate fatty attenuation on CT, high signal intensity on T1WI and T2WI MRI images an loss of signal on fat-saturated sequences
2.1 LIPOMA/ LIPOSARCOMA
LIPOMA
· Benign tumor composed of mature adipose tissue
· Well-defined, homogeneous (Fig.19-20)
LIPOSARCOMA
· Malignant counterpart
· Prominent solid soft-tissue component or adjacent organ invasion should raise suspicion for liposarcoma
· Imaging appearances vary depending on the tumor grade (Fig.21)
2.2 ENCAPSULATED FAT NECROSIS
· There is no local invasion and only minimal mass effect on surrounding structures (Fig.22)
2.3 EXTRAMEDULLARY HEMATOPOIESIS
· Benign masses of hematopoietic tissue outside the marrow can arise in patients with leukemia, thalassemia or anemia
· Multiple sites of involvement (Fig.23)
2.4 TERATOMA
· Germ-cell tumor containing tissues derived from one or more embryonic layers. Can be benign or malignant.
· ++children
· Variable imaging appearances– cystic to solid, may contain fat and calcium
· Fat-fluid levels are common (Fig.24)
B. Myxoid stroma - Hypointense on T1WI and hyperintense on T2WI images. The degree of enhancement after contrast administration depends on the extent of vascularization within the stroma.
2.5 SCHWANNOMA
· Most common tumor of peripheral nerves
· ++young to middle-aged women
· CT: well-defined hypoattenuating mass. Areas of cystic degeneration, hemorrhage or calcification can also be seen.
· MRI: heterogeneously low signal intensity on T1 and high signal intensity on T2WI
· A“target-like” pattern consisting of peripheral high signal and central low signal intensity can be seen on T2WI
· Contrast enhancement varies depending on the cellularity and presence of degeneration (Figs.25-26)
2.6 GANGLIONEUROBLASTOMA
· Transitional tumor on the intermediate spectrum of disease between ganglioneuroma-neuroblastoma
· ++ children
· Imaging can be variable and range from solid, well-marginated paraspinal masses with homogeneous enhancement to irregular, infiltrative masses with cystic degeneration
· MRI: usually low-signal on T1WI and high-signal on T2WI (Fig.27)
· Variable enhancement
2.7 NEUROFIBROMA
· Multiple tumors can be seen in patients with NF-1. Typically bilateral and symmetrically plexiform neurofibromas
· MRI: Homogeneous, isointense to mildly hyperintense relative of the muscle on T1WI
Hyperintense rim of myxoid stroma and central zone of low attenuation due to the fibrous core giving rise to the “target sign” on T2WI (Fig.28)
2.8 MYXOPAPILLARY EPENDYMOMA
· Most common intramedullary spinal cord tumor in adults
· Large destructive sacral mass, invading the spinal canal and adjacent soft-tissues
· MRI: isointense relative to spinal cord on T1WI and hyperintense on T2WI (Fig.29)
C. Fibrous tissue - Typically have soft-tissue attenuation values on CT, low-signal intensity on T1 and T2-weighted MR images and display delayed enhancement after contrast administration.
2.9 DESMOID TUMOR
· ++females, 3rddecade
· May be associated with FAP and Gardner Syndrome
· Imaging appearance is variable depending on internal contents and degree of vascularity (Fig.30)
2.10 LEIOMYOMATOSIS
· Diffuse leiomyomatosis is extremely rare. Characterized by multiple leiomyomas growing along the submesothelial tissues of the peritoneum
· Not “truly” extraperitoneal in origin but can involve extraperitoneal spaces such as the space of Retzius
· MRI: multiple masses with similar intensity to smooth and skeletal muscle on T1WI and T2WI
· Homogeneous enhancement(Fig.31-32)
2.11 LEIOMYOSARCOMA
· 2ndmost common retroperitoneal sarcoma
· ++ women, 5th-6thdecades of life
· Large tumors are heterogenous with areas of necrosis and hemorrhage
· MRI: heterogeneous iso-hyperintensity on T2WI; restriction at DWI and heterogeneous enhancement (Fig.33)
· In contrast to other sarcomas generally do not have calcifications
2.12 MALIGNANT FIBROUS HISTIOCYTOMA
· 3rdmost common retroperitoneal sarcoma
· ++ males, 5th-6thdecades of life
· CT and MRI appearances are nonspecific
· Large, infiltrating, heterogeneously enhancing mass with areas of necrosis and hemorrhage that involves adjacent organs (Fig.34)
· Peripheral calcifications in 7-20%
D. Vascularized tissue
2.13 RECTAL ANGIOMATOSIS
· Rare vascular malformation consisting of vascular lakes growing in the rectal wall and infiltrating the surrounding tissues
· Young individuals + history of rectal bleeding
· MRI:thickened rectal wall with high signal on T2WI associated with infiltration of peri-rectal fat (Fig.35)
2.14 SOLITARY FIBROUS TUMOR
· Usually benign
· Middle-aged adults
· Well-defined solitary mass with soft-tissue attenuation
· Intense enhancement on arterial phase and/or visible blood vessels (Fig. 36)
· Hyperintensity persists on the late phase- fibrous component
· Flow voids are common
2.15 PRIMARY PELVIC RETROPERITONEAL GIST
· Rarely can arise in extra-intestinal locations - mesentery, omentum, retroperitoneum
· Pelvic extraperitoneal GISTs are rare and aggressive with a higher rate of malignancy
· Large, hypervascular masses with areas of necrosis, hemorrhage and cystic degeneration (Fig.37)
· Differentiation from other solid hypervascular tumors is not possible solely based on imaging
E. Miscellany
2.16 SMALL ROUND-CELL TUMORS
· SRCT is a group of malignant neoplasms with unknown origin that occur in young patients
· Composed of primitive small round blue cells
· Include PNET, Ewing’s and Neuroblastoma (Fig.38)
· CT and MRI reveal heterogeneous bulky masses with areas of hemorrhage or necrosis
· Heterogenous enhancement
· Poor prognosis
2.17 PLASMACYTOMA
· 80% of extra-medullary plasmacytomas occur in the head/neck
· Retroperitoneal location is rare
· At imaging they appear as large, soft-tissue masses that compress adjacent structures
2.18 SPLENOSIS
· ++ males, history of traumatic splenectomy
· CT/ MRI: follows pattern of signal and enhancement of the spleen (Fig.40)
· Nuclear scintigraphy with Tc-99m sulfur colloid or damaged RBCs nuclear medicine scan are the choice
2.19 INFECTIOUS/ INFLAMMATORY
· Retrorectal pyogenic abscesses or fistulas often result from post-operative alterations or perianal IBD (FIg.41)
4th STEP: What is the enhancement pattern of the lesion? (Fig.42)
5th STEP: What is the pattern of spread of the lesion? (Fig.43)
6th STEP: Are there any characteristic imaging findings suggesting a specific diagnosis? (Figs.44-45)
7th STEP: Clinical context assessment (Fig.46)