Imaging Features
Imaging appearances vary depending on the extent of inflammation and presence of complications.
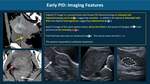
Early PID - uncomplicated or cervicitis/endometritis/oophoritis (Fig. 3)

Fig. 3: Early PID - Imaging Features
Normal imaging does not exclude the diagnosis in the correct clinical scenario. When present, features are non-specific and are those of generalised pelvic inflammation [3], which include:
- Broad ligament thickening
- Pelvic free fluid
- Pelvic fat stranding/heterogeneity
- Reactive lymphadenopathy - particularly along the gonadal veins into the para-aortic region
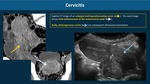
- Cervicitis - enlarged cervix with enhancement of the endocervical canal reflecting hyperaemia (Fig. 4)
- Endometritis - enlarged uterus with indistinct contour, abnormal endometrial enhancement and fluid (Fig. 5, Fig. 6)
- Oophoritis - enlarged, oedematous ovaries with peripherally displaced follicles and intra-ovarian collections (Fig. 7)
- Peritonitis
Helpful clues include the presence of an IUD and evidence of recent surgery.
Pyometra
Pus-filled endometrial cavity [4], which may be of increased T1w signal and restricted diffusion on MRI (Fig. 8). This is an important finding to convey to the clinical team as patients can decompensate acutely when pyometra is drained.

Fig. 8: Pyometra
Salpingitis/Pyosalpinx
Salpingitis: Swollen fallopian tube with mural inflammation as the predominant feature (Fig. 9).

Fig. 9: Salpingitis
Pyosalpinx: Pus within a dilated fallopian tube [5] with associated inflammation (Fig. 10).

Fig. 10: Pyosalpinx - US and CT
Imaging features on ultrasound, CT and MRI are:
- Thickened and dilated tubular pelvic structures > 5mm
- Multiplanar reformats on CT help to detect the tubular nature of the structure and assess its origin (Fig. 11)
- Contents can be simple/hypoechoic or heterogenous, sometimes with low-level internal echoes on ultrasound due to complex/proteinaceous material
- ‘Waist sign’ - incomplete linear indentations indicate a tubular structure
- ‘Cogwheel’ sign - longitudinal endosalpingeal folds have a cogwheel appearance in cross-section
- Beads on a string sign - small echogenic mural nodules (2-3 mm) are suggestive of chronic salpingitis
- Mural hyperenhancement following contrast administration on CT and MRI
- Fluid-debris levels and gas may be seen on CT
- Tubal contents and wall can demonstrate restricted diffusion [6] on MRI (Fig. 12)

Fig. 12: Pyosalpinx - MRI
Tubo-ovarian abscess
Ultrasound (Fig. 13)
- Multilocular complex retrouterine/adnexal mass with heterogeneous internal contents, septations and thickened wall
- Adjacent fluid or echogenic debris in pelvis

Fig. 13: Tubo-ovarian Abscess
CT (Fig. 14)
- Low attenuation inflammatory masses with loss of the normal adnexal structure
- May contain fluid-fluid levels or gas (which is highly suggestive)
- Often multiloculated with thickened enhancing walls and ‘incomplete’ septae

Fig. 14: Tubo-ovarian Abscess
MRI (Fig. 13)
- Thick walled pelvic masses
- Abscess contents are typically low on T1w and heterogenous or hyperintense on T2w imaging (variable depending on haemorrhagic and protein content)
- Septal and rim enhancement and diffusion restriction
- Restricted diffusion of the purulent content of the mass
Actinomycosis (Fig. 15)
- Chronic suppurative infection caused by Actinomyces israelii
- Increased prevalence with IUD
- Nonspecific imaging features:
- Solid enhancing granulation tissue with fibrosis and thickening of fascial planes [7]
- Extension across fascial planes into the pouch of Douglas, perirectal and pre-sacral region is characteristic
- Small rim-enhancing abscesses relating to solid parts of masses is suggestive

Fig. 15: Actinomycosis
- Definitive diagnosis requires microbiological confirmation and laparoscopy may be required for diagnosis if tissue not amenable to biopsy
Tuberculosis (Fig. 16, Fig. 17)
- Mycobacterium tuberculosis is the causative organism, more prevalent in patients with HIV
- Dissemination through the genital tract is usually via haematogenous or lymphatic spread, occasionally by peritoneal dissemination
- Tuberculous tubo-ovarian lesions may be small or inconspicuous compared with abscesses formed by more conventional organisms
- Often accompanied by tuberculous peritonitis which can mimic peritoneal carcinomatosis [7]:
- Thickening and nodularity of peritoneal reflections and around pelvic organs
- Dense ascites
- Omental infiltration
- Calcifications (uncommon acutely)
- Necrotic lymph nodes suggest tuberculous lymphadenitis

Fig. 17: Peritoneal Tuberculosis
Complications
Early complications include:
- Hydronephrosis (Fig. 18) - inflammation adjacent to lower ureters causes dilated pelvicalyceal system and ureters
- Ileus (Fig. 19) - bowel dilatation without a transition point
- Ovarian vein thrombosis (Fig. 19) - patients typically present with fever and back pain
Long term complications include:
- Chronic pelvic pain - inflammation results in scarring and adhesions (up to a third of women with PID)
- Subfertility (Fig. 20) - inflammation causes loss of ciliated epithelial cells along the fallopian tubes resulting in impaired ovum transport (some studies suggest a 5x increase in subfertility with a history of PID)
- Ectopic pregnancy - due to fallopian tube damage (up to 8.5% of patients with previous PID develop ectopic pregnancies, compared with background rate of approximately 1.3%)
- Adhesions - not typically visible on imaging however CT can detect adhesion-related complications, principally bowel obstruction and hydrosalpinx.
Perihepatitis/Fitz-Hugh-Curtis (Fig. 21)
- Inflammation of the liver secondary to PID [8], typically N. gonorrhoea or C trachomatis
- Inflammatory stranding and fluid along the right paracolic gutter and perihepatic region
- Abnormal enhancement of the peripheral liver, gallbladder wall thickening and pericholecystic inflammation, transient hepatic perfusion abnormalities
- Differentiate from peritoneal carcinomatosis by assessing for peritoneal nodularity and a solid component as well as correlating with clinical presentation

Fig. 21: Complications: Fitz-Hugh-Curtis
Differential diagnosis of PID on imaging
There are many causes of gynaecological pelvic pain including ovarian torsion and ectopic pregnancy, however, the following differentials should be considered in women with tubal dilatation/pelvic collection or abscess:
1. Benign gynaecological:
- Endometriosis (Fig. 22, Fig. 23) - the following signs favour this diagnosis:
- Blood in tubes, pelvic adhesions [9]
- Minimal peritoneal enhancement
- Dense fibrotic adhesions (dark)
- Adenomyosis

Fig. 22: Differential Diagnosis: Endometriosis
- Rare: infected, pus-filled fibroid

Fig. 24: Differential Diagnosis: Pyomyoma
2. Non gynaecological sources of pelvic infection / inflammation (Fig. 25, Fig. 26)
- Deep pelvic abscesses caused by diverticulitis or appendicitis
- Important to evaluate bowel wall and check appendix
- Look for epicentre of inflammatory process as gynaecological organs can become secondarily involved

Fig. 25: Differential Diagnosis: Pyosalpinx versus Appendicitis
3. Gynaecological malignancy (Fig. 27, Fig. 28)
- Typically patients are of a different age range but there is overlap. Fallopian tube cancer can be differentiated from PID by:
- Presence of enhancing soft tissue components
- Significantly elevated Ca-125
- Disseminated peritoneal disease
- Irregular peritoneal enhancement (vs smooth in PID)

Fig. 27: Differential Diagnosis: PID versus Malignancy
Management
Primary management of PID is medical, with antibiotic therapy according to local policies. This is all that is required in the majority of cases.
Interventional radiology has a role in drainage of tubo-ovarian or pelvic abscesses and can be considered in cases which are refractory to medical treatment [10]. It has the benefit of being minimally invasive and is frequently highly successful (Fig. 29).

Fig. 29: Image-guided Intervention
Surgical resection is reserved for difficult-to-drain tubo-ovarian complexes, but in itself can be challenging due to inflammation and adhesions.