1- ANATOMY OF THE OPTIC NERVE:
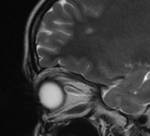
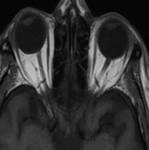
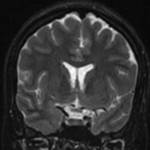
The optic nerve are the second pair of cranial nerves and they represent an extension of the central nervous system, it’s formed by axons of the retinal ganglion cells which become myelinated by oligodendrocytes as they leave the optic disc. The optic nerve can be divided into four segments:
•Intraocular: when it emerges through the scleral opening
•Intraorbital: the longest segment, communication between subarachnoid space around the optic nerve with that in suprasellar cistern
•Intracanalicular: passes through bony optic canal along with ophthalmic artery
•Prechiasmatic: Also called cisternal, intracranial segment in
suprasellar cistern.
Both nerves join to form optic chiasma, where the nasal fibers from each optic nerve decussate and temporal fibers do not decussate, then from the chiasm emerge the optic tracts.
The optic nerve is surrounded by the meninges which form an extension of the subarachnoid space containing cerebrospinal fluid.
2-HOW TO EXLORE THE OPTIC NERVE , PROTOCOLE:
-Axial and coronal T1 w sequence.
-Axial and coronal Short tau inversion recovery (STIR) or T2 FAT saturated.
-Oblique sagittals/ sagittals.
-Gadolinium enhanced sequence on T1 fat saturated sequence : Axial and coronal.
-We add Diffusion , Cerebral FLAIR / SWI and medullar imaging for associated central nervous system (CNS) lesions and etiological approach.
The intraorbital optic nerve and its surrounding cerebrospinal fluid are best seen on heavily T2 w or STIR images.
3-Imaging findings :
-A normal optic nerve is isointense to white matter on all sequences and shows no enhancement on T1 w images after injection of Gadolinium.
We consider an optic nerve as pathological according to this findings:
- Thickening or atrophy of the optic nerve compared to the unaffected controlateral nerve.
- High signal in T2 weighted sequences a result of oedema , inflammation and demyelinisation. We can also find enhancment of optic nerve on fat-supressed T1 weighted MRI after intravenous due to a blood-ON barrier breakdown.
- Hyperintensity on Flair sequence.
- Enhancment of optic nerve on fat-supressed T1 weighted MRI after intravenous due to a blood-ON barrier breakdown.
-It's important to determine the extent of the demyelinating lesions and which segments of the optic nerve are involved also involvment of the chiasma and optic tracts must be looked for
-It's important to point out that The abnormal gadolinium enhancement is not specefic in demyelinating optic neuritis as it can be found in neoplasic infiltrations, sarcoidosis and infecteous diseases.
4-Etiological approach through imaging :
Idiopathic optic neuritis: Isolated optic neuritis episode that require excluding any systemic or inflammatory disease.Possibility of recurrency and frequent recurrencies increases the riskof eventually developing MS or NMO.Any imaging pattern is possible wether short/long lesions , anterior or posterior location and chiasma/optic tracts might be affected.
ON in multiple sclerosis: Unilateral in general, less common bilatéral neuritis. The hypersignal and enhancement preferably affects the orbital segment of the optic neuritis especially in it's posterior part. Canalicular segment and prechiasmatic can be affected. Chiasma envolvement is not common but described.
ON in neuromyelitis optica disease spectrum (NMODS): Higher rate of bilateral neuritis, the hypersignal and enhancement can be more extensive than the multiple sclerosis. Intracranial segment is preferably affected in NMODS and involvement of optic chiasma and tracts is very suggestif of NMO.
5-What is not Optic neuritis ?
-Perineuritis :
The optic nerve is surrounded by the meninges which form an extension of the subarachnoid space containing cerebrospinal fluid. Pathologic conditions involving the subarachnoid space may easily spread along the intraorbital optic nerve. •Inflammation or infiltration of the meningeal sheath of optic nerve, the enhancement of the meningeal perinerve surrounding the ON.
-Optic nerve Glioma
-Optic nerve sheaths meningioma
6-Prognosis :
long-term visual outcome of ON is generally favorable, about one in three patients remains visually impaired •Very long Gd enhancing lesions as well as T2 lesions were associated with a significant loss of visual acuity. •the longer the T2 or Gd enhancing lesion on MRI, the poorer the visual acuity and recovery after treatment.
Lesion of the intracanalicular nerve seem correlated with a much significant vison loss : Solid bony canal my add a compressive component Visual acuity loss is more significant in NMOSD than MS.