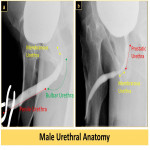
- Male Urethra Anatomy (Fig. 1)
The male urethra is divided into two parts:
- Anterior part which consists of the penile and bulbar urethrae.
- Posterior part which consists of the membranous and prostatic urethrae.
- URETHROGRAPHY Technqiues
2.1 Retrograde urethrography:
Urethrography is performed by using either Foley’s catheter or Knutson penile clamp.
2.1.1 Foley’s catheter technique (Fig. 4):
- Explain all the procedure steps to the patient and reassure him about the discomfort that he might experience.
- Clean the penis and the surrounding area with iodine and then place a sterile drape.
- Place the patient in supine oblique position (about 45o).
- Flush the patency of Foley’s catheter before using it, and test the inflating balloon.
- Administer a few milliliters of local anesthetic gel into the urethra via syringe.
- Insert the Foley’s catheter a few centimeters into the urethra until the balloon reaches the fossa navicularis then inflate the balloon using a few milliliters of normal saline until the catheter is secured (must ensure not to exceed the maximum capacity of the balloon). Before the inflation, reassure the patient about the discomfort he will experience.
- Under fluoroscopic guidance, inject 20 – 30 mL of iodinated contrast media and observe the filling of the anterior urethra.
- Once the urethra is satisfactorily opacified and distended with contrast material, spot radiograph should be obtained (normally, the contrast will be seen passing freely into the posterior urethra and urinary bladder).
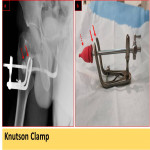
2.1.2 Knutson penile clamp (Fig. 2):
- This device is used in our department, it is a metallic device with a rubber cone-shaped tip that is placed in the external urethral orifice gently without causing an injury.
- After inserting the tip of the rubber cone into the urethra and securing the clamp externally around the penile shaft, we proceed with the same steps as above in the Foley catheter protocol.
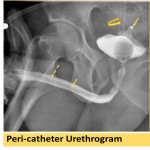
2.1.3Peri-catheter Urethrogram (Fig. 3)
This technique is used to examine the integrity and patency of the urethra when it already has an indwelling Foley catheter. Usually, it is performed to assess urethral healing after urethroplasty or to exclude urethral injury after pelvic trauma, and to decide whether the Foley catheter can be removed. If contrast material extravasation from the urethra is noticed, this means that there is incomplete healing and the removal of the Foley catheter should be delayed.
It is accomplished by using small size catheter placed next to the existing Foley catheter, and the external urethral opening is secured either by tying wet gauze around the glans of penis or squeezing the wet gauze around the tip of the glans penis to avoid external spillage of contrast (note: meticulous collimation is needed to avoid extra-radiation dose to the operator).
Important points to keep in mind:
- If resistance is encountered at the external urethral sphincter, which will prevent filling of the posterior urethra, lifting the penis to an approximately 90-degree angle and applying gentle and slow pressure should be considered to overcome the resistance.
- It is important to localize the bulbomembranous junction. It is located 1 – 1.5 cm distal to the inferior margin of the verumontanum (which is identified as an oval filling defect in the posterior part of the prostatic urethra).
2.2 Anterograde urethrography (Voiding cystourethrography) :
Voiding cystourethrography is the study of choice to assess the male posterior urethra (Fig. 1).
During this procedure, the urinary bladder is filled with iodinated contrast material. This is done by either suprapubic catheter or transurethral catheter. After that, patient passes urine under fluoroscopic guidance and spot radiographs are taken during active voiding.
- PITFALLS:
The radiologist should be aware of the following pitfalls that mimics pathologies while in fact not.
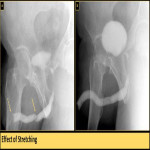
- Folded urethra can mimics focal stricture which can be avoided by adequate stretching of the penis (Fig. 4)
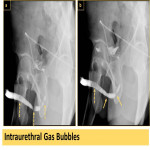
- gas bubbles can be introduced during insertion of the Foley or contrast injection (Fig. 5)
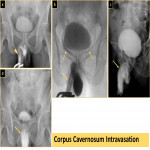
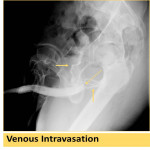
- contrast intravasation which can occur with increased luminal pressure in the setting of fragile or disrupted mucosa (Fig. 6 & Fig. 7). Gentle contrast injection is advised.
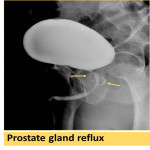
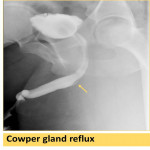
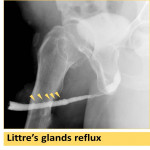
- contrast reflux into the prostatic glands (Fig. 8), Cowper’s gland ducts (Fig. 9), litters gland (Fig. 10).
- Traumatic urethral injury:
In cases of trauma, if urethral injury is suspected or in case of finding blood at the urethral meatus, we should do urethrogram to demonstrate any traumatic urethral injury, and if demonstrated, we proceed with suprapubic catheterization. We should avoid doing blind catheterization of the urethra in such cases.
Traumatic urethral injury can be due to blunt or penetrating injuries including pelvic trauma in motor vehicle accidents, pelvic fractures, gun shot or knife wound.
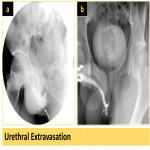
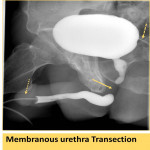
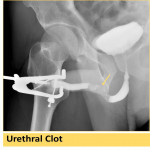
Findings of urethral injury include extravasation (Fig. 11), complete transection (Fig. 12), or if there is significant bleeding urethral clots may be visualized (Fig. 13).
Iatrogenic urethral injury can also happen post instrumentation, urethroplasty (Fig. 14), or tumor resections (Fig. 15).
- Strictures of the Urethra:
Strictures occur due to fibroblast and collagen proliferation leading to fibrous scarring of the urethra.
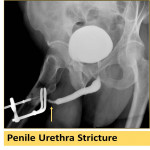
Anterior urethral strictures (Fig. 16 & Fig. 17) are usually due to inflammatory (infectious urethritis), traumatic (straddle trauma or iatrogenic instrumentation) or congenital causes.
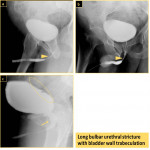
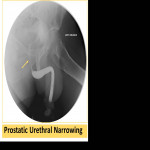
Posterior urethral strictures are usually due to urethral disruption caused by surgery or trauma or it could be due to compression by prostatic hyperplasia (Fig. 18).
Retrograde urethrography is the primary method used to image anterior urethral stricture.
Antegrade/descending urethrography must be performed for proper distension of the posterior urethra. If posterior urethral strictures are suspected, we perform both antegrade cystourethrography and retrograde urethrography to estimate the length of the urethral defect accurately.
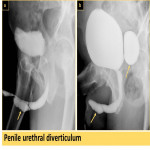
- Urethral diverticulum:
They are focal outpouchings of the urethra. Occur more commonly in women. The symptoms are usually dysuria, post-void dribbling and dyspareunia.
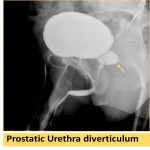
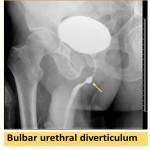
Can affect the bladder or any part of the urethra with multiple shapes, and may produce a mass effect (Fig. 19, Fig. 20, Fig. 21).
Usually diagnosed during voiding cystourethrogram, however MR imaging is currently more sensitive and becoming more popular.
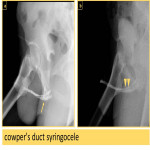
Cowper duct syringocele (Fig. 22) can mimic a diverticulum. It refers to cystic dilatation of the main duct of the bulbourethral glands (Cowper’s glands). It is difficult to differentiate between them, however, diverticulum usually presents with post void dribbling while symptomatic syringoceles usually cause obstructive symptoms.
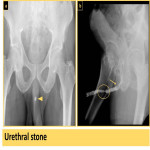
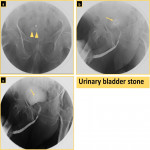
- Urethral and bladder stones:
Most urethral stones are originally formed in the urinary bladder and then migrate into the urethra during voiding.
Primary urethral stone formation rarely happens and is usually associated with urethral stricture or urethral diverticulum.
Retrograde urethrography will show a round-shaped filling defect in the urethra or bladder (Fig. 23 & Fig. 24).
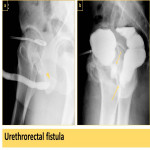
- Urethral fistulas:
Urethral fistulas are abnormal connections via tunnel like fibrous pathway between the urethra and surrounding structures.
Could be congenital or acquired due to trauma, surgery, or inflammation.
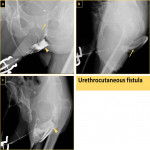
Examples include, urethrorectal (Fig. 25), urethrocutaneous (Fig. 26, Fig. 30), and urethrovaginal fistulas.
- Post-surgical changes:
Urethral and periurethral surgery will cause anatomical changes that will be reflected in the urethrogram. The operator should be aware of the operative history for proper interpretation.
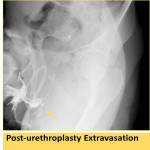
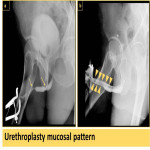
Urethroplasty will cause irregular mucosal outline of the reconstructed part of the urethra (Fig. 27).
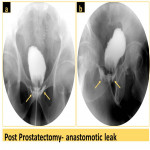
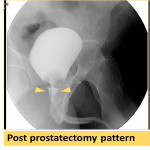
Prostatectomy will lead to loss of the prostate impression on the prostatic urethra which will be distended assuming the shape of the prostatic cavity (Fig 28).
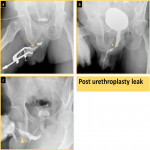
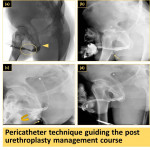
- The peri-catheter technique guides the post operative management course:
After urethral or periurethral surgery a Foley catheter is usually deployed for a period of time to divert the urine and support the healing of the tissues in the surgical field. In the absence of leakage or fistula on peri-catheter urethrogram we can remove the Foley catheter safely, however if there are complications, it should be kept for a longer period with further management steps until its resolution (Fig. 29 & Fig 30).