Abnormal embryonic pulmonary vein development may result in a wide spectrum of congenital anomalies [1], they are frequent in patients with congenital heart disease (CHD). The spectrum of findings can range from incidental findings to conditions that are lethal if left untreated. Accurate definition of the nature and extent of these abnormalities is critical for treatment decision making [2]. Abnormal pulmonary venous return was first described by Winslow in 1739 [3].
There’s a broad spectrum of pulmonary venous connections that deviate from the usual anatomical configuration and range from normal variant drainage to anomalous pulmonary-systemic communications. Patients can be asymptomatic or present with non-specific cardiorespiratory symptoms. Diagnosis can be difficult, missed, or only made at late clinical presentation in adulthood [4].
Several imaging modalities are used to assess the pulmonary veins, including chest radiography, echocardiography, magnetic resonance imaging (MRI), and computed tomography (CT). Multidetector CT is an excellent technique for this purpose and is currently available in many radiology departments worldwide. Transthoracic echocardiography has been used as the initial imaging modality for evaluation of pulmonary venous anomalies. However, owing to its small field of view and its dependance on operator technique and experience, it is not always possible to trace each pulmonary vein. CT excellently delineates vascular structures. Multiplanar and 3D reconstructed images superbly depict anomalous pulmonary venous structures. The primary disadvantage of CT is that it requires the use of ionizing radiation, although new submillisievert acquisition techniques are now being used [5]. The use of IV iodinated contrast material may adversely affect renal function or result in acute allergic-like reactions. Timing of the IV contrast bolus is critical because a suboptimally timed bolus may limit opacification of pulmonary venous structures. MRI can provide anatomical as well as functional assessment. There is no associated radiation risks and non-contrast acquisitions are possible. Recently many centers have started using MRI, yet, its widespread use is precluded by its limited availability, longer scan times and frequent need of sedation or general anesthesia [1,5,6,7,8].
Embryology of the pulmonary veins
During the first 2 months of embryological development the lung buds arises from the foregut and drain the systemic veins of the embryo. At the same time, an outpouching from the primitive left atrium forms a common pulmonary vein. When the buds fuse with the common pulmonary vein, the connections between the pulmonary veins and the systemic veins are obliterated; subsequently, the common pulmonary vein becomes incorporated into the left atrium so that two pulmonary veins remain, draining each lung. Altered absorption of these structures can result in abnormal venous caliber, increase or decrease in the number of veins, and abnormal drainage of pulmonary veins to systemic veins or the right atrium [7,8].
Normal pulmonary venous anatomy
The usual arrangement consists of four separate veins: right and left superior and inferior veins, which drain individually into the left atrium. The right superior pulmonary vein (RSPV) drains the right upper and middle lobes of the lung, and the right lower lobe is drained by the right inferior pulmonary vein (RIPV). The left superior pulmonary vein (LSPV) drains the lingula and left upper lobe, while the left lower lobe is drained by the left inferior pulmonary vein (LIPV)[4].


![Fig 2: Fig.2. Diagram demonstrating the normal anatomic variants of the pulmonary veins. L1, two separate ostia for the left pulmonary veins that are not separated by the atrial wall; L2, two separate ostia for the left pulmonary veins that are separated by the atrial wall; L3, the left lower PV drains into the left upper PV with a short (<1 cm) common segment; L4, the left lower PV drains into the left upper PV with a long (>1 cm) common segment; R1, two separate ostia for the right pulmonary veins, with the vein draining the RML joining the right upper PV and forming a short (<1 cm) common segment; R2, three separate ostia for the right-sided pulmonary veins; R3, two separate ostia for the right pulmonary veins, with the vein draining the RML joining the right upper PV and forming a long (>1 cm) common segment; R4, two separate ostia for the right pulmonary veins, with the vein draining the RML joining the right lower PV; R5, four separate ostia for the right-sided pulmonary veins, with two veins draining the RML; R6, common ostium for the right-sided pulmonary veins; R7, four separate ostia for the right-sided pulmonary veins, with a separate ostium for the vein draining the RML and an accessory right top PV that drains the apical segment of the RUL. The most common anatomic pattern is L1/R1, with a total of four pulmonary veins draining into the left atrium. LUL, left upper lobe; LLL, left lower lobe; RUL, right upper lobe; RML, right middle lobe; RLL, right lower lobe; RTPV, right top pulmonary vein; PV, pulmonary vein [17].©Department of Magnetic Resonance, Instituto Nacional de Cardiologia "Ignacio Chavez"/ Mexico 2022.](https://epos.myesr.org/posterimage/esr/ecr2022/160799/media/920248?maxheight=150&maxwidth=150)
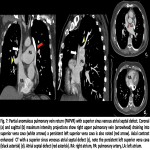
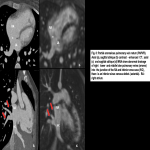
![Fig 10: Echocardiographic examination of the pulmonary veins.
[A-D] Transesophageal echocardiography of normal pulmonary veins. (A) Apical bicommissural 65º with visualization of the left atrial appendage (^), coumadin ridge (yellow arrow) and left superior pulmonary vein (*) assessed in 2D and color Doppler. (B) Middle esophageal at 117º with counterclockwise rotation with visualization of both left pulmonary veins (blue arrow). (C) Middle esophagus at 117º with clockwise rotation with visualization of both right pulmonary veins (green arrow). (D) Pulsed Doppler in the left superior pulmonary vein with reverse systolic flow due to severe mitral regurgitation.
[E-H] Transthoracic echocardiographic approximations of pulmonary veins with obstruction in the connection. (E) Modified 4-chamber apical with 4 dilated pulmonary veins and an image suggestive of a membrane at the level of the connection site with the left atrium (*) that conditions flow acceleration (aliasing) by color Doppler visualized in 4 and 2 chambers (F and G ), and corroborated by pulsed Doppler (H), with continuous venous flow reaching a peak gradient of 45 mmHg.
[I-L] Transthoracic echocardiographic approximations of TAPVR of the supracardiac variety. (I) Apical 4-chamber 2D with ostium secundum atrial septal defect. (J) Modified 4-chamber apical color Doppler image of the superior vena cava connected to the right atrium and pulsed Doppler assessment (K) showing continuous venous flow with a peak gradient of 21 mmHg. (L) 2D suprasternal approximation and color with dilated vertical vein (*) 30mm and its connection with the innominate vein (^).
[M-N] Transthoracic echocardiographic approximations of TAPVR intracardiac variety. (M) Apical 4-chamber view modified posteriorly, visualizing drainage from the coronary sinus (*) to the right atrium, with pulmonary veins connected to it (arrow). (N) Modified parasternal approximation of the inflow tract of the right ventricle, with color Doppler on the connection of the pulmonary veins to the coronary sinus and aliased flow.
[O-P] Transthoracic echocardiographic approximations of PAPVR, infracardiac variety. (O) Subcostal approximation with color Doppler, visualizing the right pulmonary vein connected to the inferior vena cava (^) with spectral flow by pulsed Doppler (P). © Echocardiography Department, Instituto Nacional de Cardiologia "Ignacio Chavez"/ Mexico 2022.](https://epos.myesr.org/posterimage/esr/ecr2022/160799/media/920256?maxheight=150&maxwidth=150)
