Abnormalities of the pulmonary veins are classified as: 1- anomalous pulmonary venous drainage, total anomalous pulmonary venous return (TAPVR) and partial anomalous pulmonary venous return (PAPVR); 2- Stenosis, atresia, cor triatriatum, secondary stenosis; 3- Other or abnormal number of pulmonary veins [2].
TAPVR consists in all four pulmonary veins draining into systemic veins of the right atrium with or without pulmonary venous obstruction. Systemic and pulmonary venous blood mix in the right atrium. TAPVR is generally classified into 4 anatomical subtypes: supracardiac, cardiac, infracardiac, or mixed. With the accumulation of experience in surgical treatment and intensive postoperative care, the outcomes of TAPVR have improved over time, with reported mortality rates consistently < 10%. This anomaly comprises 1.5% of all congenital heart defects [5,9, 10, 11, 12].
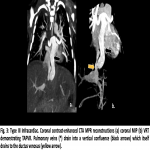
Type I: Supracardiac (55% of cases), the anomalous pulmonary veins terminate at the supracardiac level. Typically, four anomalous pulmonary veins (two from each lung) converge directly behind the left atrium and form a common vein, known as the vertical vein, that pass anterior to the left pulmonary artery and the left main bronchus to join the innominate vein.
Type II: Cardiac (30% of cases) involve a pulmonary venous connection at the cardiac level. The pulmonary veins join either the coronary sinus or the right atrium.
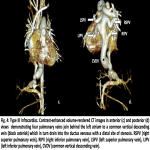
Type III: Infracardiac (13% of cases) involves a connection at the infracardiac level. The pulmonary veins join behind the left atrium to form a common vertical descending vein which usually joins the portal venous system, occasionally connects directly to the ductus venosus, hepatic veins, or inferior vena cava.
Type IV: Mixed (9% of cases), involves anomalous venous connections at two or more levels. In the most common pattern, the vertical vein drains into the left innominate vein, and the anomalous vein or veins from the right lung drain into either the right atrium or the coronary sinus [12].
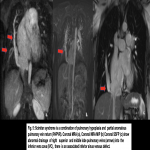
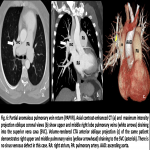
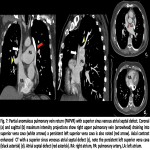
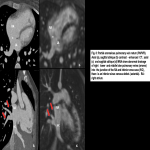
PAPVR is a congenital pulmonary venous anomaly that involves drainage of 1 to 3 pulmonary veins into the right-sided circulation, creating a partial left-to-right shunt. Scimitar syndrome is an example, in which an anomalous pulmonary vein descends from the right lung and drains into the inferior vena cava (IVC), right atrium, coronary sinus, azygos vein, portal vein, or hepatic vein. This condition is often associated with hypoplastic right lung, sequestration, CHD, diaphragmatic and musculoskeletal anomalies.
PAPVR has been reported to be twice as common in males than females, and more frequently arising from the right (90%) than left upper lobe (LUL) (10%). In addition, right upper lobe (RUL) PAPVR is associated with sinus venosus atrial septal defect (ASD) in 80% to 90% and ostium primum atrial septal defect in 10% to 15% of cases. It is presumed that ‘‘unroofing’’ of the right superior pulmonary vein into the SVC during development produces a combination of anomalous return and ASD. Anomalous veins generally connect to the nearest systemic vein or to the right atrium. On the right side, the most common drainage sites are the superior vena cava (SVC), azygos vein, right atrium, inferior vena cava (IVC), hepatic vein, and portal vein. On the left, connections include an anomalous vertical vein draining into the brachiocephalic vein, coronary sinus, or hemiazygos vein. Rarely, drainage may occur to the subclavian or subdiaphragmatic veins [14].
Pulmonary venous drainage into the coronary sinus occurs in about 3% of PAPVR, with left-sided pulmonary vein involvement seen more often than right sided. Patients may develop symptoms of right-sided volume overload or pulmonary hypertension [15,16].
Imaging evaluation of the pulmonary veins
Pulmonary veins usually drain into four separate ostia, many different anatomic variants have been described. The most common pattern is that of two separate ostia on the left, one superiorly, draining the left upper lobe, and one inferiorly, draining the left lower lobe; and two separate ostia on the right, one superiorly, draining the right upper and middle lobes, and one inferiorly, draining the right lower lobe. Radiologists should be familiar with the other anatomic variants, so that they can differentiate between a naturally occurring reduced number of ostia and a pulmonary vein occlusion [17].
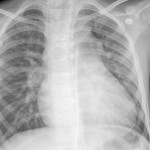
Chest radiography (CRx) is a widely available modality, the resolution of these anatomic structures is low and interpretation of the images requires training and experience. A classic sign is the "snowman-shaped heart” in supra-cardiac form, the confluence of pulmonary veins behind the heart drain to an ascending vertical vein (VV) which drains into the innominate vein, and eventually to the dilated right superior vena cava, together they make the head of the snowman, the lower part of snowman is made up of enlarged right-sided chambers [5, 6, 18].
In general, both CT and MR imaging depict the pulmonary vein anatomy well. Electrocardiographically gated cardiac CT should be used when detailed assessment of the pulmonary veins is needed, it should be timed for maximum contrast opacification of the left atrium, usually systole. Transesophageal echocardiogram is the most used tool for the evaluation pulmonary vein connection in adults and is seen in the middle esophagus. Modifications in the usual approach allow the user to evaluate the number of veins, their connection and their drainage, using a two-dimensional method, color and pulsed Doppler [19,20].

![Fig 10: Echocardiographic examination of the pulmonary veins.
[A-D] Transesophageal echocardiography of normal pulmonary veins. (A) Apical bicommissural 65º with visualization of the left atrial appendage (^), coumadin ridge (yellow arrow) and left superior pulmonary vein (*) assessed in 2D and color Doppler. (B) Middle esophageal at 117º with counterclockwise rotation with visualization of both left pulmonary veins (blue arrow). (C) Middle esophagus at 117º with clockwise rotation with visualization of both right pulmonary veins (green arrow). (D) Pulsed Doppler in the left superior pulmonary vein with reverse systolic flow due to severe mitral regurgitation.
[E-H] Transthoracic echocardiographic approximations of pulmonary veins with obstruction in the connection. (E) Modified 4-chamber apical with 4 dilated pulmonary veins and an image suggestive of a membrane at the level of the connection site with the left atrium (*) that conditions flow acceleration (aliasing) by color Doppler visualized in 4 and 2 chambers (F and G ), and corroborated by pulsed Doppler (H), with continuous venous flow reaching a peak gradient of 45 mmHg.
[I-L] Transthoracic echocardiographic approximations of TAPVR of the supracardiac variety. (I) Apical 4-chamber 2D with ostium secundum atrial septal defect. (J) Modified 4-chamber apical color Doppler image of the superior vena cava connected to the right atrium and pulsed Doppler assessment (K) showing continuous venous flow with a peak gradient of 21 mmHg. (L) 2D suprasternal approximation and color with dilated vertical vein (*) 30mm and its connection with the innominate vein (^).
[M-N] Transthoracic echocardiographic approximations of TAPVR intracardiac variety. (M) Apical 4-chamber view modified posteriorly, visualizing drainage from the coronary sinus (*) to the right atrium, with pulmonary veins connected to it (arrow). (N) Modified parasternal approximation of the inflow tract of the right ventricle, with color Doppler on the connection of the pulmonary veins to the coronary sinus and aliased flow.
[O-P] Transthoracic echocardiographic approximations of PAPVR, infracardiac variety. (O) Subcostal approximation with color Doppler, visualizing the right pulmonary vein connected to the inferior vena cava (^) with spectral flow by pulsed Doppler (P). © Echocardiography Department, Instituto Nacional de Cardiologia "Ignacio Chavez"/ Mexico 2022.](https://epos.myesr.org/posterimage/esr/ecr2022/160799/media/920256?maxheight=150&maxwidth=150)

![Fig 2: Fig.2. Diagram demonstrating the normal anatomic variants of the pulmonary veins. L1, two separate ostia for the left pulmonary veins that are not separated by the atrial wall; L2, two separate ostia for the left pulmonary veins that are separated by the atrial wall; L3, the left lower PV drains into the left upper PV with a short (<1 cm) common segment; L4, the left lower PV drains into the left upper PV with a long (>1 cm) common segment; R1, two separate ostia for the right pulmonary veins, with the vein draining the RML joining the right upper PV and forming a short (<1 cm) common segment; R2, three separate ostia for the right-sided pulmonary veins; R3, two separate ostia for the right pulmonary veins, with the vein draining the RML joining the right upper PV and forming a long (>1 cm) common segment; R4, two separate ostia for the right pulmonary veins, with the vein draining the RML joining the right lower PV; R5, four separate ostia for the right-sided pulmonary veins, with two veins draining the RML; R6, common ostium for the right-sided pulmonary veins; R7, four separate ostia for the right-sided pulmonary veins, with a separate ostium for the vein draining the RML and an accessory right top PV that drains the apical segment of the RUL. The most common anatomic pattern is L1/R1, with a total of four pulmonary veins draining into the left atrium. LUL, left upper lobe; LLL, left lower lobe; RUL, right upper lobe; RML, right middle lobe; RLL, right lower lobe; RTPV, right top pulmonary vein; PV, pulmonary vein [17].©Department of Magnetic Resonance, Instituto Nacional de Cardiologia "Ignacio Chavez"/ Mexico 2022.](https://epos.myesr.org/posterimage/esr/ecr2022/160799/media/920248?maxheight=150&maxwidth=150)
