Keywords:
Radiographers, Conventional radiography, Dosimetry, Dosimetric comparison
Authors:
�. Trožić, A. England, N. Mekis
DOI:
10.26044/ecr2022/C-15516
Methods and materials
Phantom Study
In the first part of the study, we determined which band did not produce visible artefacts on the acquired images when the adipose tissue was displaced. We simulated a patient with an antropomorphic phantom RS-13T with its back side facing the vertical stand. The first stage of obesity was simulated with catering lard wrapped in cling film. We placed it on the front surface of the phantom and secured it by wrapping the cling film around the phantom. We collected bands of four different materials - a training rubber band, a cotton cloth folded into a band, an elastic cotton bandage, and a thin triangular cotton bandage - to test which one did not produce visible artefacts on the images (Figure 1). The phantom with the attached fat anteriorly was placed in front of the wall stand detector. We then selected one of the bands and lifted the fat out of the field of view as much as possible. We attached both sides of the tape to the handles on the left and right sides of the wall stand to ensure that the tape remained in the same position during imaging. We repeated this for each band.
Clinical Study
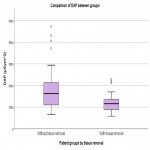
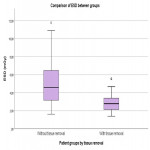
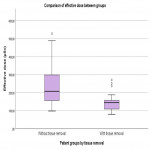
The second part of the study was performed to investigate whether image quality and radiation dose differ between images with and without adipose tissue displacement during erect pelvic radiography. This part of the study was performed on a total of 60 patients. Patients had to be 18 years of age or older, have a BMI of 25 or greater, be referred for the erect pelvic radiography and sign the informed consent form. If participants did not meet all inclusion criteria, they were excluded from the study. Patients were randomly divided into two equal groups - one of the groups manually displaced adipose tissue during imaging and the other did not.
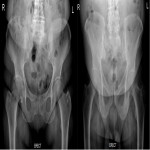
The patient stood in front of the wall stand detector and was prepared for erect pelvic X-ray. With both hands was holding the radiotransparent band and lifted the soft tissue as far as possible from the region to be examined. We recorded waist and hip circumference measurements (in one group of patients who had displaced soft tissue, these measurements were taken before and after displacement; in the other group, they were taken only once), dose area product (DAP), field size at the image receptor, source-to-skin distance, tube current and exposure time product (mAs), tube potential (kV), and patient height and weight (calculation of BMI). The entrance skin dose (ESD) and the effective dose (ED) were calculated subsequently.
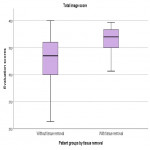
The obtained images were evaluated by three radiologists. They used a four-point scale for evaluation, with the number 4 representing a perfect/optimal image and the number 1 representing an inadequate image. On the images, they evaluated the visualisation of the hip joints, trochanters, sacroiliac joints, iliac crests, acetabula, pubic/ischial rami, femoral necks, medulla and cortex of the pelvis, sacrum and its foramina, and pelvic/hip soft tissues [7].