DEFINITION:
Nasal obstruction refers to the subjective sensation of reduced airflow through the nasal cavity and is reported to affect up to one-third of the population. It is a very common symptom, both at the primary care units and in patients referred to otolaryngologists with symptoms that are refractory to medical treatment.
IMAGING STUDIES:
- Computed tomography (CT) is usually performed in cases of inadequate response to medical treatment and persistent nasal obstruction. Besides, an imaging study (CT or MRI) becomes mandatory when some of the following "red flags" are present: persistent unilateral obstruction, epistaxis, pain, and orbital or neurological symptoms.
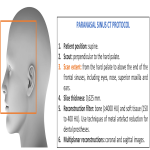
CT imaging of the paranasal sinuses has become the standard of care for preoperative planning. Helical CT allows for rapid acquisition and multiplanar reformations. Unenhanced axial images are typically obtained at 0.625 mm intervals, with reformatted images in the coronal and sagittal planes obtained at 1–2 mm intervals. Both high-resolution bone and soft-tissue algorithms should be obtained in all three imaging planes.
The nasal cavity should be evaluated from the nares to the nasopharynx. Multiplanar reconstructions are required for optimal assessment of the anterior nose, anterior skull base, congenital or acquired bony abnormalities of the posterior nose, mucosal hypertrophy and the detection of polyps.
- Magnetic resonance imaging (MRI) is combined with CT to improve the characterization of soft-tissue lesions and rule out orbital or neurological complications.
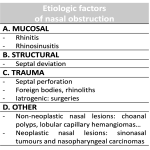
ETIOLOGIC FACTORS OF NASAL OBSTRUCTION:
The aetiology of nasal obstruction is mainly mucosal/physiological. Structural/anatomical causes are less frequent. The commonest mucosal causes are rhinitis (inflammation of nasal mucosa) and rhinosinusitis (inflammation of nasal and sinus mucosa).
A. MUCOSAL CAUSES
Allergic rhinitis is the commonest form of rhinitis, affecting up to 30% of adults. A careful history and anterior rhinoscopy are usually enough to make the diagnosis of allergic rhinitis. Nasal obstruction is also one of the commonest symptoms of chronic rhinosinusitis, which affects 14% of the adult population. The diagnosis is clinical, based on the duration of key symptoms for >12 weeks. Chronic rhinosinusitis may occur with or without polyps.
The most frequent imaging findings of rhinitis are diffuse nasal mucosal swelling, especially of the inferior turbinate. Polyps are uncommon, occurring in less than 2% of atopic patients.
Sinusitis does not usually occur without rhinitis. The exception is odontogenic sinusitis affecting mainly the maxillary sinus. There are three subtypes of chronic rhinosinusitis with both characteristic and overlapping clinical and radiological features:
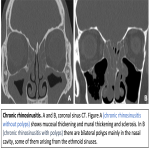
- Chronic rhinosinusitis without polyps: accounts for 60% of cases and is secondary to a combination of allergic, infectious and anatomical factors. Imaging signs include mucosal thickening, mural thickening and sclerosis, retention cysts and peripheral mucosal calcifications.
- Chronic rhinosinusitis with polyps: polyps usually are bilateral and associated with asthma, most commonly arising from the ethmoid sinuses. In severe cases, the opacified sinus drainage tracks and the nasal cavity are expanded with osseous demineralisation of the uncinate processes, ethmoid septa, lamina papyracea, bony septum, and middle turbinates. Unilateral inflammatory polyps are rare and suspicious of tumours, usually papilloma.
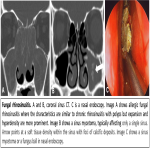
- Allergic fungal rhinosinusitis: defined as chronic rhinosinusitis with mucus containing eosinophils and fungal hyphae. These patients exhibit an intense allergic response to non-invasive fungal colonisation. The typical imaging characteristics are similar to chronic rhinosinusitis with polyps but expansion and hyperdensity tend to be more prominent. Loss of signal from the central sinus contents on T2 weighted images is also common.
B. STRUCTURAL CAUSES:
Septal deviation and turbinate hypertrophy are very common and the most frequent indications for endoscopic surgery in the treatment of nasal obstruction.
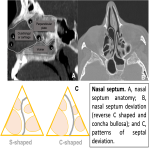
The nasal septum involves a single nasal cartilage (quadrangular cartilage) and two bones. The bony septum, consisting of the perpendicular plate of the ethmoid superiorly and the vomer inferiorly, divides the nasal cavity into two compartments, with an increase in the mucosal surface exposed to inspired air. The nasal septum must be studied from the nares anteriorly to the choanae posteriorly. The choanae separate the nasal cavity from the nasopharynx and correspond to the location of the posterior margin of the bony septum and turbinates.
The turbinates are three bony shelves covered by mucosa from the lateral nasal wall. The superior and middle turbinates are part of the labyrinthine portion of the ethmoid bone. The inferior turbinate is a separate bone projecting medially from the maxilla. It is the biggest turbinate and functionally the most important.
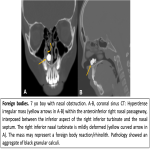
- Septal deviation increases with age. Small anterior deviations, which narrow the nasal valve, can lead to significant nasal obstruction while greater deviations in the posterior region of the nasal cavity may have no effect. The common patterns of SD are described as being C-shaped or S-shaped in the axial and coronal planes. Pneumatisation and growth of the middle turbinate (concha bullosa) is a known association with septal deviation. Spurs are found at the junction of the perpendicular plate of the ethmoid and the vomer and they are usually associated with septal deviation.
C. TRAUMATIC CAUSES:
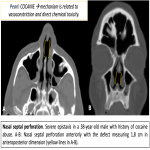
- Nasal septal perforation: defect in the nasal septum with communication between the two nasal cavities. It may affect either the bony or cartilaginous septum. The anterior septal cartilaginous area is affected more commonly.
Other sources of local trauma and potential nasal obstruction are nasal or facial bone fractures, foreign body insertion, septal perforation from substance abuse, and iatrogenic trauma (from surgery or placement of appliances). Children may present with epistaxis after digital trauma or local irritation from foreign bodies.
D. OTHER CAUSES:
Non-neoplastic nasal masses:
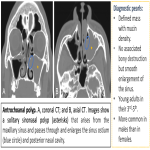
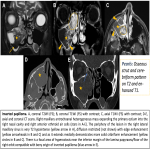
- Choanal polyps are unusual and are solitary sinus mass or mucous retention cyst, which has passed through the sinus ostium (or accessory ostium), into the nasal cavity with posterior extension to the choana. The antrochoanal polyp is the most frequent form and typically presents with nasal obstruction in children and young adult males. The imaging appearance is characteristic and frequently allows a specific diagnosis. However, neoplasms such as papillomas may mimic it on non-contrast CT.
-
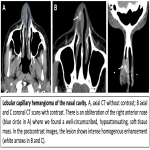
Lobular capillary hemangioma of the nasal cavity (also known as nasal pyogenic granuloma), is an uncommon, benign, rapidly growing vascular neoplasm of the nasal cavity. Epistaxis and nasal obstruction are the most common presenting symptoms.
Neoplastic nasal masses:
Unilateral and chronic obstruction usually implies structural aetiology. Additional “red flags” that suggest sinonasal malignancy include epistaxis, facial pain, facial paraesthesia, cervical lymphadenopathy, and ocular symptoms. Endoscopy and CT are indicated. The need for MRI and biopsy would depend on the findings of the initial exams.
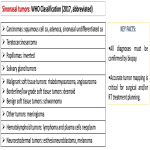
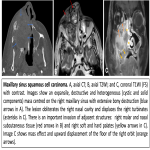
- Sinonasal tumours: sinonasal neoplasms are rare, representing 3% of head and neck cancers. Malignant lesions are more common than benign and the prognosis is generally poor. Squamous cell carcinoma accounts for 80% of malignancies and affects mainly elderly males. Risk factors are smoking, the inhalation of dust of several volatile chemicals, and infection with HPV (specifically HPV 16). The purposes of imaging are recognition of a tumour, determining the extent and differentiation from mucosa and fluid, and defining the involvement of vital anatomical structures.
Sinonasal papillomas are the most frequent benign tumour (incidence of 5% of all sinonasal tumours) and predominate in middle-aged males. The commonest subtype is the inverted papilloma that arises in the maxillary sinus or from the lateral nasal wall and originates unilateral nasal obstruction.
-
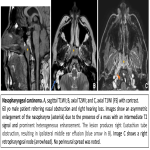
Nasopharyngeal carcinoma: adenoidal hypertrophy requires exclusion as a cause of nasal obstruction. A retrospective analysis of adult patients with adenoidal hypertrophy found an incidence of 16% of malignancy, due to nasopharyngeal carcinoma or less commonly, non-Hodgkin’s lymphoma. Asymmetry of the lateral walls (especially the fossa of Rosenmueller), and invasion of the osseous margins of the nasopharynx are very suggestive findings on CT and MRI. Radiologists mustn't assume that excess nasopharyngeal soft tissue in adults is always postinflammatory, especially in the presence of “red flags”: nasal obstruction, epistaxis, pain, otitis media, and cervical lymphadenopathy.