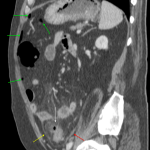
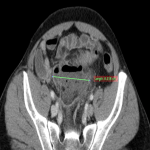
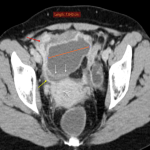
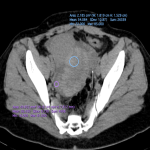
In the ED the aim of the abdominopelvic CT should be to achieve a high degree of discrimination between the pathologies that require urgent surgical intervention versus those that need conservative treatment, as well as to highlight the aspects that may further influence patient management.
Following the most recent updates to the surgical guidelines, we further review the key CT features to note when assessing a potential NTAE surgical candidate, based on the diagnoses presented in the mnemonic.
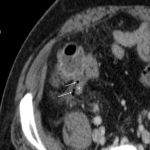
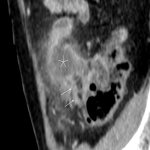
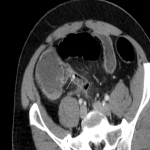
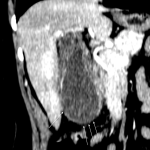
A: APPENDICITIS
Complicated appendicitis (gangrenous or perforated) requires urgent surgical intervention. [3]
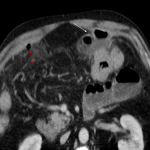
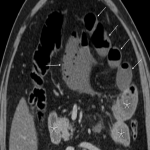
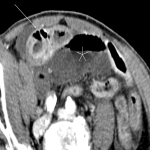
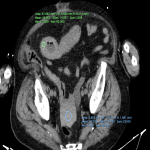
The CT differentiation between simple and gangrenous appendicitis is difficult. However, intraluminal air may indicate gangrenous appendicitis (due to the gas-forming microorganisms). This sign has moderate positive predictive value, and should at least warrant a more prompt surgical solving. [4]
Indicators for perforation are extraluminal gas, wall defect, abscess, and ileus. [5]
Furthermore, the sole presence of an appendicolith is an independent risk factor for perforation and currently represents an indication for emergency surgery. [3]
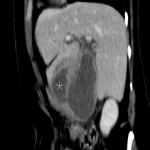
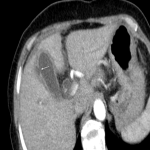
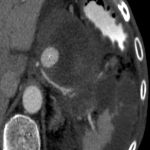
B: BILIARY TRACT DISEASE
The most severe complications of acute calculous cholecystitis are gangrene and perforation, which are surgical emergencies. [6]
When evaluating acute cholecystitis with CT, it is essential to check for homogeneous parietal contrast uptake. Focal/diffuse absence of mural enhancement strongly suggests gangrene.
Other CT indicators of gangrene, but of lower sensitivity are intraluminal membranes, mucosal hemorrhage, and pericholecystic abscess.
Additionally, a focal parietal irregularity or defect is a major sign of gangrenous transformation with subsequent perforation. [7]
Emphysematous cholecystitis is another surgical emergency due to the high risk of perforation. The diagnosis is made by identifying gas within the gallbladder lumen or wall. [7]
- Acute cholangitis - is essentially a clinical diagnosis.
CT finds its usefulness in diagnosing a concurrent liver abscess (parasitic or pyogenic) and identifying its most feared complication - rupture in the abdominal cavity or the bile ducts, which is a surgical emergency. [8]
D: DIVERTICULITIS
The management of acute diverticulitis has changed dramatically over the last years and CT has a crucial role in deciding between conservatory treatment and surgery. [9]
Currently, the only indication for emergency surgery is perforation complicated with generalized peritonitis. The CT diagnosis is based on the combination of extra-luminal air with free fluid, with the following remarks:
- the extraluminal air should be at a distant location, defined as > 5 cm from the affected segment of the colon;
- contrast medium extravasation is considered an accessory criterion. [9]
As regards abscess formation, the size of 4–5 cm is considered the limit between antibiotics only versus drainage/surgery. [9]
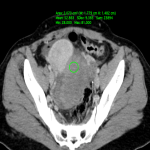
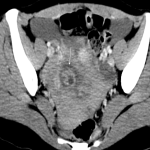
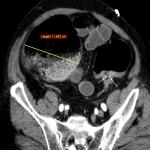
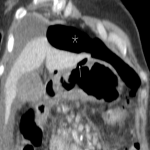
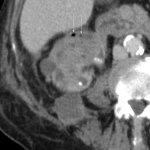
O: OVARIAN DISEASE
The main surgical emergencies related to the ovary are diseases that:
- Cause sepsis: Tubo-ovarian abscess
- signs of complications that are surgical emergencies: abscess rupture (irregular mural contour/contrast enhancement) and generalized peritonitis (thickened and enhancing peritoneum).
- dimensions are important, as a diameter >3-4 cm calls for urgent drainage;
- a serpiginous tubular/multilocular morphology is more suggestive of pyosalpinx. [10]
- Cause ischemia: Ovarian torsion
The only pathognomonic CT sign for ovarian torsion is the appearance of a twisted ovarian pedicle (whirlpool sign). Lack of contrast enhancement and hyperdensity on the pre-contrast scan (> 50 UH) is suggestive of hemorrhagic necrosis. [11]
- Cause hemorrhage: haemoperitoneum secondary to a ruptured hemorrhagic cysts
Useful features for diagnosis are cyst size and shape (shrunken vs. maintained), sentinel clot sign, haemoperitoneum attenuation difference pre- and postcontrast, and contrast medium extravasation.
The CT criteria that influence the decision for urgent surgery are cyst size and haemoperitoneum depth. [11]
M: MALIGNANCY
The main surgical emergencies of gastrointestinal malignancy are obstruction and perforation.
Obstruction is more frequent than perforation.
Gastric cancer perforation is a local complication of the ulcerative subtype.
Colon cancer perforation can occur at the tumor site (70%), usually with localized peritoneal contamination in the form of abscess/fistula,
or proximally (30%, diastatic perforation of the caecum due to obstructive tumors), in which case the result is generalized peritonitis. [12]
CT features pathognomonic for perforation are wall discontinuity with adjacent fat stranding and extraluminal air.
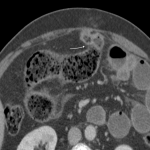
I: INTESTINAL OBSTRUCTION
Adhesions from previous surgery are the primary etiology (~ 75 %) of intestinal obstruction (IO). [13]
Over the last decade, the management of IO evolved such that today most are treated non-operatively. Indications for urgent surgical exploration are peritonitis (perforation), strangulation, and ischemia. [13]
An algorithm for a quick assessment and report could be:
1. Check for pneumoperitoneum;
2. Check for mesenteric veins and arteries permeability;
3. Check the intestinal wall and contents:
- Alarming signs are those of bowel wall infarction (and consequently urgent surgery): absent mucosal enhancement, pneumatosis intestinalis, pneumatosis portalis.
- The thickness of the wall does not correlate to the severity, as in pure arterial occlusion the wall may appear thinned ("paper-thin wall"). Mural thickening is classically attributed to the venous occlusion, and it may appear hypodense (edema)
or hyperdense (hemorrhage).
- the small bowel feces sign suggests a subacute/partial IO and is usually present near the site of obstruction. [14]
4. Check loop configuration:
- A closed loop configuration (C- or U-shaped, with the mesenteric vessels converging toward the site of obstruction) calls for urgent surgery.
- The presence of a transition point between dilated and collapsed bowel is suggestive of IO secondary to adhesions.
5. Check other associated features:
Generally, mesenteric fat stranding and free fluid have limited value in estimating the severity of bowel ischemia, but in pure arterial occlusion, fat stranding appears exclusively in transmural ischemia.[14]
N: NEPHRITIC DISORDERS
The main renal urologic emergencies are:
1. Pyonephrosis
The diagnosis of pyonephrosis is not based on CT alone. However, some key features to avoid misdiagnosing it as hydronephrosis are :
- pelvis wall thickening;
- presence of gas bubbles;
- fluid density higher than normal (although fluid attenuation measurement is not a feasible method to distinguish between water and pus); fluid-fluid levels;
- renal/perinephric inflammatory changes. [15]
2. Renal/perinephric abscess
Abscesses belong to the severe end of the pyelonephritis spectrum. Depending on the diameter (>3-5 cm), the need for emergency intervention is decided.
The only pathognomonic CT feature is the presence of gas. Other diagnostic clues are irregular walls, pseudo capsule, stranding of adjacent fat, and fascial thickening. [16]
3. Emphysematous pyelonephritis
Treatment options have evolved and mild cases are now managed conservatively. However, emphysematous pyelonephritis remains a life-threatening disease that must be diagnosed and treated promptly.
CT is the most sensitive method for diagnosing this entity. The kidney appears structurally altered, including fluid collections and gas.
Gas expansion into the perinephric tissue implies extension of the infection beyond Gerota's fascia. [17]
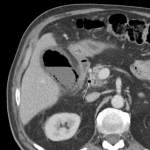
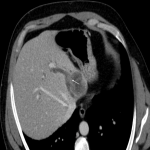
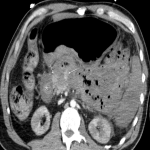
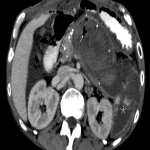
A: ACUTE PANCREATITIS
Acute pancreatitis is a pathology for which the guidelines recommend surgery as a last resort.
However, infected necrotizing pancreatitis requires urgent surgical attention (minimally invasive or open surgery).
Carefully scouting gas bubbles is recommended, as they turn the case into a surgical emergency.
The role of CT in staging and monitoring the severity of acute pancreatitis is already established. [18]
Complications are important to report because they change management:
-(peri)pancreatic necrosis;
-fluid collections;
-ascites;
-vascular complications (thrombosis, hemorrhage, pseudoaneurysms) - always check for high-density fluid on pre-contrast scan or contrast medium extravasation, because bleeding complications in acute severe pancreatitis warrant endovascular or surgical intervention. [19]