In patients with acute chest pain, the TRO protocol can confirm or rule out pathologies such as CAD, PE, or AAS simultaneously in one examination [1] [2]. However, chest pain with a troponin increase can be caused by non-coronary factors that should be identified to improve patient management [4]. Recently, some studies have shown that a cardiac CT scan may identify other myocardial pathologies such as myocarditis, Takotsubo cardiomyopathy, or Myocardial Infarction with Non-Obstructive Coronary Arteries (MINOCA) in the absence of CAD, PE, or AAS [3].
The ECG-gated CT protocol includes a pre-contrast scan of the entire thorax, an angiographic scan with z-axis coverage from the thoracic inlet to the diaphragm, and a LIE scan with the field of view limited to the heart after 7-10 minutes of the injection of contrast medium (CM [3].
If there are no contraindications, it is recommended to administer sublingual nitroglycerin about 3-5 minutes before the scan for coronary dilation and, in patients with high heart rate (HR), it is recommended to administer beta-blockers to obtain a target HR < 65 beats per minute [3].
A prospective ECG-gated cardiac CT angiogram is preferred for patients with sinus rhythm and HR < 65 bpm, whereas a retrospective ECG-gated scan is recommended in patients with arrhythmias, high heart rate, or if it is necessary for the evaluation of cardiac motion (i.e., suspected Takotsubo cardiomyopathy) [3].
The kVp setting for the angiographic study is influenced by the patient's BMI, specifically [3]:
- 80 kVp for BMI < 20.
- 100 kVp for BMI between 20 and 30.
- 120 kVp for BMI > 30.
It is recommended to use a high-concentration iodinated contrast medium (370-400 mg/mL) [3] to reach an optimal Iodine Delivery Rate (IDR) of 2 g I/s [4].
The contrast infusion protocol involves a three-phase injection [3]:
- First phase: contrast bolus.
- Second phase: mixed solution (70% saline solution and 30% contrast medium).
- Third phase: saline solution.
For selecting the scanning timing, it is preferable to use the bolus tracking technique by circumscribing a region of interest (ROI) within the left ventricle with a starting threshold value of 100 HU.
With a 256-detector CT, the amount of contrast used is calculated based on the flow rate chosen to have a total infusion duration of the iodinated bolus of 12 seconds and the mixed bolus of 5 seconds, for a total volume of contrast medium between 62 ml and 78 ml [3].
The infusion rate varies based on the set kVp [3]:
- 4.6 ml/s at 80 kVp.
- 5.4 ml/s at 100 kVp.
- 5.8 ml/s at 120 kVp.
If the TRO is negative, an additional contrast bolus is administered within 3 minutes of the first one to reach a total iodine dose of about 600 mg per kg. The volume of contrast medium to be infused with the second bolus is calculated according to the formula:
[Patient Weight (Kg) / Concentration of iodinated contrast medium (370 o 400 mgI/mL)] * 600
to which the amount already administered for the angiographic study is subtracted [3] [5].
The LIE-CT scan is acquired after 7-10 minutes from the infusion of the second contrast medium bolus with the same technical setting used for the pre-contrast scan, i.e., by performing a scan at 80 Kv [3].
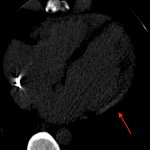
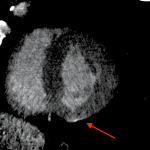
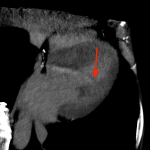
In patients with triple rule out negative, LIE allows assessing the presence of myocardial damage, defined as a focal hyperdense area compared to the surrounding heart muscle [5].
Depending on the location of the scar, it is possible to distinguish between an ischemic pattern or a non-ischemic pattern [6] [7] [8].
In the ischemic pattern, the scar involves the subendocardial and/or transmural region.
In the non-ischemic pattern, the involvement is in the intramyocardial or subepicardial region. The identification of a scar in these locations is suggestive of myocarditis or cardiomyopathies.
In the absence of myocardial damage, the quantification of ECV is useful for the diagnosis of diseases in which there is an increase in the extracellular space, as occurs in some cardiomyopathies (e.g. amyloidosis).
The ECV is calculated by the following formula:
ECV CT = (1-Hct) * (Δ UH myocardium / Δ UH blood)
Where Hct is the hematocrit of the patient measured on the same day of the CT analysis, Δ UH myocardium is the difference in myocardial attenuation between the LIE scan and the precontrast scan while Δ UH blood is the attenuation difference of the intraventricular blood pool [3].
ECV values are considered normal if they are below 27% [9]. However, some diseases may show increased values [10] [11] [12].
Although the evaluation of LIE on CT shows a slight underestimation of the extent of myocardial scarring compared to cardiac magnetic resonance [13], the simultaneous evaluation of TRO, LIE and ECV in patients with chest pain and mild elevation of troponins increases diagnostic accuracy up to 90% (vs 50% of TRO alone) [3].