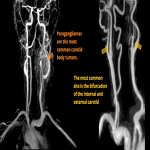
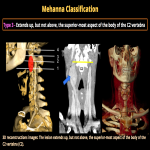
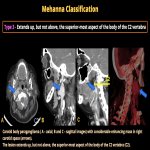
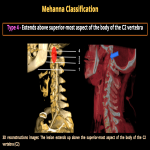
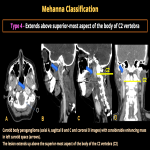
Paragangliomas are the most common carotid body tumors. Those are vascular lesions associated with the parasympathetic nervous system, originating from glomus cells within the carotid body, the jugular foramen, the middle ear, and the vagus nerve.
The most common site is the bifurcation of the internal and external carotid, which represent 70% of the paraganglioma of the head and neck.
Around 3% of the cases are functional carotid body tumors because they synthesize and secrete catecholamines, which can result in hypertension, headache, heart palpitations, and dizziness. However, most are asymptomatic, painless, and slow-growing tumors.
Treatment can vary from:
- Active surveillance
- Radiotherapy if there is continuous growth in a patient with multiple comorbidities and high operative risk.
- Surgical resection if the risk of sequelae for surgery outweighs those from surveillance or radiotherapy, as well as the patient's age and performance status.
Although a benign condition, surgical resection is challenging and can result in considerable morbidity because of neural and neurovascular sequelae. Therefore, it is crucial to accurately assess the risk of potential surgery complications for treatment decision-making.
The most known risk classification and widely used is the one developed by Shamblin et al. in 1971.
This classification helps evaluate the technical difficulty of dissecting the neoplasm before surgery by predicting intraoperative and postoperative vascular morbidity. It is an anatomical classification that describes the relationship between the tumor and the carotid body bifurcation and the degree of circumferential involvement of the internal and external carotid arteries.
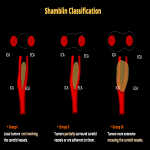
Shamblin et al. classified carotid body tumors into three groups:
- Shamblin I: Tumors are localized, and surgeons can carefully excise them without significant trauma to the vessel wall.
- Shamblin II: Adherent tumors partially surround the carotid vessels, reflecting the significant technical difficulty in dissection.
- Shamblin III: Tumors surround the carotid vessels with complicated dissection and frequent injuries to the cerebral circulation.
Luna-Ortiz et al., in 2006, proposed modifications to the Shamblin classification because they believed that it did not predict actual infiltration of tumors to the carotid vessel walls.
They proposed that the tumor size be included since it positively correlated with the Shamblin classification. Depending on vessel involvement, tumors larger than 4 cm could be classified as Shamblin II or III. However, there is no direct association between size and vessel involvement. They stated that carotid body tumors classified as Shamblin I could also infiltrate carotid vessels, a complication the previous Shamblin classification would not foresee.
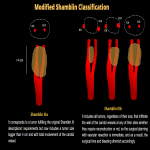
For that reason, it was proposed the division of Shamblin III into a and b:
- Shamblin IIIa: It corresponds to a tumor fulfilling the original Shamblin III descriptions' requirements but now includes a tumor size bigger than 4 cm and with total involvement of the carotid vessel.
- Shamblin IIIb: It includes all tumors, regardless of their size, that infiltrate the wall of the carotid vessels at any of their sites whether they require reconstruction or not, so the surgical planning with vascular resection is immediate, and as a result, the surgical time and bleeding diminish accordingly.
Although Shamblin and Luna-Ortiz classifications indicate technical difficulty and vascular complications (including operative time, amount of blood loss, and need for complete carotid resection), it does not predict postoperative neurological morbidity, which is the most common type of complication.