Type:
Educational Exhibit
Keywords:
Emergency, Genital / Reproductive system male, CT, Ultrasound, Ultrasound-Colour Doppler, Contrast agent-intravenous, Acute
Authors:
C. aslanidi, S. Athanasiou, Z. Papoutsou, V. Mamalis, S. Mylona, A. Tsanis
DOI:
10.26044/ecr2023/C-20007
Background
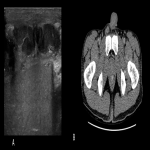
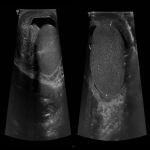
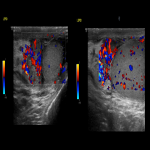
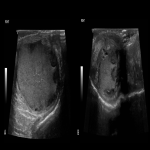
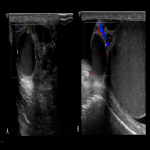
Patients presenting with acute scrotal pain (ASP) to the emergency department require a timely diagnosis. Frequently encountered causes of ASP include testicular torsion, complicated hernia, epididymo-orchitis or testicular trauma. Testicular (or internal spermatic) vein thrombosis (TVT) is a rare entity, most often involving the left side. Diagnosis solely based on the clinical presentation can be challenging and TVT can be easily misdiagnosed as an incarcerated inguinal hernia, epididymo-orchitis or spermatocele which may result in wrong treatment pathway and possibly unnecessary surgical intervention. The exact etiology of TVT is unknown but it is thought that the anatomical factors responsible for the prevalence of varicocele of the left side may explain the more frequent involvement of the left testicular vein.
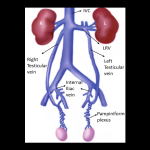
The venous drainage system of the human testis consists of two networks, the superficial which drains the veins from the scrotum and the deep which drains veins from the testis, the epididymis and the ductus deferens. Veins from the testis and the epididymis arise posteriorly from the testis and then band together in order to form the pampiniform plexus, which surrounds the testicular artery inside the spermatic cord. The lower testicular temperatures are facilitated by this arrangement, which allows the exchange of heat and tiny molecules due to the fact that arteries and veins are only separated by their vascular wall. Three or four veins in the inguinal canal drain the pampiniform plexus which ascends anteriorly to the ductus deferens. These veins emerge from the deep inguinal ring into the abdomen, climb anterior to the psoas major and the ureter on each side and then combine in order to form a single testicular vein on each side
. The right testicular vein joins the inferior vena cava directly on its right anterolateral segment at an acute angle. The left testicular vein drains in the left renal vein at a 90 degrees angle. Varicocele, which is an abnormal enlargement of the pampiniform plexus, typically arises on the left side. It is speculated that this left-side preponderance can be explained due to the elongated course of the left testicular vein and the orthogonal junction with left renal vein. Numerous variations of the anatomy of the testicular veins have been reported in the literature, including duplication, draining of both testicular veins in left renal vein, communication with other retroperitoneal veins as well as aberrant drainage of the left testicular vein into the inferior vena cava.
TVT is a rare event, with approximately 30 cases described in the literature. The clinical presentation is usually non-specific and includes groin pain, acute or subacute scrotal pain without fever, while swelling or a palpable mass may be present on the semi-scrotum that is involved. Exercise is the most commonly described risk factor, due to increased abdominal pressure and subsequent reduced venous drainage from the testis, predisposing to thrombosis. Several other etiologies have been described in the literature including trauma, malignancies causing venous obstruction, hypercoagulability (protein C deficiency, factor V Leiden mutation), as well as COVID-19 infection.
There is no standard treatment pathway for this rare entity. Some investigators suggest that conservative treatment with anti-coagulants along with rest should be the first-line approach in patients with TVT. It is also possible to treat the patient surgically, with excision of the thrombosed vein.