Radiography: In acute phase radiography may be negative,
in subacute and chronic phase they may be misdiagnosed as cases of malignancy or osteomyelitis.
In clinical suspicion of stress fracture MRI imaging is very useful for initial diagnosis and follow up,
particularly when radiographs are normal.
Initial phase sensitivity of radiograph is 15-35%,
but increases at follow up to 30-70%.
Usually are demostrated radiologically 2-4 weeks after onset of pain.
Radiographic findings in osteal bone:
Endosteal or periosteal callus formation without fracture line.
Circumferential periosteal reaction with fracture line through one cortex.
Frank fracture.
Radiographic findings in cancellous bone :
Flake –like patches of new bone formation
2-3 weeks after pain onset.
Cloud like area of bone sclerosis.
Focal linear area of sclerosis,
perpendicular to the trabeculae.
3-phase scintigraphy: In the past it was the method of choice (high sensitivity,
low specificity).Findings are evident 1-2 weeks before radiographic findings.
Not useful method for follow up.
CT Indications:
If MRI is contraindicated.
At specific locations like (sacrum,
scaphoid,
pars interarticularis).
Aids differential diagnosis of osteoid osteoma.
In surgical planning.
When fracture line is not evident at radiography/ MRI.
MRI : is the method of choice for demonstrating stress fractures,
as well as stress reactions and periosteal reactions without an obvious fracture line,
which constitute an earlier stage of stress fracture.
MRI findings precede by weeks those of plain radiographs also demonstrating associated soft tissue injuries.
It is a useful method for follow up due to lack of ionizing radiation.
It shows equal sensitivity (100%) but higher specificity (85%) to scintigraphy.
Also,
better anatomic details are shown and more precisely the tissues involved are depicted.
The grading system of stress fractures,
based on MR imaging findings is:
Grade 1- low grade periosteal edema (STIR).
Grade 2-moderate to high grade periosteal edema
(STIR) and medullary edema(Τ2).
Grade 3-as 2 and medullary edema visible at Τ1.
Grade 4-like 3 and visible fracture like.
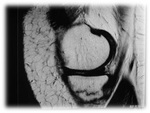
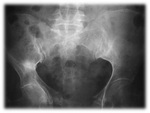
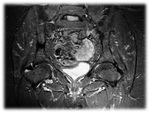
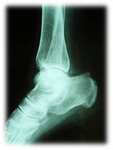
Tibia: Most common location.
It is 20-75% of all stress fractures (figure1,2,3,4).
At the anterior surface of tibia cortex is sclerotic with perpendicular lucent lines.
Longitudinal stress fractures should be differentiated from shin splint which is an early form of the stress injuries spectrum and is caused by abnormal traction effects imposed on the tibia at muscular attachments.
At radiography it appears as diffuse periosteal reaction along anteromedial cortex of distal tibia.
In contrast to stress fracture,
the periosteal reaction is not associated with a discrete band of sclerosis unless the syndrome is complicated and advanced.
MRI Grades of shin splint:
1.Soft tissue edema and inflammation along anteromedial cortex
2.Soft tissue edema with periostitis and subtle marrow edema
3.
Soft tissue edema with periostitis and significant marrow edema
4.
All the above with associated transverse bands at sites of microfractures.
Metatarsals: second most frequent location.
It occurs at neck or distal diaphysis of 2nd or 3rd (figures 5-11).At 5th metatarsal stress fracture is located 1.5cm distal to tuberous.
Femur: stress fracture at neck or diaphysis is a common location (figures 12-15). Long distance running is associated with inner surface of proximal diaphysis fracture.
Sacrum: Radiography has 0% sensitivity.
MRI is the method of choice (figures 16-20).
Pubic and ischial ramus: Associated with tendinosis and bursitis of semitendinosus,
semimembranosus and biceps.
Common location is inferior pubic ramus (figures 21-24).
Calcaneous: at radiography it appears as line of sclerosis perpendicular to trabeculae and parallel to posterior cortex(figures 25-26).
Navicular bone: Diagnosis can be delayed 2-4 months.
Common at central part due to reduced blood supply.
Diagnosis is difficult by radiography because fractures are at sagittal plane.
CT reconstructions or MRI are essentials for diagnosis.
Stress fractures are divided to low or high risk depending on their location.
Low risk are located at the posterior or medial aspect of tibia,
fibula,
and lateral malleolus whereas high risk are located at the femoral neck,
anterior midtibia,
medial malleolus,
tarsal navicular,
talus,
fifth metatarsal,
base of second metatarsal,
patella and great toe sesamoid.
High risk fractures may require longer recovery period and often surgical intervention.