Keywords:
Oedema, Education, MR, Musculoskeletal soft tissue
Authors:
J. Araújo, S. Magalhães, I. Ferreira, J. Pires, R. Maia, M. Ribeiro; porto/PT
DOI:
10.1594/essr2015/P-0045
Imaging findings OR Procedure Details
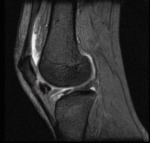
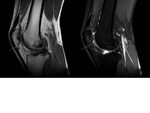
Hoffa's disease (Fig.3 and 4)
- Is a syndrome of infrapatellar fat pad impingement.
- Sometimes after an acute impact or repetitive traumas,
the fat pad can become impinged (pinched) between the distal thigh bone,
femoral condyle,
and the patella.
- As the fat pad is one of the most sensitive structures in the knee,
this condition is known to be extremely painful
- The resulting pain,
swelling and fat hypertophy limits range of motion.
Over time,
fibrotic tissue is formed.
- Hoffa's impingment,
specially in the supero-lateral aspect,
is associated with patellofemoral mechanical abnomalities,
such as an increase in the patellar tendon–patellar length ratio,
increased lateral patellar tilt and a shallower trochlear sulcus.
These factors positively influence excessive friction or pressure of the lateral patellar facet over the lateral femoral condyle,
resulting in edema in the intervening superolateral portion of Hoffa’s fat pad.
- Areas of increased signal intensity on T2-weighted MR images represent acute edema and hemorrhage within the swollen fat.
- Bowing of the patellar tendon from mass effect is seen frequently
- A small joint effusion may be present.
- Subacute and chronic phases: fibrin and hemosiderin have low signal intensity on both T1 and T2 weighted MR images.
Fibrous tissue may be transformed into fibrocartilaginous tissue,
which rarely may ossify.
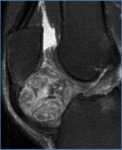
Intracapsular chondroma (Fig.5)
- Results from extrasynovial metaplasia in the capsule or adjacent connective tissues.
- Although it is a rare lesion,
it overwhelmingly occur around the knee,
typically in the infrapatellar fat pad.
- Sometimes may calcify and even ossify.
It also may erode the lower pole of the patella.
- MR imaging demonstrates a heterogeneous mass within the infrapatellar fat pad,
with the high signal T2 intensity representing chondroid matrix or edema and areas of low signal intensity,
representing either calcification or ossification.
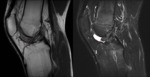
Postsurgery/postarthroscopy fibrosis (Fig.6)
- It is a complication like in the cyclop lesion,
where an excessive scar tissue response leads to painful restriction of joint motion,
with scar tissue forming within the joint and surrounding soft tissue.
- Fibrous scarring after arthroscopic surgery can involve the infrapatellar fat pad.
- The arthroscopic portals are anterolateral,
anteromedial and central.
- Local fibrosis may cause apparent thickening of the patellar tendon,
giving the appearance of chronic tendinosis or jumper´s knee.
- Predominantly low signal punctate,
linear or even nodular areas on T1 and T2,
coursing from the posterior portion of the fat pad to the anterior surface of the tibia,
wich can cause impingment.
There could also exist an heterogeneous signal on T2W images from synovitis and granulation tissue intermingled with fibrous tissue.
Cyclops lesion (Fig.7)
- It represents localized arthrofibrosis occurring after ACL reconstruction (reaction to exposed ACL graft material or operative defris).
- Consists in localized nodular soft-tissue mass that arises from the anterior aspect of the ACL graft and extends anteriorly and superiorly in the intercondylar region of the femur.
- A focal nodular mass like lesion of low signal on T1W images and heterogeneous signal on T2W images with/without cystic changes from synovitis and granulation tissue intermingled with fibrous tissue.
Infrapatellar plica syndrome (Fig.8; Fig.2)
- Is the most common plica in the knee.
Is a pathological condition secondary to inflamation.
- Is easily identified at MR imaging as a linear low signal intensity structure anterior and paralel to the ACL,
on sagital images.
- Because of its location and orietation,
it is sometimes mistaken for the ACL.
It may also be mistaken for focal nodular synovites,
post operative changes or a loose body.
- It represents an embryologic remmants of synovial fold and is originated from the intercondylar notch in the region of the anterior cruciate ligament.
It widens into the anterior joint space and attaches into the synovial lining of infrapatellar fat pad.
- there is a significant amount of curvilinear high T2 signal along the expected course of the infrapatelar plica or markedly thickened plica is visualized.
Thickening of the plica even in the absence of edema or fluid suggests a chronic injury.
Pigmented Villonodular synovitis (PVNS)-(Fig.9)
- Is a benign proliferative disorder of the synovium that may involve the synovium of the joint,
diffusely or focally,
that may occur extraarticularly in bursa (pigmented villonodular bursitis-PVNB) or tendon sheath (pigmented villonodular tenosynovitis-PVNTS or cell tumor of the tendon sheath-GCTTS).
- GCTTS/PVNTS is the most common form of the disease.
- Usually involves large joints as 80% of the cases affect the knee.
- The masslike proliferative synovium could appear as an diffuse PVNS or a limited single nodule in a focal form.
- Synovial deposition of hemosiderin results in irregular masses that show a significant low signal on all sequences.
Areas of high signal on T2 may be present and are likely caused by inflamed synovium or joint effusion.
JUMPER KNEE-(Fig.10)
- Jumper’s Knee refers to a spectrum of disorders that occur in patients with degeneration and/or tearing of the patellar tendon.
It is one of the most common tendon abnormalities in athletic active individuals,
with special incidence in basketball and volleyball players.
- Patients with Jumper’s Knee may experience a combination of proximal patellar tendinopathy and osteochondral reactive marrow changes and Hoffa edema.
- MRI have high sensibility to diagnose this cases.
T2 hyperintensity within the proximal tendon is most commonly seen.
More severe tendinopathy demonstrates full thickness involvement by intrasubstance signal. Edema may be present within the adjacent Hoffa’s fat pad,
with irregular T2 hyperintensity replacing normal fat signal.
Partial thickness and complete tears may also occur.
SINDING-LARSEN JOHANSSEN SYNDROME(Fig.11)
- It represents a chronic traction injury of the immature osteotendinous junction.
Some authors classify it as a paediatric version of "jumper's knee".
- It affects the proximal end of the patellar tendon as it inserts into the inferior pole of the patella.
- MRI shows abnormal signal in the inferior patella with irregular cortical margins and osseous fragmentation