Keywords:
Musculoskeletal spine, Bones, CT, MR, Digital radiography, Localisation, Imaging sequences, Diagnostic procedure, Neoplasia, Education and training
Authors:
E. Gezmis1, G. Özcan Söylev1, F. Ulu Öztürk2; 1Izmir/TR, 2Ankara/TR
DOI:
10.1594/essr2016/P-0007
Background
Introduction: Osteoid osteoma (OO) is a benign bone forming tumor that is first described by Jaffe in 1935 (1).
It is a small spherical tumor with a diameter of 1.5 cm or less,
composed of a central zone named nidus,
which is an atypical bone completely enclosed within a well-vascularized stroma and a peripheral sclerotic reaction zone,
which is composed of osteoblasts,
osteoclasts and dilated capillaries (2).They account for approximately 10% of all benign bone tumors and there is a male predilection with a male to female ratio of 2-4:1.
They are usually found in children and young adults,
between the ages of 10 – 35 (3).
Although any bone can be involved,
they mostly occur in long tubuler bones of extremities,
especially in proximal femur.
Around %10 of osteoid osteomas present in the vertebral column,
mostly in the posterior elements of lumbar vertebrae,
and only in %2 of these spine cases sacrum is affected (4).
Herein we present an atypical osteoid osteoma in sacrum,
which extends beyond the anterior cortex of bone causing soft tissue swelling.
Case Report: A 21 year old male patient presented to our physical therapy and rehabilitation clinic with lumbar and right groin pain that has been occurring for 3 months.
There was no history of trauma,
fever or weight loss.
On physical examination there were no specific findings or neurological deficits.
Laboratory examination results including erythrocyte sedimentation rate,
C-reactive protein value,
Rheumatoid Factor,
blood biochemistry,
liver and kidney function tests were normal.
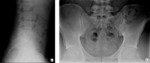
Lumbosacral spine and sacroiliac joint x-rays revealed no abnormality (Figure 1).
The result of lumbar spine magnetic resonance imaging (MRI),
which was performed to rule out lumbar disc herniation,
were also normal.
Hence conservative treatment was recommended.
However one month later the patient returned with no improvement in his complaints.
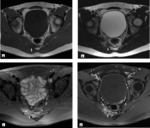
Sacroiliac joint MRI was performed to rule out sacroiliitis and showed a 2 cm in size,
slightly expansile nodular lesion on the right transverse process of S3th vertebra with central hypointensity at all sequences and hyperintense enhancing peripheral rim.
There was bone marrow edema around the lesion and the lesion was also extending towards the adjacent muscles causing soft tissue swelling and edema (Figure 2).
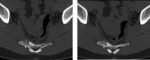
Sacral computerized tomography (CT) was performed to confirm the diagnosis,
depicting welldemarcated hyperdense sclerotic nodular lesion about 2 cm in size,
with its hypodense peripheral rim extending beyond the anterior cortex,
on the right transverse process of S3th vertebra.
A 0.3 cm nidus was also detected at the center of reactive bone sclerosis on CT scan (Figure 3).
The patient underwent surgery and the result of the pathological examination was osteoid osteoma.
Discussion: Osteoid osteoma involving the sacrum is extremely rare,
and it has also been reported that the diagnosis can be delayed compared with other more common skeletal sites (5,
6).
In our patient the diagnosis was delayed and the patient was treated with conservative therapy for 1 month which didn’ t provide relief.
Plain X-ray,
CT,
MRI,
Dynamic F-18 FDG PET/CT can be used in determining the exact localization,
characterization,
other accompanied findings such as edema and revealing the effects of tumor on the adjacent soft tissues (7).
CT is the best imaging modality to show the presence of a low-attenuation nidus,
the lesion’ s characteristic finding,
and varying degrees of perinidal sclerosis (8).