Keywords:
Extremities, Musculoskeletal soft tissue, Vascular, MR-Angiography, Catheter arteriography, Diagnostic procedure, Education, Arteriosclerosis, Education and training
Authors:
E. Gezmis1, C. Altın1, E. Duman2, E. Aydın1; 1Izmir/TR, 2Konya/TR
DOI:
10.1594/essr2016/P-0009
Background
Introduction: Popliteal artery entrapment syndrome (PAES) is a rare entity caused by developmentally abnormal relationship between popliteal artery (PA) and surrounding musculotendinous structures,
mostly medial head of gastrocnemius muscle and rarely an anomalous fibrous band or popliteus muscle (1).
It results in extrinsic arterial compression and because of the repetitive insult to the popliteal artery,
in the later stages of undiagnosed PAES aneurysm,
thromboembolism and complete arterial occlusion can occur (2).
Although the anatomic anomalies may be seen in up to %3 of the population and are often bilateral,
most of them are asymptomatic.
Individuals with well developed muscles are more likely to be symptomatic,
so that it is found in young sports person and there is a male predilection with a male-to-female ratio of 15:1.
Diagnostic delay is common because PAES usually occurs in young patients who lack the vascular conditions that would predispose them to atherosclerosis (3).
On the other hand early diagnosis and surgical treatment is very important for good operative outcome and to prevent limb loss.
Here we present a case of lately diagnosed PAES causing bilateral popliteal artery occlusion in a young man although he is a cardiologist.
Case Report: A 29 year old,
healthy man presented with right calf pain occurring during sports activities especially in cold weather.
The duration of his complaints was 10 years but it got worse in the last month turning into intermittent calf claudication and numbness during sports activities.
However patient was asymptomatic while walking.
He was a non-smoker and had no history of chronic diseases.
Physical examination was unremarkable and on both legs distal pulses were palpabl.
His complete blood cell count,
liver and renal function tests,
blood lipid levels,
and coagulation tests were within normal ranges.
He had had sonographic examinations of lower limb arteries three times before and the results had been normal,
however the examinations had been performed on neutral position without plantar flexion and dorsiflexion of feet,
which elicite the arterial compression and is crucial for PAES diagnosis with Doppler Ultrasound.
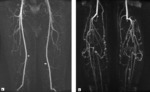
Magnetic Resonance (MR) Angiography of the lower limb arteries was performed which surprisingly revealed complete occlusion of the right PA and occlusion of the proximal half of the left PA.
There were also multiple collateral arteries,
arising from superficial femoral arteries,
supplying right crural arteries and distal half of left PA (Figure 1).
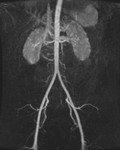
The same imaging findings were seen on the digital substraction angiography (DSA).
There were no clinical,
laboratory and radiological imaging findings supporting vasculitis (Figure 2).
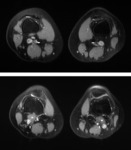
Therefore axial T1,
T2 and fat suppressed pd weighted MR images of both popliteal fossas were performed to detect the cause and they showed aberrant attachments of the medial heads of both gastrocnemius muscles between the occluded PAs and patent popliteal veins (Figure 3).
The patient was diagnosed with PAES but it was to late for muscular release surgery.
He was recommended to reduce sports activities,
antiagregan and cilostazole was initiated.
He has been under follow up since then and there has been no deterioration in clinical symptoms and radiological findings for 6 years.
Discussion: The normal course of popliteal artery in popliteal fossa is between the median and lateral heads of gastrocnemius muscle.
Unfortunately popliteal artery might be entrapped by neighbouring muscles and tendons due to variations that occur during embryologic development of the muscles and arteries (4).
Several classification systems of PAES have been described in literature.
The most commonly used classification,
which was proposed by Whelan and modified by Rich later,
divides this condition into five types (Table 1).
Our patient was affected by Type II PAES.
The characteristic symptoms are leg swelling,
aching pain,
pain at rest,
and tiredness or cramping of the calf but symptoms can vary.
In the early stages,
when the artery is patent except during calf-muscle contraction,
symptoms are usually limited to transitory cramps or a feeling of coldness.
In the later stages,
when the artery is affected by stable lesions (local stenosis or occlusion,
local thrombotic interruption,
or poststenotic aneurysm) typical symptoms are severe acute ischemia and intermittent calf claudication (5).
Most patients,
like ours,
are diagnosed years after the initiation of symptoms and complications,
because vascular problem in young patients without cardiovascular risk factors is not considered at first (6,
7).
Angiography is the classical screening and diagnostic tool in PAES and it demonstrates compression of the popliteal artery with the ankle plantar flexed (8).
Noninvasive imaging techniques such as Doppler ultrasonography,
Computed Tomography Angiography (CTA),
MR imaging and MR angiography can also be used for diagnosis.
Transverse T1-weighted MR imaging is useful to evaluate the aberrant muscular anatomy of the popliteal fossa and also to demonstrate the deviation of the popliteal artery (7).
The definitive treatment for PAES is surgical intervention which is muscle division to release the entrapment.
If significant degeneration or occlusion of the popliteal artery is present,
arterial reconstruction should be performed together with the transection of the anomalous muscle otherwise symptoms can recur because of persistent extrinsic compression on the graft (9,
10).