Keywords:
Hernia, Puncture, CT, Musculoskeletal spine, Interventional non-vascular
Authors:
F. Diez Renovales1, C. Morandeira Arrizabalaga2, B. Ruiz1, J. Cardenal Urdampilleta1, E. Galindez1, I. Lecumberri1, M. Sarmiento1; 1Bilbao/ES, 2Getxo/ES
DOI:
10.1594/essr2016/P-0065
Results
During the study period 258 procedures were performed in 171 patients (132 men / 126 women) with a mean age ± SD of 58.24±13.45 years (range,
18-88).
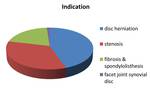
The indications for the injection were: a) disc herniation (44.57%),
b) lumbar stenosis (34.11%),
c)postoperative fibrosis and spondylolisthesis (20.15%) and d) facet joint synovial cysts syndrome (1.17%) Fig. 12 .
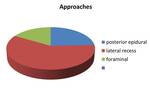
Approaches used were: a) posterior epidural (24.42%),
b) lateral recess (58.91%),
and c) foraminal (16.67%) Fig. 13 .
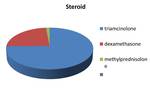
The chosen steroid was triamcinolone (74.81%),
dexamethasone (23.64%) and methylprednisolone (1.55%) Fig. 14 .
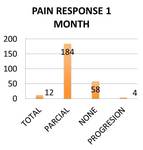
In a significant proportion improvement in the patient´s sintomatology was reported at the first month,
regardless of the indication,
route of corticosteroid injection and steroid used Fig. 15 Fig. 16 .
Regarding the overall outcome,
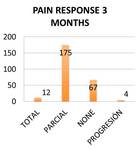
at 3 months 72.48% of the patients experienced clinical improvement Fig. 17 .
And only 21.71% required a subsequent surgery.
The clinical efficacy showed no statistically significant differences according to the indication of the procedure or the route used for the injection.
However,
the improvement of pain was significantly greater in patients treated with triamcinolone than those treated with dexamethasone (p = 0.01)at 1 month Fig. 18 and also 3 months Fig. 19 after the injection.
Regarding safety there were 6 local complications (puncture of the thecal sac) and 3 (1.16%) systemic complications (allergic reaction).
None of these complicationes were of clinical relevance.