Keywords:
Trauma, Acute, Diagnostic procedure, MR, Digital radiography, CT, Musculoskeletal system, Extremities, Bones
Authors:
R. E. Tarud Sabbag1, N. Anand2, C. Boyd1, H. Su1; 1Morristown, NJ/US, 2Morristown , NJ/US
DOI:
10.1594/essr2017/P-0176
Imaging findings OR Procedure Details
Quadriceps Injury
-
The anterior thigh is comprised of 4 muscles: the rectus femoris,
vastus medialis,
vastus lateralis,
and vastus intermedius.
These muscles insert in the patella by the quadriceps tendon.
-
Tear of the quadriceps occurs when any of these four muscles or its conjoined tendon are involved.
Injuries present as tendinopathy,
intramuscular injury,
partial or complete disruption of the distal myotendinous units of the quadriceps muscle.
-
Involves most commonly the vastus intermedius and usually occurs at or proximal to the patellar insertion.
Presentation
-
Patient presents with anterior thigh and knee pain and swelling.
-
Occurs after an acute eccentric contraction.
-
There may be an inferiorly displaced patella (patella baja).
Imaging Findings
-
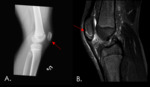
In patients with a high-grade tendon rupture x-rays may demonstrate a low-lying patella also known as patella baja.
-
Knee effusion is a common radiographic finding.
-
Avulsion of fragment from the superior patella,
calcification in the quadriceps tendon or suprapatellar soft tissue swelling may also be present.
-
Normal quadriceps demonstrate a laminar appearance,
well defined and linear with no surrounding edema on MR.
-
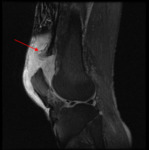
Tendinopathy demonstrates thickening and heterogeneity of tendon units of the quadriceps and may also have mild increased intratendinous signal.
-
Partial tendon tear there is focal partial discontinuity of tendon units in the quadriceps.
There is thinning of the quadriceps,
focal fluid signal within the quadriceps,
soft tissue swelling and intramuscular edema.
-
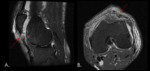
Complete tendon tear there is focal discontinuity of tendon units in the quadriceps.
On MR,
there is hematoma,
intramuscular edema,
patella baja,
redundant patellar tendon and marrow edema in the patella.
-
Intramuscular injury there is increased signal on T2WI that may be linear or ovoid along the long axis of the quadriceps and commonly occurs in the proximal thigh.
Treatment
Patellar tendon injury
- The patellar tendon is attached to the inferior aspect of the patella and extends to the tibial tuberosity.
- As with any tendon pathology patient may present with tendinopathy,
partial tear or a complete tear.
- When there is a rupture of the patellar tendon it may occur at the patellar or tibial insertion.
Presentation
- Patients present with knee pain and may present with a palpable defect in the region of the patellar tendon.
- Can occur when patients fall on a flexed knee with the foot planted.
- It is associated with posterior knee dislocation.
Imaging Findings
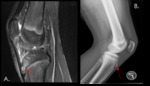
- X-rays may demonstrate soft tissue swelling,
avulsion of the inferior patellar pole and superior retraction of the patella (patella alta) in patients with complete tendon tear.
- Patellar tendinopathy may be tendon thickening and signal heterogeneity with no tendon defect on MR.
- Partial tears are identified on MR as an incomplete defect of the tendon,
as opposed to a complete tear where there is discontinuity of the whole width of the tendon at one level.
- Complete tears may demonstrate avulsion fractures of the inferior pole of the patella and usually affects the proximal portion of the tendon.
Treatment
- Patients with tendinopathy are treated conservatively with rest,
ice,
and physical therapy.
- Surgical repair is reserved for patients with complete tears using end-to-end sutures.
Osgood Schlatter syndrome
- Results from a traction apophysitis of the patellar ligament insertion on the tibial tubercle affecting adolescents and children in periods of rapid growth.
Presentation
- Occurs when there is repetitive microtrauma during the phase of skeletal maturation of the tibial tubercle.
- Patient presents with low grade pain associated with activity.
- On physical exam patients have tenderness at the anterior tibial metaphysis and a visible bump.
Imaging Findings
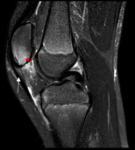
- X-rays demonstrate ossification and thickening of the inferior patellar tendon adjacent to the tibial tubercle,
irregularity of the tibial tubercle,
and adjacent soft tissue swelling.
- MR demonstrates marrow edema in the ossification centers of the tibial tubercle and a thickened infrapatellar tendon.
- Ultrasound may show a thickened,
hypoechoic patellar tendon.
Treatment
- Self-limited condition in most cases.
- Treatment is with rest and immobilization.
- Surgery is reserved for severe cases.
Sinding Larsen Johansson Syndrome
- Characterized by traction tendinitis at the inferior pole of the patella secondary to repetitive microtrauma resulting in ossification within proximal portion of inferior patellar tendon.
Presentation
- Patient presents with point tenderness at the inferior pole of the patella that is exacerbated by activity.
- 10-14 years old are most commonly affected.
- May present similar to Osgood-Schlatter.
Imaging Findings
- X-rays demonstrate calcification of the patellar tendon
- MR demonstrates edema at the inferior pole of the patella and the proximal patellar tendon with adjacent soft tissue edema.
Treatment
- Patients are treated conservatively with rest and immobilization.
Patellar Sleeve Avulsion
- This entity is only seen in pediatric population ages 8 to 12 years old.
- Patellar cartilage of the inferior pole is avulsed off with a small bone fragment.
- Commonly involves the inferior pole of the patella,
however the superior pole of the quadriceps tendon could also be affected.
Presentation
- Occurs after a violent contraction of the quadriceps muscle on a flexed knee.
- Patients present with pain,
swelling,
extensor lag,
and a palpable defect.
Imaging Findings
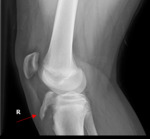
- X-rays in inferior pole avulsions x rays demonstrate a small bone fragment inferior to the patella with associated patella alta and joint effusion.
- X-rays in superior pole avulsion x-rays demonstrate a small bone fragment retracted proximally from irregular superior pole with associated patella baja and joint effusion.
- MR shows a sleeve of unossified cartilage surrounding an avulsed bone fragment.
Treatment
- Open reduction with internal fixation
Patella Fracture
- One of the most common knee injury.
- Fractures of the patella could be transverse (50-60%),
comminuted (30-35%),
longitudinal (12-17%),
avulsions or osteochondral injuries.
Presentation
- Patellar fractures may also present with disruption of any other element of the extensor mechanism such as the quadriceps or patellar tendon.
- Results from a direct blow to the patella,
indirect injury,
pathologic fractures or post surgical patients (such as total knee prosthesis or ACL repair).
- Patients present with knee pain,
swelling,
joint effusion and decreased extension strength.
Imaging Findings
- X rays demonstrate a fracture line,
comminution,
patella alta,
patella baja,
joint effusion or avulsed fracture fragments.
- Fracture line is low signal on T1WI and T2WI.
- MR demonstrates cartilage disruption and marrow edema.
- Tear of medial/lateral retinaculum and medial patellofemoral ligament may also be seen on MR
Treatment
- Open fractures should be treated emergently.
- Surgery should be performed in patients with open fractures,
> 2 mm of articular surface incongruity,
> 3 mm separation of the fracture fragments and disruption of the extensor mechanism.
- Patients treated conservatively are splinted/casted in extension for 4-6 weeks.
Patellar Dislocation
- Occurs after direct or indirect injury to the patella
- Associated with syndromes such as Ehler-Danlos or Marfan in which patients have ligamentous laxity.
Presentation
- Most often seen in patients aged 13-20 years and is more common in females.
- Mechanism of injury is internal rotating twisting force applied to a flexed knee while foot is planted.
- Risk factors include patellar dysplasia,
shallow trochlear groove of the femur,
patella alta,
deficiency of the medial retinacular complex,
lateral hypermobility of the patella and dysplastic distal one third of the vastus medialis obliquus muscle.
- Patient presents with knee sensation of giving way,
joint effusion,
knee pain,
tenderness along the medial retinaculum.
Imaging Findings
- 50-75% of dislocations are occult on physical exam or imaging since they have relocated at that time.
- X-rays demonstrate large joint effusion,
medial patellar avulsion of the medial patellofemoral ligament,
patellar surface irregularities.
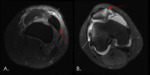
- MR identifies indirect signs of dislocation in the setting of hemarthrosis.
- Marrow contusions (poorly defined marrow foci of increased signal on T2WI and low signal on T1WI) seen at the medial patellar facet and the anterolateral femoral condyle is pathognomonic for recent patellar dislocation (kissing contusions).
- Sprain or tear of the medial retinaculum,
strain or tear of the vastus medialis obliquus and joint effusion are other MR findings.
Treatment
- Conservative management is considered when the patella is stable on physical exam,
partial injury to the medial patellar stabilizers and in the absence of osteochondral injury.
- Surgical management is for patients with osteochondral injuries,
intra articular bodies,
recurrent patellar dislocations and major tear of medial stabilizers.
Tibial Tubercle avulsions
- Most commonly seen in adolescent boys
- Distal patellar tendon attaches at the tibial tubercle ossification center which is susceptible of being avulsed.
Presentation
- Mechanism of injury: active extension of the knee with violent contraction of the quadriceps muscle in jumping sports
- Osgood-Schlatter and Osteogenesis imperfecta are risk factors.
- Patient presents with pain,
swelling and knee held in mild flexion with inability to fully extend
Imaging Findings
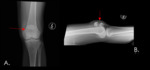
- Lateral radiograph is the modality of choice for diagnosing this injury demonstrating a bone fragment retracted proximally from anterior tibial site of tubercle ossification center.
- Ogden Classification system
- Type 1 fractures involve only the distal portion of the tubercle with or without displacement.
- Type 2 fractures involve the entire ossification center of the tubercle in which there may be separation of the tubercle from the proximal tibia or fractures are comminuted.
- Type 3 involve the entire tubercle ossification center and extend through the proximal tibial epiphysis into the joint space with or without displacement.
Treatment
- Nonsurgical treatment is for patients with minimally displaced fractures limited to the distal tibial tubercle.
- Surgical management is with open reduction internal fixation and removal of entrapped soft tissues.