Materials and Methods:107 patients,
who were referred for MRI hand with hand/wrist pain,
were included in the study from 2013 to 2015 and were followed up with histopathology reports.
A standard imaging protocol:
1.Multiplanar conventional T1-WI ,
2.Fat-suppressed fluid-sensitive (fat-suppressed T2WI ,
or STIR) and
3.
Unenhanced and contrast-enhanced fat-suppressed T1 WI sequences.
Out of 107 cases,
histopathological diagnosis was established in 39 patients.
The histopathology and MRI of these 39 patients were analyzed retrospectively.
Results of MRI,
based on the criteria followed,
were represented in Table no 1.
36 benign and three malignant cases were diagnosed ,
based on the following imaging approach.
In this study- one case (out of 39) presumed to be a benign neoplasm,
turned out to be malignant neoplasm on histopathology; ( Presumed to be neurofibroma on MRI,
was diagnosed as malignant peripheral nerve sheath tumour on HPE).
Another one case (out of 39) showed imaging characteristics of a benign neoplasm,
diagnosed to be tumour-mimic on histopathology; (Presumed to be GCT of tendon sheath on MRI,
was established as venous ectasia with thrombus,
on HPE) .
Approach:
Clinical history is prime and foremost to be considered. Duration of the lesion,
associated constitutional symptoms,
other co-morbidities have a significant value in arriving at differential diagnosis,
especially in excluding infective from non-infective inflammatory causes and differentiating aggressive from indolent lesions.
MR images of patients were analyzed based on the following four criteria.
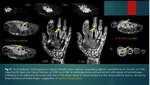
1. Location of the lesion- Sub-ungual region ,
sub cutaneous plane,
intermuscular plane,
tendon sheath,
peri-articular,
along the neurovascular bundle.
2.
Extent – single compartment / multi-compartmental.
3. Signal characteristics on MRI – fat,
fibrous tissue,
solid/cystic nature,
hemosiderin deposition,
vascular nature etc.
4.
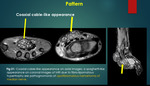
Pattern - Contrast enhancement pattern, specific imaging patterns like coaxial cable bundle appearance/ spaghetti like appearance.
1) 1.
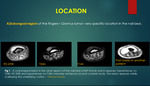
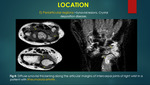
Location:
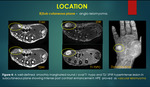
A] Subungual location: Following tumors can occur in subungual location such as benign solid tumors (glomus tumour,
subungual exostosis,
soft-tissue chondroma,
keratoacanthoma,
haemangioma,
lobular capillary haemangioma),
benign cystic lesions (epidermal and mucoid cysts),
and malignant tumours (squamous cell carcinoma,
malignant melanoma).2
Among them glomus tumor,
epidermal inclusion cyst and vascular malformations are the commonest tumours.
Glomus tumour: It is considered as hamartoma arising from glomus body which is a specialized arterio-venous anastomosis that helps in thermo-regulation.
Glomus bodies are present throughout the body,
however more concentrated in the digits,
palms,
and soles of the feet.
Although glomus tumours may affect any area of the body,
up to 75% occur in the hand,
and approximately 65% of these are in the fingertips,
particularly in the subungual space.
Clinical triad of excruciating pain,
intense tenderness that may be provoked by mild trauma,
and temperature sensitivity is specific for glomus tumour.
The most common site for glomus tumour is nail bed of the fingers.
Glomus tumour appears hypointense on T1WI,
hyperintense on T2WI and shows characteristic intense arterial enhancement with tumour blush on post contrast study due to high flow intra-tumoral vessels and subungual location is more specific for glomus tumor {figure 1}.
The literature varies,
with the prevalence of bone erosion estimated at
15-65%3,
4,5.
In the present study we observed smooth scalloping of the bone.
Squamous cell carcinoma,
although rare is the most common malignant lesion of subungual location.2
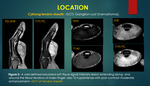
B] Subcutaneous plane:
Following tumors can arise in the subcutaneous plane such as epidermal inclusion cysts,
hemangioma,
vascular malformations,
angioleiomyoma and nerve sheath tumours.
Clinical history of trauma plays an important role in the diagnosis of epidermal inclusion cyst due to entrapment of epidermal fragments in other tissues by trauma or an iatrogenic injury,
most common site being nail bed,
subcutaneous plane and intradermal planes.
MR shows a well-circumscribed lesion of fluid signal intensity,
which varies depending on the amount of internal keratin debris.
Lack of central enhancement with peripheral enhancement is characteristic finding of epidermal cysts that helps in distinguishing these lesions from neurogenic tumours or sarcomas; If present close to tendon sheath can be confused with ganglion cysts2,6.{Figure 2a}.
Vascular anomalies include both vascular malformations (dysplastic vascular channels with normal turnover) and vascular tumours such as hemangioma (due to cellular proliferation and hyperplasia) can occur in subcutaneous plane.
{Figure2b}. Vascular malformations are subcategorized according to their flow dynamics as low-flow malformations (venous,
lymphatic,
capillary,
{Figure 3} capillary-venous,
and capillary-lymphatic-venous) and high-flow malformations (arteriovenous malformations [AVMs] and arteriovenous fistulas [AVFs]).
Angioleiomyoma is more common in lower extremities and is an uncommon tumor in hand,
due to the minimal amount of smooth muscle in this location.
Leiomyoma can arise from medial layer of vessel,
non-striated muscle of erector pili in dermis or deep soft tissue.
Commonly this lesion is misdiagnosed as other common benign soft tissue lesions. It appears as a well circumscribed lesion,
hypointense on T1,
hyperintense on T2 and intensely enhances on arterial phase with progressive enhancement9,10.
{Figure4}
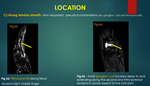
Nerve sheath tumors such as Neurofibroma/ schwannoma / Malignant fibrous histiocytomas (MFH ) can also occur.
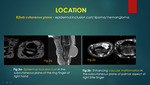
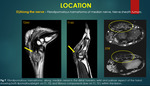
C] Along tendon sheath:
Benign and malignant lesions occurring along the tendon sheath are as follows: Giant Cell Tumour (GCT) of the tendon sheath / Pigmented villonodular tumour of the tendon sheath (PVNTS),
tenosynovitis,
nodular synovioma,
sarcoma etc.
GCT of tendon sheath occurs along any tendon of hand and presents as painless
masses in 30–50 years age group,
with a slight female predilection.
These are probably reactive benign lesions secondary to adjacent inflammatory changes,
rather than true
neoplasms.
On MRI,
these lesions appear intensely hypo intense on T2WI,
intermediate and hypo intense on T1WI and shows susceptibility artifacts on GRE with strong enhancement on post contrast study5,11.
{figure 5}.
Non neoplastic pseudo-tumoral lesions,
like ganglion cyst and tenosynovitis are to be ruled out .
Tenosynovitis could be secondary to infection/ inflammatory conditions which extends along the tendon sheath with synovial thickening, free fluid and no obvious mass6.
{Figure 6}.
D] Along the nerve bundles:
Both benign and malignant lesions can occur along the nerve sheaths,
benign being more common.
Fibrolipomatous hamartoma of medina nerve is an example of hamartoma of nerve that occurs along the median nerve12.
{Figure 7 }
E] Peri-articular regions:
Synovial lesions,
Crystal deposition diseases (Gout / CPPD) can occur in this regions.{Figure 8}.
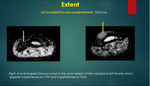
2) Extent
A] Confined to single compartment:
Predominantly,
benign soft tissue lesions are confined to single compartment.
Examples include glomus tumour3,4 {figure 9},
epidermal inclusion cyst2,6 {figure 2a},
vascular Leiomyoma9,10 {figure 4}.
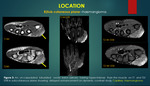
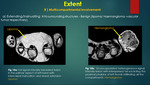
B] Insinuating (not infiltrating) into the multiple compartments:
Some benign tumors extend beyond one compartment and insinuate into the other compartments of the hand,
without infiltrating adjacent structures.
Examples include Lipoma13,14,
Hemangioma7,8.
{Figure 10a,
figure 10b respectively}.
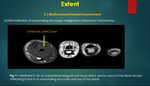
C] Infiltrating multiple compartments:
Aggressive lesions,
in contrast to benign lesions,
infiltrate the surrounding structures with loss of intervening fat plane.
Malignant soft tissue tumours like MFH,
soft tissue sarcomas etc14 are under this category.{Figure 11}.
3) MR signal characteristics: Based on typical signal characteristics the lesions can be categorized into following groups.
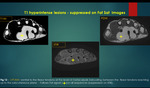
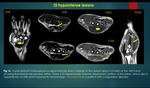
A] Hyperintense lesions on T1 WI :
i) Suppressed on fat suppressed sequences
Fat - Lipoma,
,
Fibrolipoma,
Fibrolipomatous hamartoma of median nerve,
Macrodystrophia lipomatosa,
Haemangioma,
Myositis ossificans (mature),
Liposarcoma
Lipoma / liposarcoma: Simple lipoma has homogeneous signal intensity and follows fat signal on all pulse sequences,
whereas liposarcoma has enhancing septations / nodules /soft tissue elements within13,14.
{Figure 12}
Macrodystrophia lipomatosa: It is an unusual,
congenital,
non-hereditary,
developmental anomaly resulting in local gigantism secondary to marked hypertrophy of all mesenchymal elements such as bone,
tendons,
nerves,
vessels,
and particularly fibro-adipose tissue16.{Figure 13}
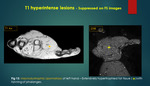
ii) Not suppressed on fat suppression sequences14
o Methemoglobin - Hematoma {figure 14a}
o Proteinaceous material - Ganglion,
abscess{figure 14c}
o Melanin – Melanoma.
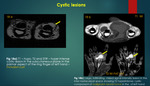
B] Hyperintense (cyst like) on T2 WI :
i) Fluid-filled lesions – Ganglia {figure 6b},
seroma,
abscess,
epidermoid inclusion cyst6,14 {figure 18a}.
ii) Solid tumor with or without necrotic components -Myxoid lesion,
intramuscular myxoma,
myxoid liposarcoma,
peripheral malignant nerve sheath tumor (PMNST ) {figure 18b}; synovial sarcoma14.
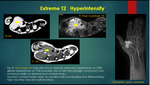
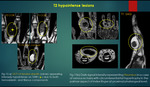
C] Extremely hyperintense lesions on T2 WI
Low flow vascular malformations7,8 {figure 19a} -Eg Haemangioma
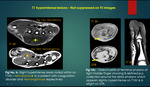
D) Hypointense lesions on T2 WI
Haemorrhage {figure 16},
thrombus {figure 15 b},
fibrous content in a tumour {figure 15 a} ,
highly cellular tumour {figure 17}.
Lesions with acute-subacute phase of haemorrhage,
appear hypointense on T2 WI and iso-to-hypointense on T1WI,
due to deoxy-hemoglobin.
Acute fibrin-rich thrombus appears dark on T2 WI and GRE sequences.
Lesions with fibrous content are persistently dark on both T1 and T2 WI.
Tumours with high cellularity,
shows hypointense signal on T2 WI and diffusion restriction with corresponding low values on ADC maps,
due to high nuclear-cytoplasmic ratio.
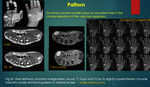
4) Pattern
i) Enhancement characteristics:
Dynamic contrast (sequential contrast enhancement) study plays an important role in establishing the vascular nature of the tumours and differentiating tumours with high vascularity (like vascular leiomyoma9,10 ) from vascular malformations( high flow or low flow) 7,8 {figure 19}.
{figure 20}.
Vascular malformation with an arterial component is considered high flow (AVMs and AVFs) while those without an arterial component are considered low flow7,8 (venous,
lymphatic,
capillary,
capillary-venous,
and capillary-lymphatic-venous).
Dynamic contrast also depicts heterogeneous enhancement of malignant lesions14,
due to presence of necrotic areas.
ii) Characteristic pattern :
Fibrolipomatous hamartoma (FLH) most commonly involves the median nerve,
though the reason for this predilection is unclear.
Chronic microtrauma from the carpal ligament or flexor retinaculum to median nerve has been suggested.
It is a benign overgrowth of fibrous and adipose tissue within a nerve sheath and is quite rare.
Clinical presentation is often with a progressive palmar tumefaction and a median compression neuropathy during childhood.
Traumatic neuromas,
ganglion cysts,
lipomas and vascular malformations are the differentials to be considered.
On the axial and coronal images,
enlargement of median nerve and nerve fascicles due to fibrous and adipose tissue overgrowth.
This has been described as a ‘cable-like’ appearance on axial,
spaghetti like on coronal images and is pathognomonic for FLH12.{Figure 21}
Differentiation of benign versus malignant soft tissue lesions based on imaging:
Inspite of the characteristic imaging features of malignant soft tissue tumours (Table No 2), they might also have smooth margins,
uniform signal intensity and homogeneous enhancement.
Though MRI is known for high soft tissue contrast and spatial resolution that helps in characterization of the lesions,
it is not specific for distinguishing malignant lesions from benign.