As an institution with high rate of SCD in the local population,
we have access to a rich source of imaging,
including early manifestations,
appearances during treatment,
and late presentations.
An illustrated review of imaging appearances of skeletal manifestations of SCD,
with examples of common and important skeletal manifestations,
is therefore presented.
Persistence and expansion of intramedullary haematopoietic marrow
In normal physiology,
red marrow is present throughout the skeleton at birth,
with conversion to yellow fatty marrow occurring with age.
In normal adults,
red marrow is only present within the axial skeleton.
However,
in SCD patients there is a chronic anaemic state,
and this acts as a stimulus for red blood cell production,
resulting in persistence and hyperplasia of appendicular red marrow in adults.
Furthermore,
the continual production of red blood cells results in medullary expansion and cortical thinning,
and this increases the risk for pathological fractures.
Signs of intramedullary hyperplasia may be subtle on plain radiographs,
with coarsening of the trabecular pattern sometimes demonstrated in the long bones.
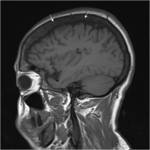
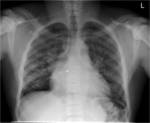
Within the skull,
marrow expansion is indicated by the thinning of the inner and outer tables and widening of the diploic space.
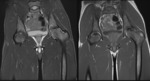
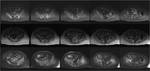
On MR imaging,
haematopoietic red marrow demonstrates isointense/ low T1w and T2w signal (relative to muscle),
in contrast to the normal high T1w and T2w signal returned from yellow marrow (Figure 1).
If gradient –echo sequences are performed,
there may be blooming artefact secondary to haemosiderin deposition from repeated blood transfusions.
Bone infarction
Bone infarction is an important skeletal pathology which occurs due to the occlusion of microvasculature supplying the bones.
The abnormal red blood cells produced in SCD have a propensity to sickle within the bone marrow,
leading to stasis of blood and therefore occlusion of the microvasculature,
with resultant ischaemia and infarction.
 Clinically,
acute bone infarction may present with painful bone crises,
or it may be clinically silent.
Clinically,
acute bone infarction may present with painful bone crises,
or it may be clinically silent.
Infarction commonly affects the long bones within children and adults,
and there are variable plain radiographic appearances depending on the timeframe.
In acute infarcts,
there is often a normal appearance,
although osteolysis and a periosteal reaction may rarely occur.
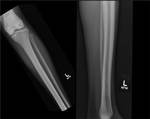
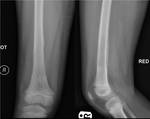
In chronic infarcts,
there may be serpiginous calcification,
or more commonly patchy sclerosis (Figure 2).
In non-long bones such as the spine,
ribs and pelvis,
there is marked sclerosis,
secondary to dystrophic medullary calcification that occurs after medullary infarction.
In children,
the diaphyses of tubular bones within the hands and feet may become infarcted,
leading to a clinical presentation of fever and swollen hands and feet,
known as “hand-foot syndrome”.
Plain radiographs demonstrate initial periosteal reaction,
followed by patchy sclerosis.
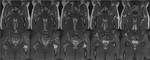
On MRI,
acute bone infarcts present with signs of oedema,
with low T1w and high T2w signal returned at affected areas.
Similarly,
high signal is seen on T1 fat-saturated sequences (Figure 3).
If intravenous contrast is given,
there is thin linear enhancement surrounding the affected areas.
In chronic infarction,
there is a classical serpiginous pattern,
characterised by low T1w signal and high T2w signal outlining the red marrow.
Additionally,
T2w sequences may demonstrate an outline composed of both low and high signal,
resulting in a “double line” appearance.
Avascular necrosis
Avascular necrosis is a common skeletal presentation in SCD,
occurring due to microvascular occlusion and subsequent ischaemia within the epiphyses.
The most frequently affected sites are the humeral and femoral heads.
Initial plain radiographs are often normal,
although subtle signs such as increased central density sometimes may be appreciated.
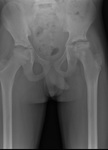
As the process progresses,
there may be crescenteric subchondral lucency,
with eventual flattening,
collapse and fragmentation of the articular surface (Figure 4 and 5).
The vertebral bodies are also typically affected by avascular necrosis,
presenting with initial sub-endplate sclerosis,
followed by collapse of the central endplates and formation of a characteristic “H” shaped vertebra (Figure 6).
Similar to bone Infarction,
avascular necrosis usually presents with signs of bone marrow oedema on MRI (low T1w and high T2w signal).
In established avascular necrosis,
there is often a serpiginous “double-line” rim on T2w sequences,
composed of an inner hyperintensity line and an outer hypointensity line,
that surrounds the affected weight-bearing region (Figure 7 and 8).
Infection
Infections including osteomyelitis,
and less commonly septic arthritis,
are significant complications which are more prevalent in SCD,
due to a combination of factors including reduced immunity secondary to hyposplenism (from infarction) and presence of a favourable culture medium provided by infarcted and necrosed bone.
Osteomyelitis in SCD patients is usually caused by Salmonella bacteria species,
with Staphlococcus aureus infections being less common.
Clinically,
osteomyelitis presents with localised pain and swelling of the affected region,
in conjunction with fever and raised inflammatory markers.
This clinical presentation is similar to that the presentation of painful bone crises,
and distinction between the two entities is challenging but important in order to avoid unnecessary antibiotic treatment.
Acute osteomyelitis may often initially demonstrate normal appearances on plain radiographs,
although features such as periosteal reaction,
osteopaenia and sclerosis may be seen (Figure 9).
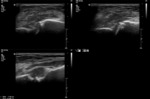
Ultrasonography of osteomyelitis may be helpful,
particularly in children,
and may demonstrate associated soft tissue inflammation and collections,
in addition to visualising cortical breaks and periosteal reaction.
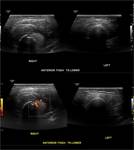
In septic arthritis,
ultrasonography is useful in terms of confirming the presence of a joint effusion,
and guiding aspiration (Figure 10 and 11).
On MRI,
regions affected by osteomyelitis demonstrate low T1w signal,
although this may be indistinguishable from the low T1w signal appearances of red marrow hyperplasia.
Fluid sensitive sequences demonstrate high signal intensity within the affected regions,
and this high signal extends into the surrounding soft tissues,
in keeping with adjacent soft tissues oedema and inflammation (Figure 12). This feature of soft tissue involvement is not usually seen with bone infarct and can be used as a distinguishing characteristic.
On post-contrast sequences,
there is irregular rim enhancement,
surrounding a non-enhancing centre,
and adjacent soft tissues also demonstrate avid enhancement.
MRI appearances of septic arthritis include synovial enhancement post-contrast administration,
and perisynovial oedema.