To avoid complications a meticulous procedure has to be performed and
thorough preparation is essential.
Some general precautions have to be observed
1.
Check the coagulation status.
Any patient under anticoagulant therapy should be discontinued as long as the risk - benefit ratio advises the injeccion Fig. 4
2.
Informed consent.
Patients have to be informed and sign a document describing the procedure,
any posible complication and treatment alternative.
3.
Anesthesia.
All the procedures decribed can be performed with the patient under conscious sedation using local anesthesia (lidocaine 1%),
however,
general anesthesia may be necessary in children or uncooperative patients.
Painful lesions,
such as neurogenic tumors,
or lesions in the hand and foot may require a regional nerve block.
Liberal periosteal anesthetic infiltration is often helpful to minimize pain.
Spinal epidural and foraminal injections.
Steroids are widely used to treat back pain due to disc herniations,
spinal stenosis or post surgical syndromes.
Once the patient is elegible for the procedure the optimal approach is selected by agreement between the clinician and the radiologist regarding a) the patient´s symptomatology b) preliminary image findings and c) accesibility.
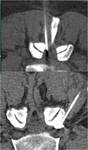
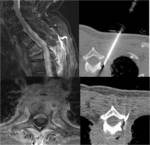
Approaches used are interlaminar and foraminal Fig. 5
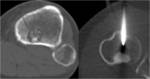
The patient in placed in prone position precise slice for entry level depending on pathology and patient anatomy is selected.
A marker is placed and the patient's skin sterilization of,
local anesthesia (1% lidocaine) and needle introduction (Chiba 22-23G) is performed Fig. 6.
After correct needle placement and contrast distribution is checked,
the steroid can be administered ( in our institution Dexametasona 12mgs).
Reported complications are rare including infection,
bleeding,
headache,
local discomfort ,
vasovagal,
lipodystrophy ,allergic reactions,
systemic corticosteroid effects,
transient increase in pain and medullary infarction.
To avoid medullary infarction it is important to keep the needle tip in the posteroinferior corner of the foramina and employ non particulated steroids (dexametasona).
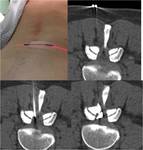
Spinal synovial cyst
They are cystic formations connected to the facet joint and containing synovial fluid lined by a cuboid or pseudostratified columnar epithelium. They may proyect onto the epidural space and result in lumbar radiculopathy in a significant number of cases.
They can be treated by CT guided access using a spinal needle.
Once an intracystic location is confirmed with contrast,
rupture of the cyst is attempted using a steroid and anaesthetic Fig. 7
Bone and disc lesions biopsy.
Spondilodyscitis and focal bone tumors can be biopsied using bone core needles.
Appropriate paths are to be known in each different location (spine,
limbs..) to avoid potential complications.
When dealing with bone,
bone biopsy dedicated needls are mandatory.
Lidocain administered in the skin,
needle path and specially in periostium is usually enough to comfortably perform the procedure.
Once the Chiba needle is placed in the proper path,
it is easy to remove the needle cap with a swinging motion,
providing a guide to place the thicker bone biopsy needle.
Fig. 8
Spondilodyscitis
Definitive microbiological and histopathologic diagnosis is often required for optimal management,
unless blood cultures guide the treatment open biopsy and cultures remain the reference gold standard for diagnosis.
Paravertebral soft-tissue changes,
when present,
may be considered a
viable target for biopsy in cases of diskitis-osteomyelitis,
even in the absence of a paravertebral abscess Fig. 9
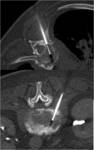
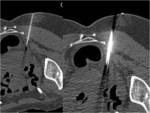
Sometimes its mandatory to access into the vertebral disc
In dorsal spine the access through the costovertebral joint is safe and easy to perform driving the needle directly to the disc
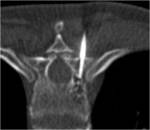
In lumbar spine posterolateral approach is most commonly used path Fig. 10 Sometime transpedicular approach can also be used.
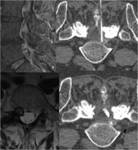
Bone lesions
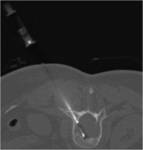
Spine bone lesions can be accessed using the same paths as the discs but the transpedicular approach is the most employed Fig. 11
It is not unusual to use the bone set to access the lesion and perform the biopsy using a trucut needle though it since the bone biopsy needle is not very well suited to obtain soft tissue samples Fig. 12
When dealing with bone lesions locaed in the limbs,
the radiologist and the orthopedic oncologic surgeon should take a team approach, especially when the bone lesion might be a primary sarcoma for which limb-sparing surgery would be considered. Comprehensive planning guidelines for image-guided needle biopsies of potential sarcomas in the long bones of the extremities have been proposed regarding the relationships of the bones,
compartmental anatomy,
and neurovascular structures,
based on the standard surgical approaches used for limb-sparing surgery of the extremities.
Fig. 13
Complications
Complications are very unusual and include Hemorrhage,
Neurological injury,
Pneumothorax and Infection- meningitis.
Careful planification and strict adherence to safety measures are the best way to avoid them.
Percutaneus abscess drainage.
Pus at any location should be drained.
Usually this procedure is performed under ultrasound guidance.
Nontheless collections located in some US-guided difficult to access locations,
are more easily managed with CT-guided techniques.
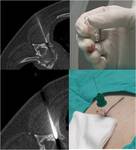
We employ trocar system Fig. 14 to perform this procedure,
the procedure is done in two steps:
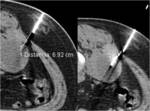
1.- Chiba needle is inserted until it reaches the collection,
injecting anesthetic alog the pathway
2.-The trocar can be inserted directly into the collection in parallel,
using the chiba as a guide,
once the correct location is stated,
the pigtail catheter can be released,
it is important to make sure that all the catheter holes are inside The abscess.
In our experience deep pelvic and paravertebral-psoas located collections are most frecuently managed under ct guidance.
Fig. 15 Fig. 16
Precautions:
-Some organs can be transversed such as Stomach,
Liver,
Pleural space (recess),
Bladder.
-Always avoid gall bladder,
intestine,
spleen,
kidneys and pancreas.
-Do not go through thick vessels or epigastric artery
-In organs use the shortest path
Complications:
Hemorrhage Bacteremia.
Septic shock Hollow visceral perforation