Case study (Patient 1):
A 78 year old male,
who had a left total hip replacment 18 years ago.
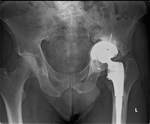
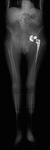
Plain radiographs (Fig. 1 Fig. 2 Fig. 3) were obtained 7 years ago,
when he presented with occasional pain in the left hip joint,
associated with excessive activity and relieved over time with rest.
In September 2016,
the patient presented with severe pain in his left hip and marked restriction of movements.
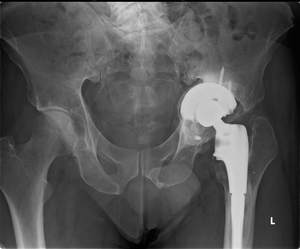
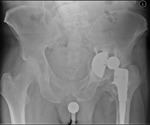
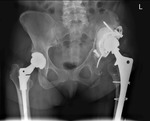
Fig. 1: Patient 1 - preoperative AP pelvic radiograph
References: Amanda Isaac
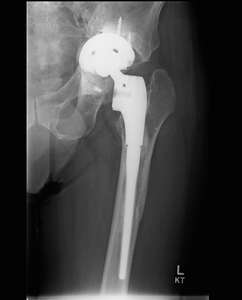
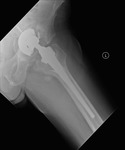
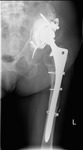
Fig. 2: Patient 1 - preoperative AP left hip radiograph
References: Amanda Isaac
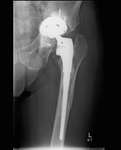
Plain radiographs obtained (Fig. 4 Fig. 5 Fig. 6) demonstrated loosening of the acetabular component with superior and medial migration of the acetabular component and massive bone loss.
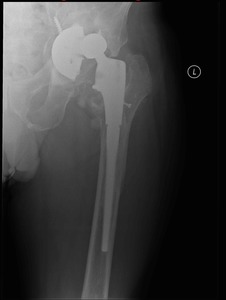
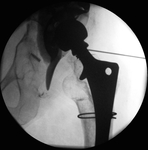
Fig. 4: Patient 1 preoperative plain radiograph of the left hip joint.
The patient presented 5 years later with massive bone loss, loosening of the acetabular cup and dislocation of the cup
References: Amanda Isaac
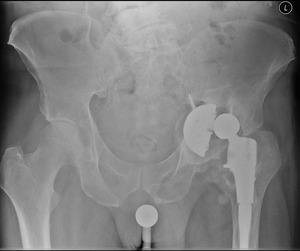
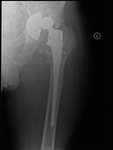
Fig. 5: Patient 1 preoperative plain radiograph of the left hip joint.
The patient presented 5 years later with massive bone loss, loosening of the acetabular cup and dislocation of the cup
References: Amanda Isaac
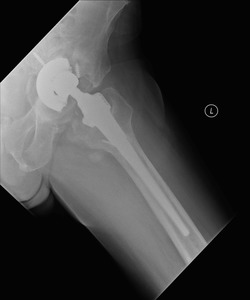
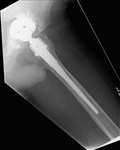
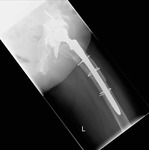
Fig. 6: Patient 1 preoperative lateral plain radiograph of the left hip joint.
The patient presented 5 years later with massive bone loss, loosening of the acetabular cup and dislocation of the cup
References: Amanda Isaac
A subsequent MRI was performed (Fig. 7 Fig. 8 Fig. 9) and demonstrarted loosening of the acetabular component with periacetabular cystic change in the bony pelvis.
The extent of bone loss could not be assessed due to marked superimposed metal artifact.
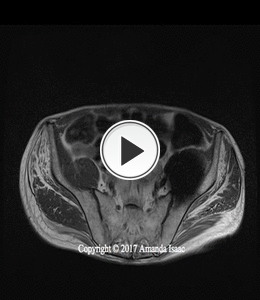
Fig. 7: Patient 1 - MRI Axial T1 post contrast MARS protocol demonstrating metal artefact as well as marked fatty atrophy of the muscles around the left hip
References: Amanda Isaac
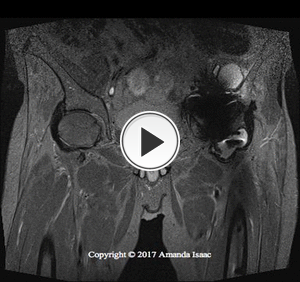
Fig. 8: Patient 1 - MRI Coronal STIR demonstrating numerous cystic cavities circumferential to the prosthesis
References: Amanda Isaac
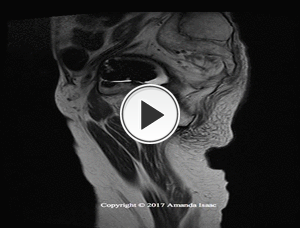
Fig. 9: Patient 1 - MRI sagittal STIR demonstrating cystic cavities around prosthesis
References: Amanda Isaac
A CT scan (Fig. 10 Fig. 11) was therefore requested which confirmed bone loss and remodelling of the acetabulum,
but image analysis was limited by metal artifact and 2D imaging,
despite obtaining multiplanar reformats.
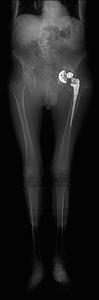
Fig. 10: Patient 1 - CT scout, demonstrating limb length discrepancy, pivotal to pre-operative planning
References: Amanda Isaac

Fig. 11: Patient 1 - MDCT axial acquisition for pre-operative planning
References: Amanda Isaac
The patient was discussed in our weekly hip MDM and a questionnaire was completed by all three hip surgeons,
who were blinded to their colleagues' responses.
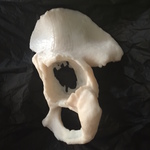
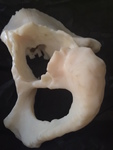
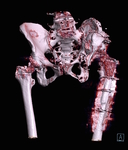
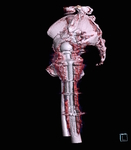
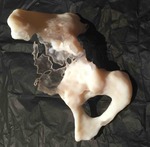
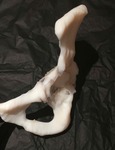
A 3D patient specific model was subsequently produced (Fig. 12 Fig. 13 Fig. 14 Fig. 15 Fig. 16),
presented at the hip MDM and the same questionnaire was completed by all three surgeons.
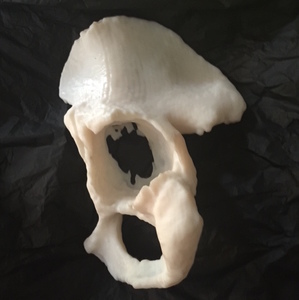
Fig. 12: Patient 1 - 3D printed model 1:1 scale (true to size)
References: Amanda Isaac
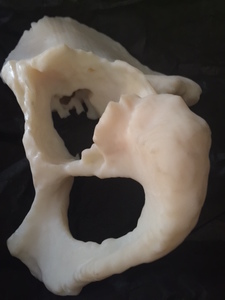
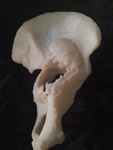
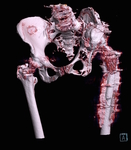
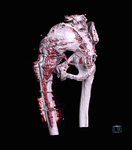
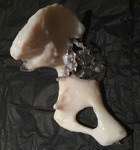
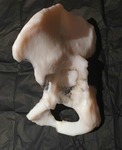
Fig. 13: Patient 1 - 3D printed model 1:1 scale (true to size)
References: Amanda Isaac
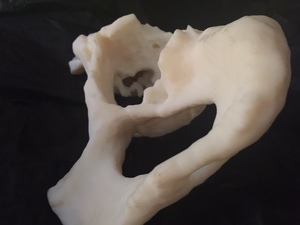
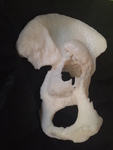
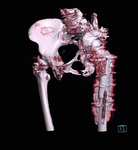
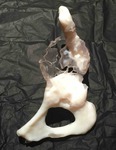
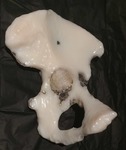
Fig. 14: Patient 1 - 3D printed model 1:1 scale (true to size)
References: Amanda Isaac
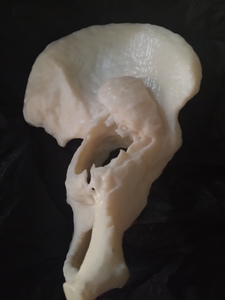
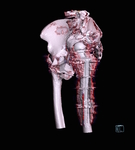
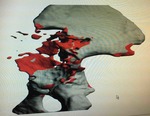
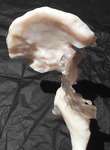
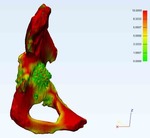
Fig. 15: Patient 1 - 3D printed model 1:1 scale (true to size)
References: Amanda Isaac
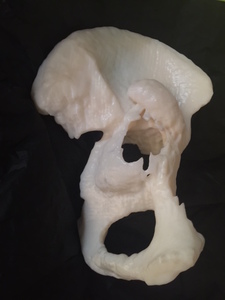
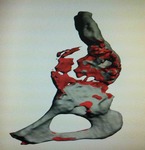
Fig. 16: Patient 1 - 3D printed model 1:1 scale (true to size)
References: Amanda Isaac
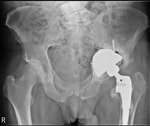
The operation was successfully performed for complex revision hip arthroplasty (Fig. 17).
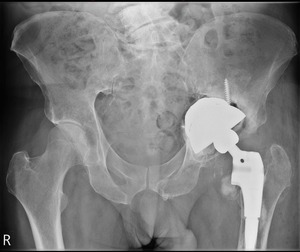
Fig. 17: Patient 1 - post revision AP pelvic radiograph
References: Amanda Isaac
Intraoperative data collected includes:
- Surgical time: 4 hours and 3 minutes.
- Anaesthetic time: 5 hours and 33 minutes.
- Intraoperative blood loss: <500mls.
Hb preoperative 133 and 98 postoperative.
Did not require a blood transfusion post procedure.
- Hospital stay: 5 days
- Prosthesis cost: £4000 (TMARS implant by Zimmer).
- Loan kit cost: £200-600
The cost of the 3D model was £748.
The total savings using 3DP were estimated to be >£2000.
An alternative to using this 3D model was to use a custom made implant,
costing £12,000-£16,000 instead of the "off the shelf TMARS implant" used.
Four other cases from our pilot study are also included in this presentation to demonstrate the extent of variability and complexity of complex revision hips,
the limitations of current conventional 2D imaging and to illustrate the value of 3DP applications to accurately evaluate bone thickness,
bone quality and the configuration of residual bone following massive bone loss.
Overall,
our pilot study has proven to:
- Shorten the operative time by 30-90 minutes,
reducing the costs of theatre & staff time,
allowing more procedures to be performed on the day,
thus reducing waiting lists.
- Reduce the excess of pre-ordered prostheses,
lowering shelf- kit loan costs and overall operative costs.
- Subjectively improve patient outcomes through reduced anaesthetic time,
intraoperative manipulations with associated blood loss and soft tissue bruising.
- Improve the surgeon’s confidence in preoperative planning through the choice of appropriate prosthesis,
position and trajectory for screw placement.
- Allow for "elective" peer review discussion of the case in an MDM setting.
Traditionally,
decisions can only be made intraoperatively,
once the old implant is removed,
as the acetabular bed is prepared and the extent of bone loss and residual bony configuration is established.