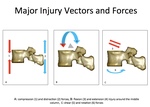
MORPHOLOGICAL PATTERNS
It is well recognized that,
on the basis of a specific trauma mechanism,
characteristic findings are observed.
In general compressive forces result in wedge or burst fractures,
distractive forces in ligametous disruption or dislocation,
while rotation-shear forces result in combined bone and ligamentous injuries producing fracture dislocation (Fig.
4).
The major types of thoracolumbar spine injury are described according to the mechanism of injury: compression or wedge,
burst,
flexion-distraction or Chance and fracture dislocation.
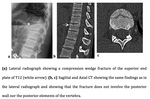
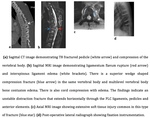
Anterior Wedge Compression Fractures (Fig.5)
The mechanism of injury is axial loading with or without a flexion component.
The classic imaging finding is of a wedge-shaped vertebral body compressing the anterior cortex and sparing the middle and posterior columns.
The wedge is particularly visible on the lateral radiograph.
Radiologic stability is best assessed by CT,
which will verify the integrity of the posterior wall and of the vertebral arch,
the exact amount of loss of vertebral body height and the fracture line.
MRI is not essential,
it shows marrow edema as a secondary indicator of fracture and can reveal hidden trabecular fractures of adjacent vertebral bodies7.
The treatment is non-surgical,
rarely,
may be surgical in order to prevent secondary spinal deformities.
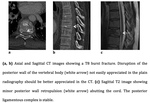
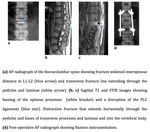
Burst fracture (Fig.6,
7)
The burst fracture is produced by pure axial compression that involves at least the anterior and middle columns.
Is distinguished from an anterior wedge compression fracture by a disruption of the posterior cortex of the vertebral body (ie,
middle column),
which can be displaced into the spinal canal (retropulsed fragment) and may cause compression or even disruption of the neural structures2.
Radiographically usually shows a wedge-shaped vertebral body with widened interpedicular distance.
CT often performed immediately,
shows the degree of posterior retropulsion,
any posterior displacement of bone fragments into the spinal canal and evaluates the size of the residual vertebral canal.
It not uncommonly also shows associated injury to the spinous process or facet joints nor appreciated on radiographs.
MRI is indicated where there is neurological symptomatology,
to highlight contusion-impaction of the adjacent vertebrae,
to assess continuity of the PLC (a determining factor as regards conservative or surgical treatment8) and to determine the effects of the fracture on the spinal canal and neural structures.
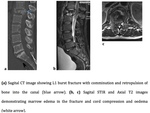
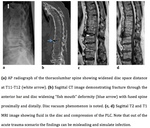
Chance fracture (Fig.8,
9)
Chance-type spinal injuries result from hyperflexion of the spine around an anterior fulcrum in combination with a posterior distracting force.
A Chance fracture involves compression of the anterior column with distraction of the middle and posterior columns (3-column injuries).
The term “distraction” refers to a complete separation at the fracture site of bone fragments in a cranio-caudal direction or a widened interspinous process distance.
In general,
in high-speed injuries a combination of an axial load and flexion causes the upper body to rotate forward while the lower body is fixed,
classically described as a “seat belt” injury in a motor vehicle injury.
They can be purely bone,
purely disco-ligamentous (rare) or mixed.
A classic Chance fracture is a horizontal fracture through the spinous process,
the lamina,
the pedicles,
the intervertebral disc space,
and the posterior longitudinal ligament,
SSL and ISL.
On radiography the findings include wedging of the anterior vertebral body and increased inter-spinous distance,
which implies posterior ligamentous distraction,
and disruption of the pedicles often bilaterally,
which can be appreciated on the radiograph as ‘elongation’ of the pedicles.
The CT is often done immediately.
Chance fractures are most often high kinetic trauma and associated with a high rate of abdominal viscera injury4.
CT is more sensitive,
with the sagittal reformatted image showing a horizontally oriented fracture extending across the posterior elements and continuing into the vertebral body with more separation of the fragments posteriorly.
MRI is essential for the accurate understanding,
documentation,
and depiction of osseous and soft-tissues injuries that occur in Chance-type spinal injuries9.
Non-displaced fractures consisting of bone only can be treated conservatively.
Discoligamentous injuries have a poor prognosis for healing unless surgical treatment is performed.
Although more rare,
extension distraction type fractures (Fig.10) can also occur typically in the rigid spine.
These are also unstable fractures (3 column-injuries).
The fracture starts in the anterior column and follows a transcorporeal or transdiscal path before reaching the neural arch.
They are frequently ignored and the appearance misleading simulating an infection or a tumour.
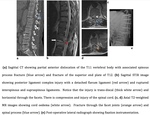
Fracture Dislocation (Fig.
11)
Fracture dislocations of the thoracolumbar spine can occur as a result of combined shearing,
flexion and rotation forces to the spine.
They variably combine dislocations in various planes.
These are very unstable injuries,
the fracture and ligament damage typically involves all three columns,
and the vertebrae are often drastically malaligned and displaced.
They are often associated with neurological lesions CT shows vertebral column discontinuity and listhesis at the level of injury,
complete disruption of the intervertebral disc,
or horizontal fracture through the vertebral body with displacement and/or rotation.
Horizontal fracture through the facets with anterolisthesis and fracture through the neural arch may also be demonstrated.
MR is essential to characterize spinal cord,
ligaments and intervertebral disc to assess the extent of the respective soft tissue disruption.
Treatment is surgical to stabilise the spine on account of the very extensive ligamentous disruption and often malaligned vertebral column.