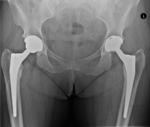
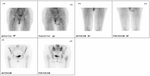
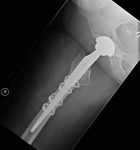
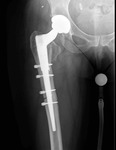
339 patients underwent primary hip arthroplasty in our institution using the Corail® Total hip system between 2008 and 2016; of which:
31 patients (9.14%) had bone scans (28 had symptoms,
3 had scans for other reasons including two patients with total knee replacement with possible infection or loosening and one patient to investigate malignancy (was negative).
Out of three asymptomatic patients 1 had increased uptake around the Corail® implant (incidence 1 in 339,
0.29%) within 1 year from surgery.
Out of 28 patients with hip or thigh symptoms within 9 years of THR surgery (incidence of 8.26%):
- 2 patients (0.59%) had revision for infection
- 4 patients (1.18%) had revision for loosening
Therefore 6 patients (1.77%) required revision surgery within 9 years.
- 5 patients (1.47%) had causes of pain unrelated to hip (Spine,
ITB,
psoas tendonosis)
- 5 patients (1.47%) had hip pain but negative SPECT and normal radiographs.
Therefore there were 10 patients (2.95%) where imaging and serological investigations could not identify a cause directly related to the implant.

Fig. 7: 9 year outcomes
References: Danoob Dalili
12 patients (3.54%) had positive SPECT-CT scans but their symptoms resolved over time.
Serological investigations remained equivocal and those imaged had no radiographic changes over serial imaging.
Those who were investigated with follow up SPECT demonstrated reduced tracer uptake over time.
In nine (10/12) patients the symptoms completely resolved over 6 months and did not recur.
Two (2/12) patients subsequently developed back pain or tendonosis and initial hip or thigh pain settled over 12 months.
None of this group of patients required interventional procedures (surgery/hip injections) or developed clinical/radiological evidence of loosening or infection.
All 12 patients with positive SPECT-CT had increased osteoblastic activity in zone 1,7.
One patient also had circumferential uptake around the entire femoral component of the Corail® system.
Transient circumferential or focal increased uptake around the margins of the femoral stem was observed in a proportion of patients presenting with focal pain symptoms on dynamic movement of the ipsilateral hip.
This phenomenon was observed in patients with a history of early return to high levels of activity.
The possible explanation,
could be excessive micro motion at the bone-implant (Hydroxyapatite) interface causing an increase in osteoblastic activity.
Reducing levels of physical activity was advocated and advised,
which led to reversal of clinical symptoms and radiographic findings on serial imaging at follow up (3-9 months),
without need for any further intervention.
In patients with unresolved symptoms,
increased serological inflammatory markers & scintigraphic findings other than those described above in addition to other causes including infection and/or loosening were detected and treated with revision hip surgery.