We performed a retrospective review of cases of popliteal masses in 2016 at our institution and selected key X-ray (Xr),
ultrasound (US),
computed tomography (CT) or magnetic resonance (MR) images of the various entities.
For literature review,
we have searched indexed publications using Medline as the scientific repository for current data regarding this particular area of interest.
-
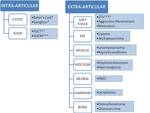
INTRA-ARTICULAR – CYSTIC LESIONS
A.1.
POPLITEAL CYST
Popliteal cyst,
or Baker’s cyst,
is the commonest posterior knee mass.
It is a painless fluid-filled mass that represents a distention of a preexisting bursa in the popliteal fossa,
most commonly the gastrocnemio-semimembranosus bursa.
This bursa is unique in that it communicates with the knee joint,
unlike other periarticular bursae,
via an opening in the joint capsule posterior to the medial femoral condyle.
Popliteal cysts rarely manifest alone and are most often found in conjunction with other intra-articular pathologies and inflammatory conditions.
In children, popliteal cysts are only occasionally associated with these conditions and are more often an incidental finding discovered during a routine physical examination.
Imaging features (figure 2):
-
US: well-defined fluid collection with the classical “talk bubble” or “speech bubble” appearance (a “neck” at its deepest extent), extending into the joint space between the semimembranosus tendon and the medial head of the gastrocnemius.
-
MR: cystic lesion with fluid signal characteristics on all sequences.
Complications:
-
Rupture - fluid leaking deep to the deep fascia and superficial to the medial head of the gastrocnemius; oedema of the soft tissue; irregularity of the cyst wall.
-
Dissection - usually inferomedially
-
Compression of the popliteal vessels and tibial nerve
-
Compartment syndrome
A.2.
GANGLION CYST (GANGLION,
GANGLIA)
Histologically,
ganglia are filled with gelatinous fluid rich in hyaluronic acid and other mucopolysaccharides and have a thin connective tissue capsule,
but no true synovial lining.
In the popliteal fossa,
ganglion cysts are often incidental and result from myxoid degeneration of the posterior joint capsule or tendon sheaths of both medial and lateral head of gastrocnemius.
Typically,
they are attached to the underlying joint capsule or tendon sheath.
Imaging features (figure 3):
-
US: anechoic to hypoechoic mass with well-defined margins; many demonstrate internal septations.
-
MR: unilocular or multilocular fluid signal mass,
adjacent to the joint or tendon sheath.
T1-weighted (T1W) images – usually demonstrate low signal intensity; intermediate signal intensity may result from high proteinaceous content or haemorrhage;
T2-weighted (T2W) images – homogeneously hyperintense.
-
INTRA-ARTICULAR – SOLID LESIONS
B.1.
TENOSYNOVIAL GIANT CELL TUMOURS (TSGCT)
Represent a diverse group of benign proliferative disorders of the synovium that may affect the joints,
bursae,
and tendon sheaths.
TSGCTs are usually divided according to the site of origin (intraarticular or extraarticular) and pattern of growth (localized or diffuse) (figure 4).
B.1.1. Pigmented Villonodular Synovitis (PVNS)
The term pigmented villonodular synovitis is generally used when diffuse intraarticular involvement is present.
The aetiology of this disease remains unclear.
Usually a mono-articular process of the large joints (occasionally oligoarticular).
The knee is involved in about 80% of cases; other affected joints,
in order of decreasing frequency,
include the hip,
ankle,
shoulder,
and elbow
Macroscopically: many villous or frondlike synovial projections with a characteristic tan or reddish color due to hemosiderin within the lesion.
Microscopically: solid or fingerlike masses of hyperplastic synovium with multinucleated giant cells,
xanthoma cells,
and intra- and extracellular hemosiderin,
lying in a fibrous stroma.
Imaging features:
-
Plain radiograph: may show normal findings or may reveal periarticular soft-tissue swelling; occasionally the fluid may appear dense,
a finding suggestive of haemorrhagic effusion; bone erosions can be seen - these occur most frequently in joints with a tight capsule,
such as the hip and shoulder (bone erosions are less common in the more capacious knee joint); visible calcifications are very unusual.
-
CT: the hypertrophic synovium appears as a soft tissue mass,
may appear slightly hyperdense compared to adjacent muscle (due to hemosiderin deposition); CT is also useful in detecting small erosions not visible on radiographs.
-
MR: technique of choice for diagnosis and follow-up in patients with PVNS because of its very specific imaging features,
which help to distinguish PVNS from other synovial processes.
Images typically show a synovial-based mass that affects most or all of the joint and that displays:
T1W and T2W images – low to intermediate signal intensity; can also contain areas of variable signal intensity,
with foci of brighter T1 and T2 signals that indicate relatively low concentrations of hemosiderin.
Gradient echo imaging: "blooming" phenomenon of hemosiderin-laden nodules (characteristic).
After gadolium administration,
marked enhancement of the synovium is common due to the hypervascular nature of the disease.
B.2. SYNOVIAL OSTEOCHONDROMATOSIS
Benign neoplastic synovial proliferation and formation of cartilaginous (chondromatosis) or osseous bodies (osteochondromatosis).
Primary Synovial osteochondromatosis (SOCM) is very rare (figure 5).
Secondary SOCM is a disorder that results in with intra-articular loose bodies as a result of trauma or arthropathy.
The knee is most commonly affected (50%).
Imaging features:
-
Plain radiograph: multiple calcified or ossified intra-articular
loose bodies of similar size,
which are distributed throughout the joint.
Secondary SOCM is typically associated with changes of the underlying degenerative disease of the joint and the intra-articular bodies tend to be larger,
less numerous,
and more varied in size and shape.
-
MR: loose bodies are of variable signal,
depending on proportion of calcium,
chondroid,
and mature ossific tissue.
-
EXTRA-ARTICULAR
C.1 SOFT TISSUE
C.1.1.
Soft-Tissue Sarcomas (STSs)
Malignant tumours of mesenchymal origin.
Classified according to the tissue of origin.
In 3-5% of the cases,
STSs occur in the popliteal fossa: are considered extra-compartmental and therefore have a poorer prognosis compared to intra-compartmental STSs due to poor surgical margins.
The commonest histological types found in the popliteal fossa include synovial sarcoma (SS),
undifferentiated pleomorphic sarcoma (figure 5),
liposarcomas and leiomyosarcomas.
Most soft-tissue sarcomas grow as space-occupying intramuscular lesions,
enlarging in a centripetal fashion that pushes rather than infiltrates local structures
Suspicious features include a soft tissue mass that is increasing in size,
has a size >5cm or is deep to the deep fascia,
whether or not it is painful.
Imaging features: soft-tissue sarcomas are tumors without specific imaging findings beyond solid enhancing,
soft tissue mass and need biopsy for histological diagnosis.
Findings depend on the type of tumour and may have internal cystic component,
myxoid tissue,
fat,
calcification or necrosis (see image 5 for more detailed features on MR images).
-
General US features: Large heterogeneous hypoechoic mass,
well-encapsulated,
usually located in deep (subfascial) tissues; commonly hypervascular with disorganized vascular pattern on colour Doppler imaging.
± Myxoid tissue: Well-defined,
intra-tumoural anechoic or hypoechoic areas.
± Necrosis: Poorly-defined hypoechoic areas.
± Calcification: Discrete intra-tumoural echogenic foci with acoustic shadowing.
± Haemorrhage: Ill-defined intra-tumoural echogenic areas without acoustic shadowing
C.1.2. Aggressive Fibromatosis (AF)
Fibromatosis is a rare mesenchymal tumour proliferation of fibroblasts and myofibroblasts with marked production of intercellular collagen.
It comprises a broad group of fibrous tissue proliferations of similar histologic appearance that has biologic behaviour intermediate between that of benign fibrous lesions and fibrossarcoma.
Occurring in almost any anatomic location,
fibromatosis can be divided into superficial and deep subtypes:
- The superficial fibromatoses are usually small (< 5 cm) slow growing lesions that rarely involve deep structures.
- The deep group consists of rapidly growing lesions that often reach a large size and have a high tendency to recur after treatment,
hence the term “aggressive fibromatosis”:
-
Principally involves the musculature of the trunk and the extremities
-
Characteristic infiltrative growth along the fascial planes,
forming intermuscular masses of soft tissue.
-
Local recurrence after surgery is high although it does not have any propensity for metastasis.
-
Imaging features (figure 6):
- Plain radiograph: either is undetectable or is identified as an amorphous soft-tissue-density mass.
Calcification is uncommon.
- US: typically shows a slightly hypoechoic,
lobulated,
or infiltrative mass.
- CT: nonspecific,
enhancing soft-tissue mass that may be iso- or slightly hypodense to surrounding muscle.
- MR: provides the optimum method of tumor evaluation
T1: homogeneous iso-intensity or mild hyperintensity
T2/STIR: high heterogenous signal
Typically enhances avidly after gadolium administration
The unusual characteristic of heterogeneous,
band-like low signal intensity areas on T1W and T2W images is a distinguishing feature of AF.
C.2.
LIPOMATOUS
C.2.1.
Lipoma
Benign lipomatous tumour composed of well-differentiated adipocytes.
They are the most common soft tissue tumour.
Well-defined,
circumscribed and encapsulated ovoid mass made almost entirely of fat,
with fine linear septations parallel to the long axis of the tumour.
Although blood vessels,
muscle fibres,
fibrous septae and fat necrosis can be seen in lipomas,
evidence of non-fatty soft tissue component,
thick or nodular septae or signs invasion are suggestive of malignant transformation.
Lipomas are characterized according to their location:
-
US: variable echogenicity depending on their cellularity and fat-water content; they are compressible and have absent or minimal intralesional vascularity on colour Doppler imaging
-
MR: Lipomas are similar to adjacent subcutaneous fat and follow fat SI on all MRI sequences.
C.3.
MUSCLE
C.3.1.
Myositis ossificans (nonhereditary myositis ossificans/myositis ossificans circumscript)
Benign,
self-limited,
heterotopic ossification within the muscle,
that usually appears after trauma.
It occurs predominantly within large muscles such as the thigh or shoulder.
The pattern of ossification can help differentiate from agressive lesions.
Imaging features:
- at 8 weeks: well-circumscribed lesion with peripheral rim calcification and lucent centre,
separated from the adjacent periosteum of the adjacent bone by a lucent zone;
- conversion to mature bone over time,
becoming smaller and denser.
- before 8 weeks: imaging can be indistinguishable from malignant lesions because peripheral calcification is not well seen.
- at 8 weeks: inhomogeneous mass with soft tissue and osseous oedema.
Peripheral curvilinear low signal corresponds to the mineralization.
C.4.
VASCULAR
C.4.1.
Popliteal Artery Aneurysm
Popliteal artery is the most common location of peripheral aneurysms,
accounting for 80% of the cases.
Definition: popliteal artery diameter >2cm
Imaging features (figure 7): fusiform or saccular arterial enlargement.
C.5.
NEURAL
C.5.1.
Peripheral Nerve Sheath Tumour
Benign tumour arising from nerve sheaths.
Histologically,
they are classified in neurofibromas and schwannomas.
Any peripheral nerve can be affected.
In the lower extremity,
the knee is the commonest site (PNST of the common peroneal nerve).
Imaging features: fusiform lesions oriented along the long axis of the involved nerve; atrophy of the muscles supplied by the involved nerve
-
MR (figure 8):
T2W images: central low signal intensity with peripheral high signal intensity (target sign) and a rind of fat surrounding PNSTs (split fat sign)
In the great majority of the cases,
it is possible to see the entering/exiting nerve,
usually with marked enhancement on post-contrast images.
Malignant transformation (MPNST) is usually seen associated with neurofibromatosis type 1 or induced by radiation.
Imaging features (figure 9): similar to PNSTs but are often larger (>5 cm),
infiltrative,
intralesional necrosis with heterogeneous enhancement.
C.6.
BONE
C.6.1.
Osteochondroma
Osteochondroma are the most frequent bone tumor and may be thought of as a developmental anomaly instead of a  benign bone tumour: they develop during childhood and remains for the rest of the individual’s life.
benign bone tumour: they develop during childhood and remains for the rest of the individual’s life.
Sporadic or associated with hereditary multiple exostoses (diaphyseal aclasis).
They are formed by cortical and medullary bone (which is continuous with the medullary cavity of the parent bone) surrounded by a hyaline cartilage cap.
The long bones of the lower extremities are affected in 50% of the cases,
mostly around the knee (distal femur>proximal tibia).
Malignant transformation is rare (~1%) and occurs in the cartilage cap,
with suspicious findings being a cap thickness >2cm.
Imaging features: usually pathognomonic
-
Plain radiographs: sessile or pedunculated metaphyseal lesion typically projecting away from the epiphysis; cartilage cap has a variable appearance.
-
US: demonstrates the cartilage cap as a hypoechoic region bounded by bone on its deep surface and muscle/fat superficially.
-
CT: can better demonstrated medullary continuity and the cartilage cap
-
MR: best imaging modality useful to assess the cartilage cap and adjacent structures.
- The cartilage cap of osteochondromas appears the same as cartilage elsewhere: intermediate to low signal on T1 and high signal on T2 weighted images.
- Peripheral enhancement of the cartilage cap can be seen post-contrast.
C.6.2.
Osteosarcoma (OS)
Malignant osteoid-forming tumours.
They represent the second most common primary bone tumour after multiple myeloma.
Primary osteosarcoma: typically in children and adolescents
Secondary osteosarcoma: occurs in the elderly; usually secondary to malignant degeneration of underlying bone lesion (e.g.:Paget disease,
extensive bone infarcts,
post-radiotherapy, osteochondroma,
osteoblastoma).
Many subtypes have been described (with varying different imaging findings) according to the degree of differentiation,
location within the bone,
and histological variants:
Conventional high-grade OS is the most common type and presents as a metadiaphysary lesion of tubular bones in the appendicular skeleton,
affecting the knee in ~60% of cases (distal femur>proximal tibia).
Imaging features:
-
Plain radiographs: medullary and cortical bone destruction;  permeative or moth-eaten appearance; wide zone of transition; aggressive periosteal reaction; variable amount of tumor matrix ossification.
permeative or moth-eaten appearance; wide zone of transition; aggressive periosteal reaction; variable amount of tumor matrix ossification.
-
CT: specially useful in predominantly lytic lesions with little amount of mineralized material.
-
MR: best imaging modality for local stating and surgical planning.
T1W images – low signal intensity of mineralized components; intermediate signal intensity of soft-tissue non-mineralised component and peritumoral oedema.
T2W images: low intensity of mineralized components; high signal intensity of soft-tissue non-mineralised component and peritumoral oedema.
After gadolium administration,
solid components enhance.