|
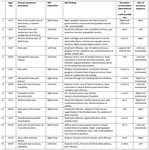
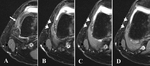
The review of the MRI examinations revealed an accessory plantaris muscle in 15 out of the 600 patients (2.5%) [fig.1-table].
Patients’ age ranged from 16 to 59 yrs (mean age=38yrs).
There were 9 female patients (1.5%) and 6 male patients (1%).
There was no statistically significant difference between the prevalence of the accessory plantaris muscle in males versus females.
In 3 patients MRI was performed on both knees.
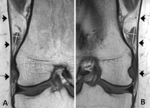
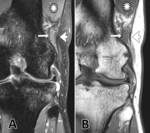
In one of them (case 1) the accessory plantaris muscle was found on both sides [fig.2-case1],
while in the other two (cases 3,13) an accessory plantaris muscle was disclosed only at one side.
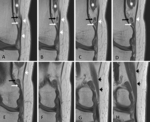
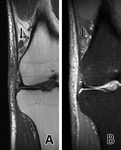
In one patient (case 4) the accessory plantaris had two parallel bellies (superior and inferior) [fig.3-case 4].
The review of the initial MRI reports disclosed that the accessory plantaris muscle was mentioned only in 7 out of the 15 patients.
All the accessory plantaris muscles originated from the iliotibial band,
below the lower end of the vastus lateralis muscle,
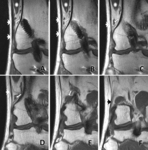
and coursed posteriorly to blend with the normal plantaris muscle [fig.4-case 9].
The laterolateral dimension on the coronal plane at the middle of the belly of the accessory plantaris muscle ranged between 2.5-6 mm (mean=4 mm) and the craniocaudal dimension at the same coronal level ranged between 4.5-14 mm (mean=10.5 mm) [fig.1-table,
fig.2-case 1].
The bellies had an ellipsoid shape on the coronal plane and a conical end at the iliotibial band [fig.5-case 10].
In case No 4 there was a variation of the accessory plantaris muscle.
This muscle had two parallel oriented bellies that they blended posteriorly with each other and with the native plantaris and anteriorly each belly inserted separately into the iliotibial band.
Both insertions were located below the lower end of vastus lateralis muscle [fig.3-case 4].
Symptoms included acute or chronic knee pain,
(cases 1-8,10,11,13,14,15),
and instability (case 8,9,15).
One patient (case 12) did not experience pain but she was examined for evaluation of known patellar chondromalacia.
Clinical evaluation indicated possible meniscal tear in 4 patients (cases 1,2,6,11),
ACL rupture in 3 patients (cases 5,8,15),
chondromalacia of patella in 2 patients (cases 10,12),
quadriceps femoris tendon tear in one patient (case 14),
osteonecrosis of medial femoral condyles in one patient (case 13),
and probable iliotibial band friction syndrome in one patient (case 11).
Special care should be taken in cases of ACL reconstruction,
as in case No 9,
if the surgical technique used includes an antegrade,
outside-in,
screw fixation of the proximal part of the graft at the lateral side of the lateral femoral condyle [3].
In case No 9 [fig.4] (evaluation of ACL reconstruction),
the accessory plantaris was found intact.
In cases of iliotibial band friction syndrome there is compression of the adipose tissue interposed between the iliotibial band and the lateral femoral condyle [4].
The presence of the accessory plantaris muscle could act as a predisposing factor,
as it restricts the volume of the adipose tissue.
In case No 11 [fig.7] (probable iliotibial band friction syndrome) the symptoms were due to soft tissue edema superficially the iliotibial band.
The commonest MR finding coexisting with the accessory plantaris muscle was joint effusion [fig.5,6].
Other MR findings included: ganglia at various locations either intraosseous or in soft tissues (cases 1-4,6,10,15),
torn medial meniscus (cases 2,4,5,9,10),
torn lateral meniscus [fig.4-case 9],
chondromalacia of the patella (cases 6,9,10,12),
osteochondral lesions (cases 3,5),
ACL rupture-bone contusions [fig.6-cases 5,8,15],
popliteal cyst (case 4),
myxoid degeneration of anterior cruciate ligament (case 3),
pes anserinus bursitis and prepatellar bursitis (case 2),
patella alta (case 4),
bone island (case 6),
nonossifying fibroma of fibula (case 7),
soft tissue oedema [fig.7-case 11],
Osgood-Schlatter disease (case 5),
bone marrow edema lesions (case 13),
tear of the distal end of the quadriceps tendon (case 14).
In 1 knee the findings were unremarkable (case 1).
|