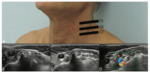
Exploration of the brachial plexus requires a high frequency probe,generally between 10 and 18MHz.
Based on topographic anatomy,
some anatomical regions can be identified when we want study the different components of the brachial plexus:
1. the paravertebral region;
It is important to have some landmarks that will help find the actual level of the roots:
- thyroid gland;
- the transverse process of C7;
- vertebral artery.
The probe is positioned in a horizontal plane at the level of the thyroid gland. Move the probe laterally and find the transverse processes of the cervical vertebrae; from this position drag the probe from the top downwards to see the different roots. C6 is “V” shaped,
C5 is like a “U” for the presence of two branches (anterior and posterior) and T1 doesn’t have a tubercle.
The transverse process of C7,
instead,
not only lacks an anterior tubercle but also,
in most cases,
the foramen for the vertebral artery.
2. the interscalene region;
Landmarks of the interscalene triangle:
- superficially: the junctional fibrous layer of the omohyoid muscle
- anteriorly and medially: the anterior scalene muscle
- posteriorly and laterally: the middle scalene muscle
- inferiorly: the subclavian artery
- the deep cervical arterythat arises from subclavian artery and generally passes between C7-C8 cervical nerves.
Using the anatomical landmarks previously described,
start with axial slices of the roots along the omohyoid muscle.
3. the supraclavear region;
Landmarks:
- subclavian artery
- transverse cervical artery
- first rib (hyperechoic cortex with a shadow cone)
- the apex of the lung(hyper-echoic pleura moving with breathing)
4. the retropectoral and infraclavicular/axillary regions.
Landmarks:
- axillary artery (continuation of the subclavian artery distal to the costoclavicular gap).
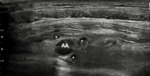
The cords are grouped posterior and lateral to the axillary artery,
forming a “phrygian cap” (Mercedes sign) (fig.
2.1.12):
- posteriorly and laterally: the posterior cord;
- superficially: the lateral cord;
- medially and deeply: the medial cord.
To study the cords under the axilla,
raise the arm of the patient and start from the proximal third of the arm, where the median,
ulnar and radial nervesare easy to find surrounding the brachial artery.
Then follow them back to the axilla using the elevator technique (distal to proximal,
short axis scan).