* Operation: Among the 163 patients
- Endoscopic decompression : 15 pts.
- Simple decompression : 23 pts.
- Interspinous locker device insertion(soft fixation) with/without decompression : 99 pts
- Interbody fusion surgery with/without decompression :17 pts.
- Percutaneous vertebroplasty : 7 pts.
* After reviewing the W-B MR,
- The treatment plans have been determined or modified : 78 pts.
(78/163=48%)
- Perform the surgery with confidence : 44 pts.
- Another additional surgery : 22 pts.
- Modified (n=2) or reduced (n=10) the extent of the operation : 12 pts.
Case 1.
M/51 (Fig.1 to Fig.
7)
C.C ( Chief Complaint): Post.
Neck pain
- remote onset : 5years
- recent onset : 3 weeks
Brief Hx.)
- Previous C4-5 (15MA),
C5-6 (3MA) Artificial disc replacement (ADR) surgery.
- Persistent neck pain,
upper thoracic,
left scapular area pain.
- Pain aggravated on neck flexion.
Pain Management, Facet injection,
MBB → transient effect

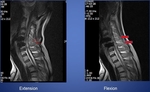
Fig. 1: Plain X-ray : ADR (Artifical disc replacement) state at C4-5, C5-6, remained instability.

Fig. 2: Dynamic MR with G-Scan: Widening of the C4-5, C5-6 interspinous spaces / instability.

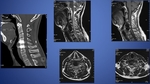
Fig. 3: Pre-op. CT and conventional MR : ADR state with metal artifact, degenerative change.

Fig. 4: Supine and W-B ( Weight-Bearing) MR with G-Scan :
Decreased metal artifact, Left C6-7 foraminal narrowing accentuation on W-B MR (long arrow).
Clinical courses:
- Previous C4-5,
C5-6 Artificial disc replacement.
- Neck pain,
both upper back pain persist.
- On dynamic study with G-Scan → C4-5,
C5-6 post.
Instability.
- C6-7 central,
left foraminal narrowing also accentuation.
- C4-5,
C5-6 post.
Fusion surgery was performed first.
- After the operation,
neck pain subsided but C6-7 instability accentuation on dynamic study,
and C6-7 left side foraminal lesion remained.
- Conservative treatment,
and additional C6-7 post.
Fusion surgery was done.

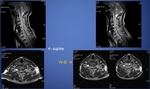
Fig. 5: After C4-5, C5-6 post. Fusion surgery.

Fig. 6: Post-op. MR, decreased metal artifact in G-Scan images, compare to conventional image.

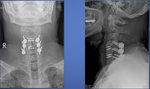
Fig. 7: C4-5, C5-6 fusion surgery and additional C6-7 post. Fusion.
Clinical relevance:
- W-B images as well as Dynamic images with G-Scan on C-spine.
- Instability after the ADR ( artificial disc replacement ) in C4-5,
C5-6.
- C6-7 pathology also detected (→ occult pathology).
- After the additional C6-7 post.
Fusion surgery,
instability was improved.
** Decision of the operation,
operation level.
Case 2.
F/48 (Fig.8 to Fig.
13)
C.C ) Post.
Neck pain,
Gait disturbance,
left leg weakness
- Onset : remote - 10 mos.
recent - few days.
On the neck flexion,
neck,
back pain,
numbness,
both upper arm pain(Lt>Rt), both 4,5th finger tingling sensation was aggravated..
Brief Hx.) Traumatic injury ,
20 Yrs.
Ago
Developed post neck pain,
both arm/leg numbness,
aggravated on neck flexion.

Fig. 8: Plain X-ray, C1-2 instability.

Fig. 9: Conventional MRI, C1-2 cord compression with compressive myelopathy.

Fig. 10: Conventional MR with Dynamic images, C1-2 compression was aggravated on flexion.

Fig. 11: G-Scan, supine vs W-B MR, C1-2 compression was accentuated on W-B.
Clinical courses:
- C1-2 instability ,
Progressive myelopathy,
Cord atrophy with signal change
- S/P C1-2 Post.
Fusion
- After fusion,
symptom relieved

Fig. 12: After C1-2 fusion surgery, C1-2 cord was decompressed.

Fig. 13: C1-2 cord was decompressed, G-Scan images.
Clinical relevance:
- C1-2 instability case.
- W-B MR: Pre-operative instability was aggravated on W-B position as well as dynamic ( flexion & extension) images.
- Pre-op.
and Post-op.
evaluation of the instability with the W-B study.
** Decision of the operation method.
Case 3. M/40 (Fig 14 , Fig.
15)
C.C: Localized Left Back and flank pain
onset : 1 month.
Brief Hx.
: Symptoms aggravated on standing and driving a car.

Fig. 14: Conventional CT, MR: mild disc bulging , at T8-9.

Fig. 15: W-B MR : Aggravated the Disc protrusion at T8-9 with cord indenation/compression.
Clinical courses :
- T8-9 level disc protrusion with cord compression on W-B MR.
- Confirmed by selective nerve root block,
left T9 → symptoms were improved about 70%.
- PETD(Percutaneous Endoscopic Thoracic Discectomy) was done → symptoms were relieved.
Clinical relevance :
- Protrusion with mild cord compression in thoracic level can develop symptoms in dynamic position.
- It is difficult to explain with conventional imaging study in supine position (mild bulging).
- W-B MR : Clearly visualized the correlative pathology as the dynamic study.
- Diagnosis,
and perform optimal treatment!
** Decision of the operation,
occult disc herniation.
Case 4.
M/61 (Fig.
16 to Fig.
20)
C.C: Back and bilateral leg radiating pain
Onset : more than one and a half years
Brief Hx.) Conservative Tx.
Frequently → no improvement.
Gradually aggravated symptoms.
Difficulty in walking for more than 5 minutes.

Fig. 16: Plain radiography: anterolisthesis, L4 on L5, mild L4-5 disc space narrowing.

Fig. 17: Conventional MRI and F/U : mild stenosis, L4-5, facet OA (osteoarthropathy).

Fig. 18: G-Scan, supine/standing comparison: Decreased disc height, aggravated anterolilsthesis, L4 on L5, increased post. protrusion , lig. Flav. Thickening on standing image → aggravated L4-5 stenosis.

Fig. 19: G-Scan, axial images supine/W-B comparison: L4-5 stenosis was aggravated.
Clinical courses :
- S/P L4-5 laminectomy with ILF(Interspinous locker fixation)
- After the operation,
symptoms were relieved.
- Follow up study : maintain the neural foraminal dimension as well as central decompression and stable status.

Fig. 20: Post-op. (L4-5 laminectomy with ILF, interspinous locker fixation) images showed well decompressed L4-5 stenosis.
Clinical relevance;
- Patient had been suffering from long-term pain due to instability
- Mild to moderate stenosis on supine MRI → Aggravated to severe stenosis on W-B MRI.
- Dynamic stenosis as well as the Post.
Elements pathologies (Facet OA,
perifacetal soft tissue edema,
lig.
flavum thickening) might be the source of the back and radiating pain.
- Resolved after decompression with ILF (soft fixation)
- Optimal Minimal Invasive Spine Surgery (MISS) after accurate diagnosis,
correlated with symptoms!
** Decision of the operation.
Case 5.
F/58 ( Fig.
21 to Fig.
23)
C.C: Back,
right leg pain
Remote onset: 3 years
Recent onset: 2-3 months.
Brief Hx.) Symptoms aggravated on sitting,
standing,
walking.
Initial op.
plan: L3-4 laminectomy with ILF(Interspinous locker fixation)

Fig. 20: Post-op. (L4-5 laminectomy with ILF, interspinous locker fixation) images showed well decompressed L4-5 stenosis.

Fig. 22: Supine conventional MRI, CT, Myelogram: L3-4 stenosis and L4-5 mild protruded disc.

Fig. 23: G-Scan, supine/W-B comparison: Increased volume of the Rt. L4-5 disc herniation with L5 root swelling (long green arrows).
Clinical courses:
- Op.: L3-4 laminectomy with ILF and L4-5 open discectomy(additional)
- Op.
findings : Right L4-5 disc protrusion with gummy/bouncy texture (more protrusion on pressure on operation field).
- After the surgery,
symptoms were improved.
Clinical relevance :
- Back pain – by the L3-4 pathology.
- Right leg pain: Caused by right L4-5 disc herniation and distal L5 root swelling (found out on W-B MR clearly).
- Added the L4-5 open discectomy to the initial op.
plan.
- W-B MRI can prevent failed back surgery.
- Gummy/Bouncy/Sticky texture of the herniated disc,
could be revealed on W-B MR (as increased pressure on the disc).
** Occult disc,
added operation.
Case 6.
F/71 (Fig.
24 to Fig.
27)
C.C : Back pain,
severe left buttock and leg pain
Brief Hx: symptoms onset – 6 mos.
- Conservative treatments : ineffective

Fig. 24: Plain X-ray : Diffuse spondylosis, L-spine.

Fig. 25: Supine MR, CT: bulging left L5-S1 foraminal zone.

Fig. 26: G-Scan, supine/W-B comparison: increased volume of the herniated disc.
Clinical courses:
- Severe left leg pain.
- On W-B MR,
left L5-S1 foraminal disc protrusion with stenosis was revealed.
- Temporary effect after left L5 root block
- Operation ( PELD,
Percutaneous Endoscopic Lumber Discectomy) was done – there was large protruded disc
- After the operation,
symptoms were relieved.

Fig. 27: PELD (Percutaneous Endoscopic Lumbar Discectomy), left L5-S1 foraminal :Nerve root(red arrows) was decompressed ( Herniated disc on op.field- arrowhead).
Clinical relevance:
- Case of the Foraminal disc herniation with stenosis → severe leg pain.
- Bulging contour with patent epidural fatty tissue around the root on supine images.
- Disc protrusion was clearly demonstrated on W-B → removed the disc material.
- The Clinical relevant pathology could be verified by the W-B MR and root block.
** Decision of the operation,
occult disc.
Case 7.
F/76 (Fig.
28 to Fig.
30)
C.C: Back pain,
both(L>R) L/E pain,
walking difficulty
- remote : several years
- recent : 3-4 mos.
Brief Hx.: L5 spondylolysis,
Conservative Tx.
: temporary effective ( but symptom progressed)

Fig. 28: X-ray, CT: L5-S1 lytic listhesis, left L5 pedicle fracture.

Fig. 29: CT, conventional MR: moderate L3-4, severe L4-5 stenosis, bilateral L5-S1 foraminal stenosis, left L5 pedicle fracture.

Fig. 30: On the G-Scan, supine and W-B images, L3-4 stenosis was slightly aggravated, and L4-5 stenosis was aggravated.
Clinical courses;
- Initial op.
plan : L5-S1 interbody fusion and L3-4,
L4-5 decompression.
- With minimal change of L3-4 lesion on W-B MR → We decided to decrease the level of the operation ( L5-S1 interbody fusion and L4-5 decompression).
- Symptom improved after the surgery.
Clinical relevance:
- Long standing pain & definite L5-S1 lesion.
- Even though,
L3-4,
L4-5 stenosis,
there was mild accentuation of L3-4 lesion on W-B study ( L4-5,
L5-S1 pathology were aggravation,
on the other hand).
- After reviewing the W-B study,
we could exclude the management of the L3-4 pathology.
- Operation level was diminished with the evidence of the inconsequential pathology ( not related with patient’s symptom) by virtue of the W-B study.
** Reduce the operation level.
Case 8.
M/67 ( Fig.
31 to Fig.
33)
C.C) Back,
both buttock pain,
bilateral leg pain.
Onset : 2Mos.
Brief Hx.
:
Conservative Tx.
: Improved leg pain,
temporary
Lumbaization of S1,
Compression fracture,
L1 to L4

Fig. 31: X-ray : scoliosis, anterolisthesis of L4 on L5, L5 on L6 ( lumbarization of S1).

Fig. 32: Conventional (1.5 T) MR & MR myelogram: mild L4-5 stenosis and moderate to severe L5-6 stenosis.

Fig. 33: G-Scan : On standing MR, L4-5 stenosis was remained mild degree.
On the other hand, L5-6 stenosis was aggravated compare to supine MR.
Clinical course ;
- Because of the dermatomal pattern,
we considered the decompression surgery at L4-5 and L5-6 with L5-6 laminectomy with ILF at first.
- However,
after reviewing the images include W-B images,
we decided the laminectomy with ILF at the L5-6 level.
- After the operation,
main symptoms were improved.
- Few months later,
we performed PVP at the L1 and L2 fracture site.
Clinical relevance;
- The patient have other coincidental pathologies ( L1 to L4 fracture).
- Therefore,
the first surgery should be minimized.
(other lesions must be warned !)
- Main symptoms (leg and buttock pain) were improved after the primary surgery ( L5-6 decompression with ILF).
** Reduce the operation level.