Soft tissue sarcomas (STS) are rare,
heterogeneous lesions derived from the embryonic mesoderm,
accounting for approximately 1% of adult cancers.
Suit et al.
suggested that their low incidence perhaps accounted for an apparent delay in detailed knowledge of their natural history (1). Dangoor et al.,
indirectly corroborated this statement,
noting that the rarity,
heterogeneity and diffuse location of these lesions had created challenges in establishing concrete evidenced-based guidelines (2).
Patients can present with solitary lesions or de novo metastatic disease,
with metastatic disease at first presentation having a worse prognosis.
59-75% occur in the extremities,
abdomen (retroperitoneal),
or head and neck,
presenting primarily with insidious,
painless,
soft tissue masses.
Size and recent growth are considered important clinical features suggestive of malignancy.
Soft tissue lesions over 5cm have a 20 % risk of malignancy (3). Patients presenting with a mass greater than 5 cm in size,
deep to the fascia,
which are fixed,
immobile,
painful and increasing in size should be urgently referred to a specialist centre according to the most recent NICE guidelines (2-4).
Bauer et al.
conducted a study describing the anatomical location of 1851 primary tumours,
noting that 35% occurred subcutaneously,
32% were intramuscular and 32% deep,
extramuscular. 75% were categorised as high grade (III/IV) and the median size was 7cm (1-35cm).
Metastatic disease relating to these lesions was not discussed(5).
The American Joint Committee on Cancer (AJCC) noted the prognostic significance of the anatomic tumour location and its relation to the surrounding fascia of an extremity or trunk in 1998.
Additionally,
NICE and ESSR,
all consider pre-treatment radiology critical for defining local tumour spread,
staging,
biopsy guidance and diagnosis.
Furthermore,
staging incorporates tumour size,
histological grading,
depth and whether there is distant or nodal metastatic disease (1-3).
Local control has improved secondary to good wide local excisions and neo-adjuvant therapies whilst local recurrence and its management is well established in the literature (3,6).
Metastatic disease however still remains a significant onus occurring in up to 40% of patients.
Distant metastases are more often related to higher grade and larger tumours,
with haematogenous disease contributing to the most common cause of death in STS disease (7).
Most commonly metastases are seen in the lung accounting for up to 80% of cases and osseous metastases occur in 10%.
Metastatic disease has been described in alveolar,
angiosarcoma,
leiomyosarcoma,
undifferentiated pleomorphic and dedifferentiated liposarcoma.
Up to 80% of those osseous metastases are lytic and fluorodeoxyglucose (FDG)-PET positive (4,8,9,10).
Lymph node involvement is more rare (3%) occurring with rhabdomyosarcoma,
clear cell,
epithelioid,
angiosarcoma and synovial sarcomas (11).
In summary,
histological grade (most important),
tumour depth,
size,
resection margin,
patient age,
previous radiotherapy and histology are all critical prognostic indicators.
However,
at the time of this submission,
there is no comprehensive description in the literature assessing the relationship between the primary STS depth and the pattern of metastatic disease.
We evaluated the location of the primary STS (superficial or deep to fascial planes) and the presence and location of metastatic disease at presentation.
For the purposes of this submission,
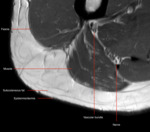
fascia relates to the aponeurotic tissue engulfing a muscle.
Superficial therefore describes a lesion superficial to fascia,
whilst deep is beneath the fascia.
Superficial and deep is in reference to infiltration both above and below this aponeurosis (Figure 1).