Keywords:
Neoplasia, Metastases, Cancer, Vertebroplasty, Ablation procedures, MR, Fluoroscopy, CT, Neuroradiology spine, Musculoskeletal spine, Interventional non-vascular
Authors:
D. Notaro, M. Bellini, M. A. Mazzei, L. Volterrani, L. Monti, A. Cerase, P. Galluzzi; Siena/IT
DOI:
10.1594/essr2018/P-0079
Methods and Materials
This retrospective study included 12 lumbar and 4 thoracic vertebrae treated in 14 patients (10 M,
4 F; mean age,
60 years; range,
23-79) suffering from symptomatic vertebral bone metastases or multiple myeloma.
The primary cancer locations were: Breast n.3; Lung n.5; Multiple Myeloma n.3; Kidney n.2; Colon n.1. In 2 patients,
the procedure was performed at 2 levels at the same time.
Inclusion criteria were 1) painful vertebral lytic lesion with high risk of collapse or pathologic fracture seen at MRI or CT 2) persistent pain after pharmacologic or radiotherapic treatment,
and 3) no or moderate intracanalar tumor.
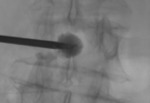
RFA (Boston RF3000 Generator,
Boston Scientific Way Marlborough,
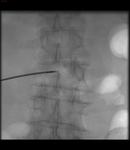
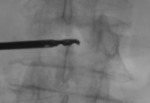
USA) was performed by monopeduncular approach,
under biplanar fluoroscopic guidance and local anesthesia,
applying single needle or umbrella shaped array electrode in two different part of the bone lesion,
depending on dimensions.
Power was increased by applying 1 Watt every minute and treatment was finished when impedence rised 200 ohms.
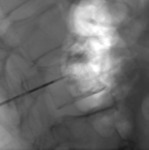
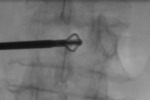
Vesselplasty system (Vessel,
Dragon Crown Medical Co.
Shandong,
China) has then implanted into vertebral body lesions,
and expanded by injection of a biological or a PMMA high viscosity cement (CaSO4 Osteo-G®,
Spirit Spine,
Taiwan; VertaPlex HV Bone Cement,
Stryker,
USA).
All the patients underwent thoraco-lumbar spine gadolinium-enhanced MRI before and 1 month after the treatment.
A VAS scale was taken before,
1 week,
1 month,
and 6 months after treatment.