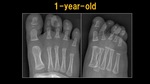
From pediatric to adult age,
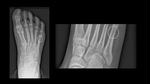
we can see the normal growth of the 5th metatarsal bone (fig.2-fig.10).
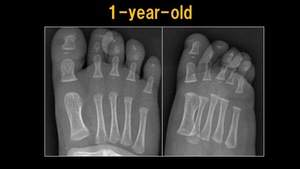
Fig. 2: X-ray: 1 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
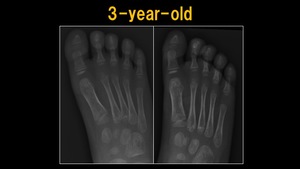
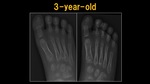
Fig. 3: X-ray: 3 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
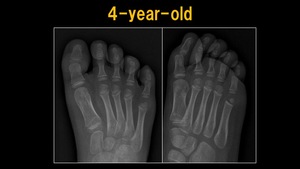
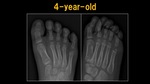
Fig. 4: X-ray: 4 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
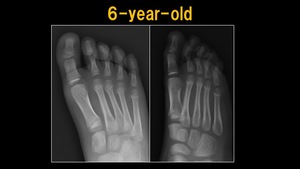
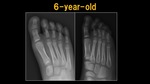
Fig. 5: X-ray: 6 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
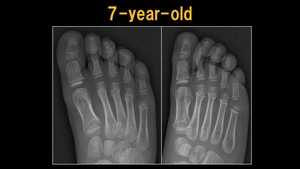
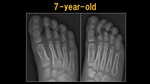
Fig. 6: X-ray: 7 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
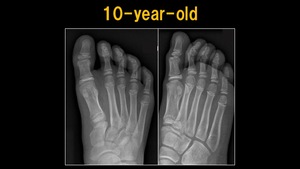
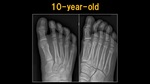
Fig. 7: X-ray: 10 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
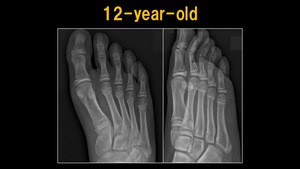
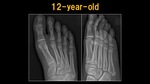
Fig. 8: X-ray: 12 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
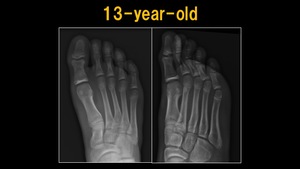
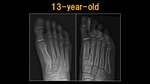
Fig. 9: X-ray: 13 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
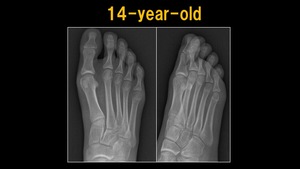
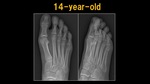
Fig. 10: X-ray: 14 y.o. child
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
Many pathologies can involve it:
ISELIN DISEASE
Iselin disease is a benign condition,
defined as apophysitis of the 5th metatarsal bone.
It was firstly described by H.
Iselin,
in 1912.
Iselin disease is seen in adolescent (8-13 years old) and it is also seen in males with sport injuries related to a repetitive traction of the peroneus brevis tendon at its insertion.
Symptoms are pain in lateral foot and physical examination can demonstrate swelling and erythema with tenderness over base of the 5th metatarsal bone.
(fig.11).
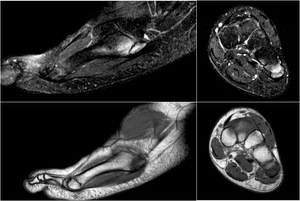
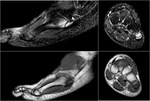
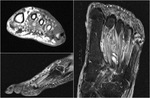
Fig. 11: MRI: Iselin Disease
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
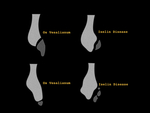
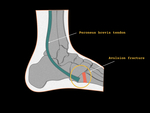
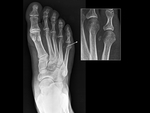
Differential diagnosis includes the fracture of the base of the 5th metarsal and os Vesalianum (fig.12).
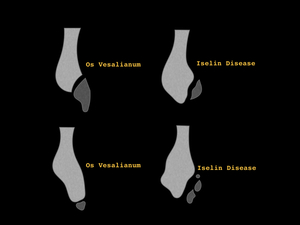
Fig. 12: Differential diagnosis between Iselin Disease and Os Vesalianum
Os vesalianum is an intratendinous accessory bone that can be associated with pain. It is formed as a result of failed fusion of the secondary ossification center of the metatarsal.
It is situated at the base of the 5th metatarsal in the peroneus brevis tendon.
FRACTURES
5th metatarsal bone fractures are frequently injuries of the foot,
accounting of 68% of metatarsal fractures.
Typically,
there are three anatomical location of 5th metatarsal fracture.
They are the proximal tubercle,
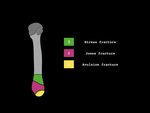
the proximal meta-diaphysis and the diaphysis (Dameron-Lawrence-Bofte classification- fig.13-14).
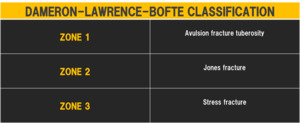
Fig. 13: Dameron-Lawrence-Bofte classification
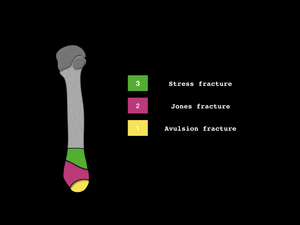
Fig. 14: Drawing of Dameron-Lawrence-Bofte classification
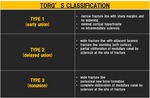
Torg's classification of the proximal 5th metatarsal fracture is based on the degree of sclerosis adjacent to the fracture (fig.15).
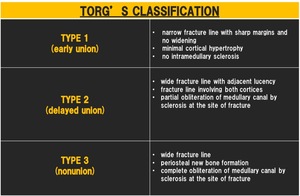
Fig. 15: Torg's classification
1.
Tuberosity avulsion fracture (Dancer’s fracture)
This fracture involves the proximal tubercle of the bone.
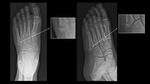
The typical mechanism of fracture is related to inversion-stress forces on the peroneus brevis tendon that cause avulsion of the base of the bone. (fig.16-17).
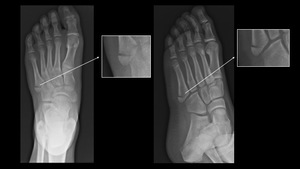
Fig. 16: X-ray: Zone 1 fracture
References: Ospedale IRCCS Giannina Gaslini, Genoa, Italy
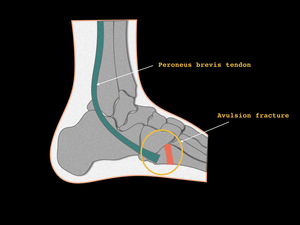
Fig. 17: Drawing of avulsion fracture
2.
Jones fracture
This fracture occurs at the methaphyseal - diaphyseal junction and involves the 4th-5th metatarsal articulation.
The mechanism of fracture is a medio- lateral force applied while heel is raised and foot is plantar flexed (fig.18).
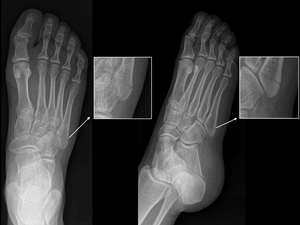
Fig. 18: X ray: Zone 2 fracture
3.
Diaphyseal fracture
It is typically a stress fracture.
The mechanism may by a chronic microtrauma (fig.19).
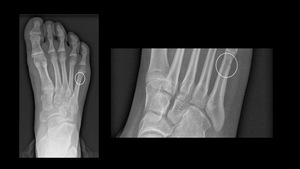
Fig. 19: X-ray: zone 3 fracture
TENDONS PATHOLOGY
The peroneus brevis (PB) muscle arise from the posterolateral surface of the fibula.
Its tendon shares a common synovial sheath with peroneus longus (PL) tendon,
passing posterior to the fibular malleolus,
inside the retro-malleolar groove. Usually,
the PB tendon is anteromedial to the PL.
On the lateral aspect of calcaneus, it runs superficial to the calcaneofibular ligament (CFL),
then superior to the peroneal trochlea and inserts on the base of the 5thmetatarsal bone
This tendon is a plantar flexor of the ankle and everter of the subtalar and mid-tarsal joints. Within the distal part of the tendon,
may be located the os vesalianum,
an inconstant accessories ossicle.
PB resides in a vulnerable position,
between the retro-malleolar groove and the PL tendon: at this level,
inflammatory processes (tenosynovitis) and tendon tears may occur. In some cases, the PL tendon can migrate forward into the peroneus brevis, causing a split lesion.
Peroneal tendon tears may be associated with other pathologic condition of the lateral ankle complex: bone fractures,
ligament injuries and retinaculum disruptions.
The pathological involvement of the distal part and insertion of PB tendon is rare. Peroneal tendons pathologies are best evaluated with US and MRI.
OSTEOMYELITIS
The definition of osteomyelitis implies an infection of the bone marrow.
osteomyelitis can develop through three mechanisms: hematogenous spread of infection,
spread from a contiguous source of infection,
direct implant of infection.
Often,
the exact mechanism of infection may not be clear and more than one potential mechanism may be involved.
Hematogenous spread of infection to the bone results first in osteomyelitis than can be followed by infective osteitis,
infective periostitis and soft tissue infection,
in that order.
Infection can extend from one tissue to an adjacent one,
and normally the bone is contaminated from nearby soft tissues. In these cases,
the sequential stages of the process are in the following order: infective periostitis,
invective osteitis,
and osteomyelitis. A classic example of this mechanism is the infections that occur in the foot of diabetic patients.
Direct implant of infection it is the result of puncture wounds,
foreign bodies,
exposed fractures or surgeries.
Based on the patient's clinic and the radiological characteristics we can divide the osteomyelitis into three stages: acute,
subacute and chronic.
Osteomyelitis must compromise 30 to 50% of bone mineral content to define noticeable changes in plain radiographs. Plain radiographs may show regional osteopenia,
periosteal reaction, endosteal scalloping and loss of bony trabecular architecture.
MRI is the most specific and sensitive imaging modality to identify osteomyelitis. On T1-weighted images the bone presents intermediate to low signal than normal due to fluid and marrow edema and can present cortical bone destruction.
On T2-weighted images the bone present high signal.
After contrast administration,
images show post-contrast enhancement of bone marrow,
abscess margins,
periosteum and adjacent soft tissue collections.
One of the most common causes of osteomyelitis,
in the adult,
of the 5th metatarsal is the diabetic foot (fig.20).
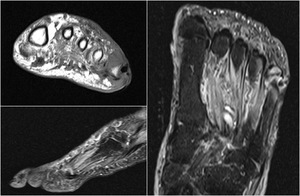
Fig. 20: MRI-diabetic foot: osteomyelitis of the 5th metatarsal bone
It is helpful to mark the skin or subcutaneous lesion (like ulcer or sinus tract) and to find its relation to the alteration of the bone.
Often,
in these cases,
amputation is required to control the infection.
RHEUMATOID DISEASES
The foot is the second most involved part of the body in rheumatoid disease after the hand,
and the forefoot is described as the most common site for symptoms.
The 5th metatarsal-phalangeal joint is frequently the first and the most involved anatomic site of the foot. The pathogenetic reason resides in the high-pressure values to whom it is subdued and lead to chronic micro-traumas, also other chronic mechanical damages,
such conflict with the shoe,
have been hypothesized as a complementary cause in the pathogenesis.
Rheumatoid arthritis (RA) is the commonest type of inflammatory arthritis.
Up to 90% of people with this condition will report associated foot problems.
The 5th metatarsal-phalangeal joint frequently is the first joint to give radiographic evidence of destructive disease.
Plain X-ray is the gold standard techniques for the study of erosions; MRI has not demonstrated a superior power to identify erosions but it can easily reveal early synovitis and bone edema which can been described as a frequent precursor to erosions.
Psoriatic Arthritis (PsA) can usually be distinguished by RA by involvement of specific joints and the absence of rheumatoid factor in the blood.
It is more common for this type of arthritis to be asymmetrical and to involve the synovial bursae. The first metatarso-phalangeal joint is traditionally known as the most common site,
however the inflammatory involvement of the bursa located between the insertion of the tendon of abductor digiti minimi and the head of the 5th metatarsal bone has often been described. This peculiar bursa is contiguous to the 5th metatarsal-phalangeal joint,
which can explain the development of marginal bone erosions on the head of the 5th metatarsal as a purely extra-articular event also in the absence of concurrent joint synovitis. In PsA ultrasound examination can be usefully used as a first approach technique,
which can easily detect distension of the bursa,
and inflammation through Doppler Imaging.
SESAMOIDITIS
Sesamoids are osseous,
well corticated,
ovoid or nodular structure, partially or totally embedded in a tendon.
They protect the tendons from injury by reducing friction and are located near a bone or joint.
In contrast,
accessory ossicles are supernumerary bones that commonly derive from unfused primary or secondary ossification centres with no definite known function.
The sesamoids of the foot are: the hallucal sesamoids,
lesser metatarsal sesamoids and interphalangeal joint sesamoid of the great toe.
Anatomically, lesser metatarsal sesamoids are located in the plantar aspect of the joint capsule and may also be multiple or multipartite.
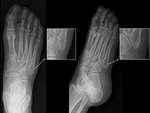
The prevalence of sesamoids at the 5th metatarsal is around 4.3 %. They are best visualized on antero-posterior and oblique radiographs of the foot (fig.21).
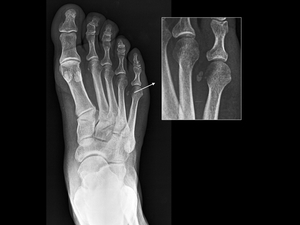
Fig. 21: X-ray: sesamoids of the 5th metatarsal bone
Pathology associated with these sesamoids is very rare.
Infections of adjacent soft tissue that spread deeply to the bone plane may cause sesamoiditis: sesamoids show bone marrow edema,
best evaluated on MRI.
The most important complication in the osteonecrosis,
with a progressive bone collapse.
Regarding accessories ossicles,
Os Vesalianum is located near the base of the fifth metatarsal,
within the peroneus brevis tendon and may articulate with the cuboid. Its reported prevalence is between 0.1 and 1%, best seen on an oblique radiograph of the foot.
The Os Vesalianum can be associated with pain but it is rarely a source of pathology and it must not be misinterpreted like a fracture of the base of the fifth metatarsal.