Epidemiology
KD mainly affects young adults,
but there are also cases in adolescents and in the elderly.
Men are affected as twice as women.
The disease is rarely bilateral.
Anatomy
The lunate bone is the central bone of the proximal carpal row.
It has two faces without cartilaginous covering,
the palmar and dorsal face through which nutritious vessels penetrate and four articular surfaces:
the proximal articular surface for the distal articular surface of the radius and the triangular fibrocartilage complex,
the medial surface for the triquetrum,
the lateral surface for the scaphoid,
the distal surface for the capitate.
In some cases a small distinct articular surface for the hamate is present between the articular surfaces for the capitate and for the triquetrum (type II lunate morphology according to the Viegas classification).
Pathophysiology
The etiology of KD is still unclear,
but is likely to be multifactorial.
The morphological variability of the lunate was evaluated as a risk factor for the disease onset and severity,
with discordant results.
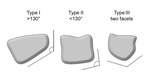
According to the Antuña Zapico classification [1],
the angulation of the proximal and lateral articular surfaces identifies three types of bone,
with the type I most at risk for the progression of KD,
due to a lower capacity of the bone trabeculae to oppose the loading forces (Fig.1).
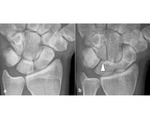
Viegas described the anatomic variability of the distal articular surface of the lunate [2] which may have a distinct medial facet for the hamate and a lateral one for the capitate (type II) instead of a single facet for the capitate (type I) (Fig.2). It has been observed that type II is protective against coronal fractures in KD [3].
Ulnar variance was investigated as a risk factor,
hypothesizing that the negative ulnar variance predisposed the lunate to greater load stress,
but cases of KD were observed even in the presence of null or positive ulnar variance [4].
The lunate is vascularized by branches coming from palmar and dorsal radiocarpal and intercarpal arches,
respectively.
These vessels penetrate the volar and dorsal surfaces through the insertions of the ligaments.
The palmar arteries are more numerous than the dorsal ones and provide a greater blood supply; the dorsal vessels are smaller and may even be missing [5].
The anastomoses between these vessels within the bone are variable and their absence,
as well as the lack of dorsal vessels,
may represent a risk factor for the development of KD [6].
Other factors have been studied as repeated microtraumatisms on the wrist by manual or sports activities,
increased intra-osseous pressure due to venous network congestion [7],
coexistence with autoimmune diseases [8] and cerebral palsy [9].
None of these seems to be related to the onset of the disease,
but rather to the severity of the symptoms.
It is possible that the disease arises on an anatomical predisposition and is the manifestation of a biological phenomenon of infarction and failure to repair the necrotic bone [10].
Clinical onset
KD begins with wrist dorsal pain and stiffness,
which worsens with repeated movements,
especially extension.
Patients report swelling and tenderness due to reactive synovitis around the lunate,
difficulty in wrist movements and reduced grip strength.
If left untreated,
KD evolves into clinical signs of degenerative arthritis such as crepitus and reduced range of motion.