Imaging findings
Kienböck's disease can be classified at imaging both morphologically and functionally,
in order to evaluate the most appropriate therapeutic choices.
The morphological classification proposed by Lichtman et al.
in 1997 and revised in 2010 [11] uses bone density in radiography and CT attenuation to evaluate the deformation and sclerosis of the lunate.
MRI evaluates changes in the ischemic bone marrow in T1 and T2-weighted images (Table 1).
In the early stages of KD,
due to insufficient blood supply,
the lunate is affected by bone marrow edema and progressive sclerosis,
but maintaining its morphology.
In the advanced stages,
the bone is no longer able to withstand load forces until fragmentation and reduction in height.
The adjacent inflammatory reaction occurs with synovitis and intra-articular effusion.
Morphologic classification
Stage I
- Bone marrow edema due to ischemic damage without morphological changes
- Normal density of the lunate in radiography and attenuation at CT scan
- Low signal intensity on T1-weighted images and usually hyperintense on T2-weighted fat-suppressed images.
Stage II
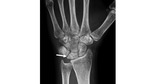
- Sclerosis of the lunate bone due to chronic ischemic damage (Fig.
3)
- Increased density in radiography with preserved morphology
- CT is more accurate in determine subtle fractures lines and pseudo-cystic inclusions
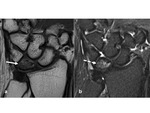
- Low signal intensity on T1-weighted and variable signal intensity on T2-weighted images (Fig.
4).
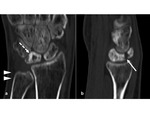
Stage III
- Sclerosis and collapse of the lunate
- No signs of degenerative arthritis changes in the other wrist bones
- Increased density in radiography and collapse of the lunate
- CT reveals fractures,
deformity and widening on the sagittale plane
- Low signal intensity on T1-weighted images and variable signal intensity on T2-weighted images.
Three subgroups
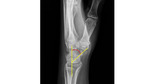
- Stage IIIa - no carpal instability (radio-scaphoid angle <60°) (Fig.
5 and 6)
- Stage IIIb - carpal instability (radio-scaphoid angle >60°)
- Stage IIIc - chronic coronal fractures of the lunate (Fig.
7)
Stage IV
- Collapse of the lunate
- Carpal instability
- Radiocarpal and midcarpal degenerative arthritis
- Functional impairment
- High density in radiography and high CT attenuation
- Low signal intensity on T1 and T2-weighted images due to sclerosis and necrosis.
Functional classification
The functional classification proposed by Schmitt et al.
[12] is based on contrast-enhanced MR images and allows to evaluate the residual perfusion and the viable portions of the lunate.
This information is integrated to the morphological one in order to choose the appropriate therapeutic option and during follow-up,
in particular for revascularisation.
Three contrast enhancement MR patterns are described:
- ceMR pattern A: there is a homogeneous contrast enhancement in T1-weighted images in all portions of the bone.
The signal is high in T2-weighted fat-sat images and low in unenhanced T1-weighted images,
compatible with bone marrow edema with preserved perfusion.
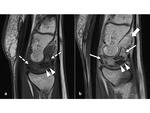
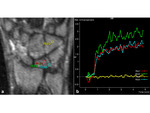
- ceMR pattern B: Contrast-enhancement is inhomogeneous,
patchy.
Non viable bone portions have no contrast enhancement and are located more often on the proximal surface of the bone.
Osteonecrosis is partial and shows low signal in both unenhanced T1-weighted images and T2-weighted fat-sat images (Fig.
6).
- ceMR pattern C: There is no contrast enhancement.
Osteonecrosis is extensive and shows predominantly low signal in all sequences.
Treatment options
In KD therapeutic options are multiple in relation to the stage of disease and anatomical variability.
There is no agreement on which is the most effective.
Stage I
Treatment is conservative with immobilization of the wrist.
Stage II
The goal is to prevent the collapse of the lunate and promote healing by restoring normal vascularization.
Several techniques have been proposed to unload the central column of the carpus (capitate and lunate) such as radial wedge osteotomy in case of negative ulnar variance or capitate-shortening osteotomy.
StageIIIa-b
Revascularisation with vascularized bone graft (VBG) consists in transposing a vascular pedicle with a bone fragment,
inside the necrotic portions of the lunate to promote angiogenesis (Fig.
8) [13,
14].
These options are used in stage IIIa,
where there is not carpal instability,
lunate cartilage is intact and the bone is viable.
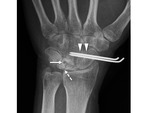
In stage IIIb carpal instability and flexion of the scaphoid must be corrected.
Revascularization interventions are associated with scapho-capitate (SC) or scapho-trapezio-trapezoid (STT) arthrodesis (pinning) (Fig.
9).
The aim of the SC and STT arthrodesis is to correct instability and to reduce the compression of the other carpal bones on the lunate [15].
This intervention promotes the healing of the lunate in advanced stages and reduces symptoms.
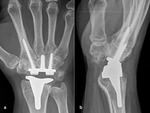
Stage IIIc and IV
Damage is advanced and there is no possibility of recovering the necrotic bone.
Options are proximal row carpectomy and wrist arthroplasty (Fig.
10) [16].