No matter which underlying mechanism results in an entrapment syndrome,
the reaction of a nerve to external compression has common features.
Ischemia due to compression results in fascicular edema.
The progression to a more chronic state results in fibrotic changes of the nerve sheath.
Sonographic signs reflect these pathophysiological reactions with altered echotexture and shape changes of the nerve.
Sonographic signs are an abrupt change in diameter; loss of the normal fascicular pattern of the nerve; swelling or coalescence of fascicles; hypertrophy of the outer epineurium; intraneural echogenic fibrotic spots in entrapments of longer durations; hypervascularity assessed as flow signals by color or power Doppler; atrophy of innervated muscles in longstanding disease assessed as a loss in bulk and increased reflectivity.
MEDIAN NERVE
ELBOW AND FOREARM
Median nerve entrapment at the elbow presents in two different ways: the pronator syndrome and the anterior interosseous nerve syndrome (Kiloh-Nevin syndrome).
Pronator Syndrome
CLINICAL ASPECTS: Pain and paresthesia in the volar aspect of the elbow,
forearm and in the hand affecting the first,
second and third digit as well as the radial half of the ring finger.
10-12
ULTRASOUND: The median nerve can be entrapped at four locations around the elbow:
-
Level of distal humerus by the ligament of Struthers: a rare anatomical variant associated with the presence of a supracondylar bony process at the distal humeral diaphysis.
The ligament extends from the supracondylar process to the medial humeral epicondyle.
The process and ligament can be easily identified in US.
-
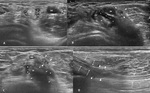
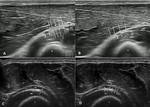
Level of proximal elbow by a thickened biceps brachii aponeurosis due to trauma or overuse of the biceps or due to a bicipito-radial bursitis (Fig. 1); after intravenous (i.v.) or brachial artery injection with formation of hematoma.
-
Level of elbow joint between the two heads of the pronator teres muscle (superficial and deep). Benign tumors such as lipomas and hemangiomas or productive bony lesions (posttraumatic or degenerative) may be responsible.
-
Level of proximal forearm: is the most common site of compression usually by a thickened proximal edge of the flexor digitorum superficialis muscle,
or with a fibrous band between pronator teres and flexor digitorum superficialis.
Kiloh-Nevin syndrome
CLINICAL ASPECTS: Also called anterior interosseous nerve (AIN) syndrome,
this presents as motor deficiency typically by weakened ability to pinch the thumb and index finger together,
tested by asking the patient to make an “OK” sign with the hand.
This sign reflects the weakness of the following muscles: flexor pollicis longus,
radial part of the flexor digitorum profundus of the index finger,
and pronator quadratus.
ULTRASOUND: The causes of AIN syndrome include a compression through a hematoma,
mass or a thickened interosseous artery.
There is also a non-mechanical cause of AIN syndrome,
the Parsonage-Turner syndrome which is an acute brachial neuritis.
Due to the small size of the nerve and its relatively deep location,
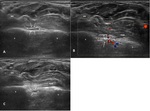
the identification with color or power Doppler of the adjacent anterior interosseous artery at the volar aspect of the interosseous membrane helps to assess the position of the nerve (Fig. 2).
Longstanding disease may be suggested with sonographic changes of atrophy of the innervated muscles.11
WRIST
Carpal tunnel syndrome
Carpal tunnel syndrome (CTS) is the most common entrapment neuropathy and consists in the compression of the median nerve as it courses through the carpal tunnel.
The prevalence of CTS is approximately 2% of the adult population with a lifetime incidence of 10% (15% in patient with occupational risk).
Women are affected 3-5 times more often than men,
and CTS is bilateral in up to 50% patients.
The median nerve provides sensory and motor innervation to the thumb,
index,
third digit,
and radial half of the fourth digit.13
CLINICAL ASPECTS: Clinically patients complain of nocturnal pain,
clumsiness,
tingling and numbness in the median nerve distribution.
Typically,
sensory loss precedes a motor deficit.
There may be a wasting of the soft tissues in the thenar eminence on physical examination.
ULTRASOUND: The diagnosis of CTS is usually made on the basis of typical clinical signs and symptoms as well as electrodiagnostic testing.
Although the cause for median nerve entrapment is,
most of time,
idiopathic,
in selected cases US can demonstrate the cause of nerve compression:
-
Thickening of the flexor retinaculum due to osteoarthritis,
mechanical overuse or trauma.
-
Increased carpal tunnel content as result from a wide variety of causes:
-
Ganglion cysts.
-
Anomalous muscles in the tunnel (e.g.
variations in palmaris longus muscle,
palmaris profundus,
proximal origin of the lumbricalis muscles,
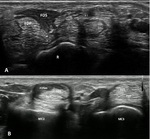
digastric flexor digitorum superficialis tendon for the index finger) (Fig. 3).
-
Tenosynovitis related to inflammatory arthritis or from mechanical overuse.
-
Deposition of amyloid or gout.
-
Radiocarpal synovitis due to osteoarthritis or inflammatory rheumatologic diseases.
The diagnosis on US can be made with the demonstration of:
-
Nerve enlargement assessed by comparing the difference in cross-sectional area between the nerve in the carpal tunnel and proximally at the level of the pronator quadratus muscle in the distal forearm,
with a Δ > 2 mm2 value.
The evaluation must cover the entire course of the median nerve in the carpal tunnel because rarely the major swelling area is distally at the carpal tunnel instead of proximally; this feature is known as “inverted notch” sign14-15.
A bifid median nerve is a possible variation of the nerve anatomy which can be present with a persistent median artery.
The nerve can be partially or complete bifid or even trifid.
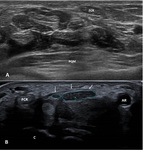
The evaluation of the cross sectional area is done by summing the areas of the lateral and medial branches of nerve with a new cutoff Δ value of 4 mm2 instead of 2 mm2 (Fig. 4).
-
Distal flattening of the median nerve.
-
Palmar bowing of the flexor retinaculum.
Palmar Cutaneous Branch of the Median Nerve
Proximal to the flexor retinaculum the median nerve gives off a small sensory branch close to the flexor carpi radialis tendon: the palmar cutaneous nerve.
US can identify the palmar cutaneous branch and characterize its abnormalities.
Complaints of sensory deficit in the palmar triangle and thenar eminence suggest a neuropathy of this branch.
The nerve can be affected in patients who have undergone carpal tunnel release or other interventions such as a resection of a ventral carpal ganglion cyst,
patients with history of penetrating trauma.
ULNAR NERVE
Ulnar nerve entrapment can occur at the elbow with the cubital tunnel syndrome and at the level of the wrist in Guyon's canal syndrome.
Cubital tunnel syndrome
Ulnar nerve compression is the second most common nerve entrapment of the upper extremity.
The nerve is compressed in the cubital tunnel,
a fibro-osseous tunnel formed by olecranon process laterally,
medial epicondyle medially,
elbow joint capsule and posterior band of the medial collateral ligament anteriorly,
and Osborne’s retinaculum (incl.
the arcuate ligament) posteriorly.
While the Osborne retinaculum executes a static compression over the ulnar nerve,
flexion of the elbow causes instead a dynamic increase of pressure within the cubital tunnel and increased tensile load on the ulnar nerve. Individuals with recurrent anterior dislocation of the ulnar nerve during elbow flexion,
known as snapping ulnar nerve syndrome,
have an increased risk of developing a cubital tunnel syndrome.
CLINICAL ASPECTS: Patients present with pain,
paresthesia and weakness in the fifth finger and ulnar side of the fourth finger,
as well as numbness in the dorsal ulnar aspect of the hand and these fingers.
Chronic compression may lead to claw deformities of the fourth and fifth fingers.
In cases of snapping syndrome the patient may complain a snap during elbow flection.
The repetitive dislocation and reduction by flexion and extension can lead to friction neuritis (Fig. 5).
Causes of dislocation are the absence of the cubital tunnel retinaculum,
a laxity of the arcuate ligament or a shallow epicondylar groove.16
ULTRASOUND: US shows enlargement of the ulnar nerve at the level of cubital tunnel with hypoechoic appearance and loss of honeycomb-like fascicular pattern of the ulnar nerve.
Actual cut-off value of ulnar nerve cross-sectional area is 10 mm2,
but a ratio of the cross-sectional area between the location of maximal nerve swelling (generally at the level of epicondyle) and proximal at the level of medial triceps head is used to overcome individual variations.
A CHR,
cubital-to-humeral nerve area ratio over 1.4 is considered a positive value when associated with structural changes of the nerve.
Dynamic sonography during flexion and extension is a real-time method of evaluating the transient dislocation and can visualize both the nerve and medial head of the triceps.
A more distal site of compression can be located at the level of flexor carpi ulnaris (Fig. 6).
The role of US is also to exclude external compression,
space-occupying lesions (tumors,
ganglia,
hematomas),
synovitis from elbow joint,
regional inflammation and accessory muscles (e.g.
anconeus epitrochlearis) (Fig. 7).17-22
Guyon’s canal syndrome
Guyon's canal is an oblique fibro-osseous triangular tunnel with a length of about 4 cm.
The pisiform bone forms the medial side of the canal,
the flexor retinaculum and the superficial volar carpal ligament form the deep and superficial boundaries respectively.
Guyon canal syndrome is uncommon to rare.
CLINICAL ASPECTS: Guyon’s canal syndrome leads to initial paresthesia and later motor abnormalities in the distribution of the fourth and fifth digits as well as weakness in the midpalmar muscles.
ULTRASOUND: US typically show swelling of the ulnar nerve.
Cross-sectional area measurements are performed proximal of the distal radioulnar joint and distally at the maximum swelling of the nerve in Guyon’s canal.
The examiner must pay attention to space-occupying lesion such as lipoma,
varices,
ulnar artery pseudoaneurysm,
or ganglion cyst from pisotriquetal joint.
RADIAL NERVE
The radial nerve courses in the arm in the spiral groove posterior to the humerus at the level of the elbow joint.
It divides into a superficial sensory branch,
which courses in the forearm,
and a deep motor branch that enters the radial tunnel.
The motor branch,
as it exits from the radial tunnel runs between the superficial and deep supinator muscle,
and as this exits from the posterior aspect of the supinator muscle takes the name of posterior interosseous nerve (PIN).
After leaving the supinator,
the posterior interosseous nerve courses down the dorsal surface of the interosseous membrane,
further dividing into small branches that extend into the extensor muscles of the forearm and ends at the dorsal aspect of the wrist supplying dorsal carpal proprioception.
Compression of the motor branch at the elbow can lead to either radial tunnel syndrome or posterior interosseous nerve syndrome (also called supinator syndrome).
Proximal compression of the sensory branch is rare and can mimic radial tunnel syndrome.
Superficial radial nerve entrapment can occur at the level of the forearm and wrist with the Wartenberg's syndrome.
Radial tunnel syndrome and supinator syndrome (PIN syndrome)
CLINICAL ASPECTS: Radial tunnel syndrome presents as tenderness and pain at the lateral aspect of the proximal forearm mimicking lateral epicondylitis with or without motor weakness.
Clinical manifestation of the PIN syndrome mostly presents with painless palsy of the extensor muscles of the forearm.
ULTRASOUND: US shows enlargement of the PIN proximal of the compression site with or without hypoechoic changes in nerve fascicles.
The normal mean cross-sectional area of the radial nerve has been estimated to be 7.2 mm2 at the humeral shaft,
6.2 mm2 at the intermuscular septum,
and 2,3 mm2 at the supinator area.
The presence of hyperemia can be found on color or power Doppler imaging.
The most common site of compression is the arcade of Frohse that represents a thickened tendinous proximal edge of the superficial head of the supinator: most commonly.
Other structures such as a thickened leading edge of the extensor carpi radialis brevis muscle and distal ligamentous margin of the supinator muscle can lead to nerve entrapment (Fig. 8).
Another rare compression can be caused by crossing branches of the recurrent radial artery,
the so called "leash of Henry" (LoH).
Other rare causes are space occupying lesions such as tumor (i.e.
lipomas) ganglion or bicipitoradial bursitis.
An additional US sign is the atrophy of the dorsal extensor muscles caused by denervation.23-32
Lesions of the cutaneous sensory branch
An isolated lesion of the sensory branch of the deep radial nerve at the dorsal aspect of the wrist,
that provides only innervation of the dorsal wrist joint,
is rare.
It may be compressed by a radiocarpal ganglion,
cannulation of the cephalic vein and wrist overuse (Fig. 9).
Wartenberg’s syndrome
CLINICAL ASPECTS: Wartenberg’s syndrome is an entrapment neuropathy of the superficial branch of the radial nerve at the level of the distal forearm and wrist.
The patient presents with pain,
numbness,
and paresthesia in the radial-side of the wrist and thumb.
De Quervain’s disease and proximal intersection syndrome should be excluded.
Wartenberg’s syndrome may be associated with de Quervain’s disease or be secondary to decompressive surgery of the first compartment.
Other possible causes can be a compression from a hematoma after an intravenous cannulation or a chronic external compression due to bandages (e.g.
jewelry,
handcuff or wristwatch).
ULTRASOUND: US shows nerve swelling and loss of normal fascicular echotexture.
The role of US is to distinguish Wartenberg's syndrome from de Quervain's disease or arthritis of the trapeziometacarpal joint.
US can show secondary nerve compression from adjacent scar tissue or post-traumatic/postoperative changes of the soft tissue.
Posterior antebrachial cutaneous nerve (posterior cutaneous nerve of arm)
The cutaneous antebrachii posterior nerve arises from the radial nerve and travels subcutaneously with the cephalic vein towards the posterior elbow and antebrachial region.
Its compression can be due to posttraumatic scar tissue,
leading to pain syndromes.
Ablation of the posterior cutaneous nerve of arm under US-guidance has been recently proposed to treat refractory lateral elbow pain syndromes.33
MUSCULOCUTANEOUS NERVE
And lateral antebrachial cutaneous nerve (LABC).
The musculocutaneous nerve (MCN) is the fourth major nerve of the upper extremity.
It arises from the lateral cord of the brachial plexus and,
after piercing the coracobrachialis muscle,
descends along the lateral aspect of the arm passing obliquely between the biceps and the brachialis muscles to continue in the forearm as the lateral antebrachial cutaneous (LABC) nerve after piercing the brachial fascia.
At this point the nerve travels behind the cephalic vein and divides itself into volar and dorsal branches.
Cases of MCN neuropathy are rare.
Compression within the coracobrachialis muscle can be due to heavy exercises and hypertrophy of biceps brachii and brachialis muscles can lead to entrapment between the two muscles.
The clinical presentation of a proximal MCN neuropathy is a painless weakness flexion of the elbow and supination of the forearm.
Distal involvement of the LABC nerve leads to numbness or neuropathic pain over the elbow and radial side of the forearm.
Patients typically have a history of injury or overuse of the elbow with activities such as weightlifting and tennis.
The most commonly reported area of entrapment is at the point where the nerve emerges from beneath the biceps tendon and pierces the deep fascia,
proximally or at the elbow crease.
The lateral margin of the biceps aponeurosis exerts a compression force on the LABC nerve as the elbow extends,
and the nerve is caught between the biceps tendon and the brachialis fascia.
A specific cause of compression can be a proximal biceps rupture with a distal migration of the biceps muscle,
causing a compressive neuropathy of the LABC nerve.
Identification of the LABC nerve can be done by locating the MCN piercing the coracobrachialis muscle and following it distally where it runs lateral to the biceps brachii tendon and subsequently pierces the superficial antebrachial fascia.34-36
MEDIAL ANTEBRACHIAL CUTANEOUS NERVE
The medial antebrachial cutaneous nerve (MACN) arises from the medial cord of the brachial plexus.
The nerve runs parallel to the brachial and basilic vein until it pierces the superficial antebrachial fascia.
It then runs in the subcutaneous tissue.
Its anterior and posterior branches innervate the medial portion of the forearm.
Lesions and entrapments of this nerve are described after ulnar nerve surgery.36-37