General considerations
Musculoskeletal findings in multiple myeloma (MM) typically occur in one of several patterns.
The disease can be disseminated,
with lesions usually affecting the axial skeleton,
or focal,
with a mass of plasma cells forming a plasmacytoma.
- The disseminated form classically has multiple lytic lesions,
described as 'punched out'.
It is also recognised that disseminated disease can alter the appearance of the bone marrow without identifiable lesions; the relative reduction of fat content within the marrow is identifiable on MRI but not specific for disease.
- Plasmacytomas are usually a solitary mass,
most frequently seen in the spine or pelvis.
Occasionally multiple plasmacyomas are seen.
Traditionally patients have been assessed using a skeletal survery,
but it is now well recognised MRI is more sensitive for detecting lesions and this now forms the bulk of the imaging.
Classic MM deposits are usually relatively hypointense on T1 weighted sequences,
and hyperintense on fluid-sensitive sequences such as T2 weighted or STIR images.
If contrast is given,
the lesions enhance avidly early.
Whilst these signs are non-specific,
finding the combination of these and the axial location is highly suspicious for MM; diagnosis is also through serum and bone marrow examinations.
When there are atypical lesions or locations on a background of known myeloma,
diagnosis can be more challenging.
Image review
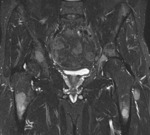
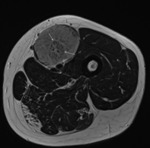
Figure 1 shows typical myelomatous lesions within the pelvis and proximal femora.
There are large subtrochanteric lesions that pose a risk of pathological fracture.
Features are consistent with the disseminated pattern of MM.
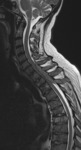
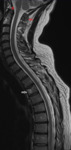
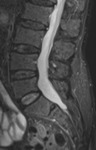
Figure 2 demonstrates one of the more concerning presentations of myeloma - spinal cord compression.
This is a relatively common presentation,
seen in up to 25% of cases but the usual cause is a pathological fracture in MM.
The incidence of compression from an epidural mass has not been documented in the literature,
but as extraosseous disease is seen in less than 5% of patients it is likely to be fractions of a percent.
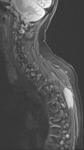
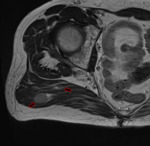
Figure 3 shows a soft tissue mass in the dorsal soft tissues,
in keeping with a plasmacytoma. The International Myeloma Working group classifies solid plasma cell tumours as solitary plasmacytoma of bone (SPB),
extramedullary plasmacytoma (EP) or multiple plasmacytomas (MP). EPs are rare,
accounting for less than half the cases of extraosseous myeloma,
and the majority of EP cases involve the upper respiratory tract.
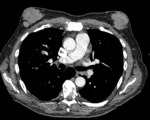
Figure 4 demonstrates bilateral soft tissues masses in the breasts of a male.
Biopsy confirmed these as MPs.
Review of the literature shows fewer than 100 cases of breast involvement reported in the last century,
and the majority of these were unilateral.
It is worth noting gynaecomastia can be a complication of MM treatment,
which may confuse the clinical picture.
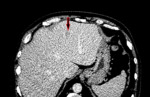
Figure 5 shows a small,
indeterminate lesion in the left lobe of the liver not present on the previous imaging.
Liver involvement occurs in approximately 40% of cases of myeloma,
but is usually a diffuse infiltration and nodular lesions are only rarely reported.
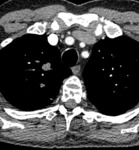
Figure 6 demonstrates a lobulated soft tissue nodule medially in the right upper lobe.
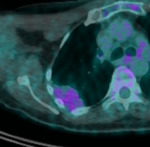
Figure 7 shows a pleurally based lesion in a different patient.
Lung involvement is again rare in myeloma,
and can present as masses,
consolidation or diffuse infiltration.
Pleural involvement more usually manifests as diffuse pleural thickening or an effusion.
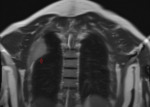
Figure 8 is a scout image from an MRI of the same patient as in figure 7,
and serves as a reminder to assess all available images when reporting.
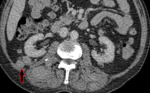
Figure 9 shows retroperitoneal MPs,
seen as well-circumscribed soft tissue masses.
In the retroperitoneum they have a predilection for the perirenal space due to the stem cell environment here.
A more rare presentation of retoperitoneal myeloma is as a process mimicking retroperitoneal fibrosis.
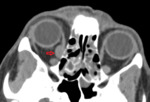
Figure 10 depicts an EP within the right medial rectus muscle.
Intraorbital myeloma is very uncommon,
and usually presents as proptosis secondary to growth of an osseous lesion extending into the orbit rather than primary soft tissue mass.
This patient complained only of some blurring of vision.
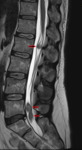
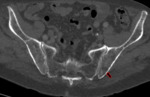
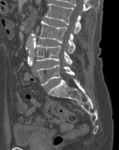
Figures 11 and 12 are from the same patient.
The former demonstrates a typical SPB in C1,
as well as other stigmata of multiple myeloma.
The latter shows lesions associated with the sacral nerve roots; CSF analysis confirmed plasma cells.
Whilst drop metastases are possible in the intradural compartment,
this patient had no evidence of dural infiltration at C1 and the assumption is that these are de novo MPs in the cauda equina.
Intradural EP/MPs are extremely rare,
with only a handful of cases reported in the literature.
Figures 13 and 14 are from the same patient,
who had multiple biopsy-confirmed MPs.
There appeared to be separate populations of tumours,
with several - including the large thigh lesion - appearing infiltrative,
whereas others - for example the gluteal lesions - are more well-defined.
This demonstrates the variable nature of EPs.
Myeloma is more common as age increases,
and it is not uncommon for patients to have concurrent cancers.
Figures 15 - 17 are from the same patient,
who had previously been treated for MM and presented with back pain.
The MRI of the spine performed detected an incidental renal tumour,
confirmed as renal cell carcinoma (RCC).
This MRI and the subsequent CT of the trunk showed multiple osseous lesions with different characteristics.
The features of multiple,
axial lytic lesions without extraosseous extension or periosteal reaction are more in keeping with MM than RCC; the sclerotic border is suggestive of treated MM; however,
the signal characteristic were atypical for this on MRI.
Biopsy was performed for confirmation of the suspected MM,
with evident significant impact on treatment planning.