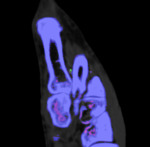
MSU deposits on dual energy CT
In patients with gout,
MSU deposits occur within joints,
tendons,
bursae,
fasciae,
or cartilage (3). In keeping with the lower limb predilection of gout clinically,
MSU deposition on DECT is more common in the lower limb (1,4).
The most common lower limb sites of MSU deposition on DECT include the 1st MTP joint,
ankle joint,
Achilles and peroneal tendons,
followed by the tendons,
bursae and menisci around the knee (4).
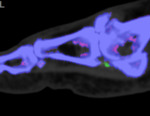
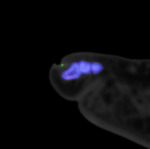
Figure 1 is a colour-coded image demonstrating intra-articular MSU deposit in the 1st metatarsal phalangeal joint (purple pixels). Note the presence of a 1st MTP joint erosion.
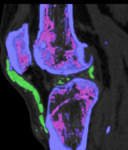
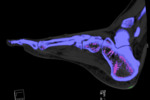
Figure 2 demonstrates MSU deposition within the patella tendon shaded purple on DECT colour-coded image.
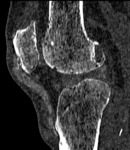
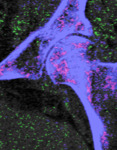
There is also MSU deposition in the lateral meniscus of the knee. Note that MSU deposition in the patella tendon and lateral meniscus is also visible as increased attenuation in the gray-scale conventional CT image in Figure 3.
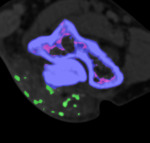
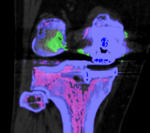
Figure 4 demonstrates MSU deposition within the olecranon bursa.
False positive findings and artefacts
Artefacts are very common in dual energy CT,
present in up to 90% of studies in one series,
particularly in skin and nail bed (5).
1) Artefact from skin and nail beds
Artefacts mimicking MSU deposition are common in the nail and thickened skin,
thought to be due to the similarity of changes in attenuation of keratin and MSU at different CT energies (5).
Figure 5 demonstrates artefact in the toenail.
Figure 6 demonstrates artefact in thickened skin along the plantar aspect of the heel. This artefact is sometimes also seen in skin creases.
2) Beam hardening artefacts and noise
Changes in attenuation due to noise and beam hardening may be interpreted by software algorithms as MSU deposition,
which can often be distinguished from genuine MSU deposition by their distribution. Noise produces random submilimetre artefacts which do not relate to any anatomical structure,
and is a particular problem when attempting to image larger joints,
as demonstrated around the left hip on Figure 7.
Beam hardening artefact is limited to the path of beam hardening. Figure 8 demonstrates metallic beam hardening artefact around the knee secondary to a knee prosthesis,
which is interpreted by software algorithms as MSU deposition.
3) Advanced degenerative change
False positives are also demonstrated on dual energy CT in the presence of advanced degenerative changes (6). This may be due to MSU within degenerative cartilage.
4) Vascular ‘artefact’
‘Artefacts’ mimicking MSU deposition are occasionally demonstrated along blood vessels (5),
as demonstrated in Figure 9. It is unclear if this represents vascular MSU deposition or artefact from noise in small calcified vessels.
False negative studies
The overall sensitivity of dual energy CT for detection of MSU deposits in patients with gout is generally considered to be high,
87%-88% in systemic reviews (2,7). However there is variation in sensitivity between studies. This may partly be due to patient selection. Factors that may influence the sensitivity of dual energy CT include :
1) Duration of disease. A short duration of disease of < 6 weeks is associated with false negatives (6).
2) MSU lowering therapy. Treatment with MSU lowering agents such as allopurinol has been suggested as a cause of false negative results for gout on DECT (8,
9). In a recently published study of 152 patients,
69% of patients with a diagnosis of gout being treated with MSU lowering therapy for an average of 5 years had evidence of MSU deposition on DECT (9).
3) Non-tophaceous gout.
The meta-analyses include studies in patients with chronic tophaceous gout.
In newer studies limited to patients with non-tophaceous gout,
the sensitivity of dual-energy CT ranges from 64% to 90% (6,
10)
Limitations of dual energy CT
The ability of DECT to detect individual MSU deposits may depend on the size and density of the MSU deposits. A possible explanation for this is that conventional dual energy CT analysis utilise a pixel threshold CT value (typically +150 Hounsfield Units),
only above which a pixel is identified as containing MSU (5,
6,
11).
Pathologically proven MSU crystals in tophi that are occult on dual energy CT have been documented (11).
It follows that dissolved MSU or small MSU crystals within synovial fluid in a symptomatic joint may be occult on dual energy CT. In an in-vitro study using synovial fluid containing a high concentration of MSU,
DECT did not detect MSU deposition (12). In vivo studies with proven MSU on aspirate and microscopy show variability on whether MSU deposition is detectable on DECT at the joint which is symptomatic,
ranging from 25%-90% of joints (6,
10). Thus,
DECT may not necessarily be a reliable technique in establishing if a particular joint is involved in a patient with known gout.
The diagnostic performance of dual energy CT to detect MSU deposits is known to vary depending on the parameters used in the software analysis,
in particular the slope of attenuation at one energy versus attenuation at another energy that defines whether a pixel is ascribed as calcium or MSU (13).
These parameters are manufacturer determined but can be modified in some software packages (1,
13).
It is important to note that dual energy CT demonstrates MSU deposition which in itself may not necessarily equate to a diagnosis of gout. MSU deposition on dual energy CT has been demonstrated in patients with asymptomatic hyperuricaemia,
albeit in smaller quantities and at lower incidence that in patients with symptomatic gout (14).
The diagnostic performance of dual energy CT in detecting MSU deposition within larger joints and within the axial skeleton is also unproven. For example,
the intervertebral discs are a known site of MSU deposition in patients with gout (3). However,
similar degrees of apparent MSU deposition in the intervertebral discs have been demonstrated on DECT in patients with gout and age-matched controls (15),
suggesting DECT findings in intervertebral discs may be artefactual.