Knowledge of basic nerve anatomy is important for accurate interpretation of nerve imaging. Individual nerve fibers are encircled by the endoneurium,
and a group of nerve fibers are encircled by the perineurium to form a fascicle.
A group of fascicles is in turn encircled by the epineurium,
which represents the outermost layer of a nerve.
Interspersed between the fasciculi are blood vessels which run longitudinally within the nerve.
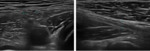
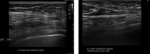
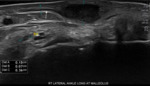
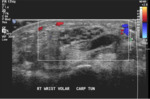
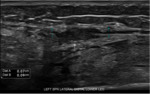
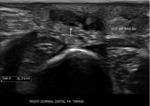
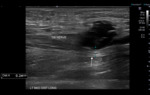
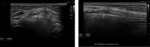
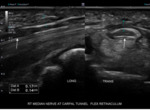
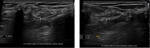
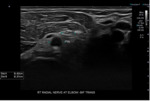
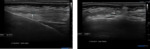
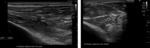
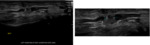
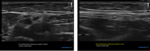
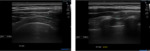
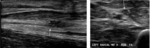
Nerve anatomy can be identified on high resolution ultrasound up to the fascicular level (Figures 1,2,3,4). In the transverse orientation,
nerves demonstrate a typical “honeycomb” appearance which reflects the normal fascicular architecture. The surrounding epineurium is hyperechoic.
Longitudinally,
nerves demonstrate parallel lines of hyper- and hypoechogenicity.
Masses:
Space-occupying mass lesions of peripheral nerves include peripheral nerve sheath tumors,
neuromas,
intraneural ganglion cysts,
and fibrolipomatous hamartomas.
Peripheral nerve sheath tumors can be benign (ie.
schwannoma or neurofibroma) or malignant. Schwannomas arise eccentrically from the peripheral nerve whereas neurofibromas arise within the nerve. Malignant peripheral nerve sheath tumors are often large and demonstrate aggressive features. Clinical presentation reflects location of the lesion and the parent nerve. In general,
peripheral nerve sheath tumors are identified on ultrasound as hypoechoic masses that are seen in continuity with the peripheral nerve on ultrasound (Figure 5).
Fibrolipomatous hamartomas are rare benign tumors that most commonly affect the median nerve (Figure 6).
They present as slowly growing masses that cause progressive pain on the volar aspect of the wrist.
Hypoechoic adipose tissue can be seen interspersed between the nerve fascicles,
a finding which can also be confirmed on MRI.
Neuromas of peripheral nerve can occur after traumatic laceration or iatrogenic transection (ie.
in the setting of amputation or mass resection). Traumatic neuromas occur after high grade nerve injury,
after which the regenerating neurons fail to heal in an orderly manner,
resulting in a haphazard arrangement of nerve fibers that manifests as a hypoechoic mass in continuity with the peripheral nerve (Figure 7). In the case of complete nerve transection,
a stump neuroma can develop (Figure 8),
resulting from disordered regeneration of the proximal segment of the transected nerve.
Extrinsic mass lesions can abut and cause mass effect on peripheral nerves,
resulting in clinical symptoms reflective of the parent nerve. For example,
peripheral soft tissue sarcoma can cause compressive nerve pathology on adjacent nerves (Figure 9). Distinction between the nerve itself and the mass is crucial on ultrasound as well as identifying the degree of nerve caliber change.
Neuritis:
Neuritis is a general term describing inflammation of a nerve leading to clinical symptoms reflective of parent nerve dysfunction such as pain,
paresthesia,
weakness,
and muscle wasting dependent on the nerve involved. Ultrasound can detect characteristic findings of neuritis of peripheral nerves such as hypo-echogenicity of the nerve,
nerve enlargement,
and disruption of fascicular architecture (Figure 10).
Neuritis can result from a variety of etiologies including stretch injury,
iatrogenic injury,
and nerve compression as in the case of carpal tunnel syndrome (Figure 11).
In cases of neuritis,
ultrasound may be used for guidance of perineural injections (Figure 12). Perineural injection of only anesthetic can be performed as a diagnostic test,
with documentation of pre- and post- procedural pain score. Perineural injection of anesthetic and corticosteroid can be performed as a therapeutic intervention.
While performing ultrasound evaluation for neuritis of a peripheral nerve,
attention to adjacent nerves or branches of peripheral nerves may be helpful in some cases. For instance,
when evaluating the radial nerve at the elbow,
both the deep and superficial branches of the radial nerve should be examined sonographically (Figure 13). Evaluation of an inflamed nerve distally to the point of normalization is also important,
and may sometimes involve imaging small branches of peripheral nerves (Figure 14). In cases of suspected neuritis of very small peripheral nerves,
subtle findings may be observed and comparison to the contralateral side can be extremely helpful (Figure 15).
Laceration:
High-resolution ultrasonography can be used for evaluation of peripheral nerve trauma,
both in the acute and non-acute settings.
Ultrasound can demonstrate laceration of peripheral nerves through partial or complete disruption of nerve fibers. Sonographic findings of traumatic nerve injury in the acute setting include focal nerve hypo-echogenicity,
thickening,
and loss of fascicular architecture at the site of injury which may demonstrate overlying soft tissue edema on ultrasound as well as cutaneous findings of trauma on direct visual inspection (Figure 16). In the case of complete nerve transection,
the proximal and distal segments of the injured nerve should be identified with measurement of the “nerve gap” (Figure 17). In the non-acute setting,
stump neuromas may be identified both proximally and distally after complete nerve transection (Figure 18).