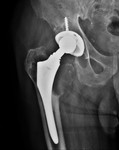
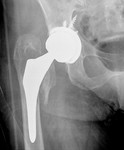
We selected images of plain radiographs that display the normal imaging findings after a hip arthroplasty from the archives of our institution.
We also selected radiographs that show the imaging findings of the most common complications of hip arthroplasty.
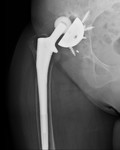
NORMAL POSTOPERATIVE FINDINGS
The initial posteroperative radiography must be acquired in a standard way since sequential radiography is the most valuable method for detecting complications.
The recommended initial posteroperative radiography is a standing anteroposterior pelvic radiograph,
with the hips in internal rotation and extension.
The centre of the x-ray beam should be focusing on the pubic symphysis to provide the inclusion of the entire hip prosthesis and cement.
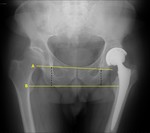
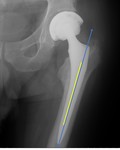
Evaluating a hip arthroplasty includes multiple parameters such as leg length,
vertical and horizontal centre of rotation,
lateral acetabular inclination and femoral stem positioning (Fig. 1).
The acetabular anteversion can also be determined from a true lateral radiograph.
Leg length is measured as the distance between a line connecting the inferior border of the acetabular tear drops (pelvic reference line) and a line crossing the middle of the lesser trochanters (femoral reference line) – Fig. 2.
After hip arthroplasty,
leg length discrepancy is common.
A discrepancy of up to 1 cm is well tolerated; bigger inequalities can be corrected with an orthosis if needed.
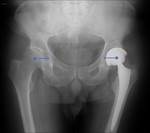
The horizontal centre of rotation is measured as the distance between the centre of the femoral head and the lateral outline of the teardrop shadow – Fig. 3.
This distance should be equal to the contralateral hip,
as close to the normal anatomy as possible.
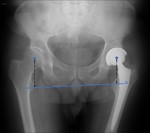
The vertical centre of rotation is measured as the distance between the centre of the femoral head and a line crossing the ischial tuberosities (transischial tuberosity line) – Fig. 4.
As the horizontal,
this distance should be equal to the contralateral hip.
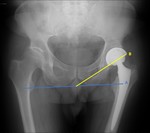
The acetabular inclination is measured as the angle between a line that crosses the medial and lateral margins of the acetabular cup (acetabular axis) and the transischial tuberosity line – Fig. 5.
The normal angle ranges between 30 and 50º; smaller angles provide stability,
but a reduced abduction.
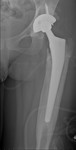
The longitudinal axis of the femoral stem should be aligned with the longitudinal axis of the femoral shaft and the tip of the stem located in the centre of the shaft (Fig. 6).
The acetabular anteversion cannot be determined on an anteroposterior view and it requires an additional radiograph on a lateral view.
It is measured as the angle between the acetabular axis and the coronal plane.
The normal angle ranges between 5 and 25º anteversion,
since it permits adequate flexion of the hip.
In cemented prostheses,
the interfaces between the cement and bone,
cement and prosthesis and the cement thickness should be analysed,
searching for gaps or lucencies.
Regarding the femoral cement mantle,
a thickness of 2-3 mm is warranted.
There is no consensus regarding cement mantle thickness of the acetabular component.
For standardized description of cement-related or periprosthetic abnormalities of the acetabular and femoral components,
there is a template described by Charnley-Delee and Gruen,
respectively.
According to this classification,
the bone adjacent to the acetabular component is divided into three zones labelled I,
II and III,
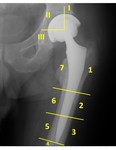
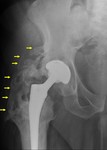
from lateral to medial on an anteroposterior view (Fig. 7).
Bone adjacent to the femoral component is divided into seven zones on an anteroposterior view: the first three zones are numbered from proximal to distal on the lateral aspect,
zone 4 is located at the tip of the stem and the last three zones are numbered from distal to proximal on the medial aspect (Fig. 7).
MOST COMMON COMPLICATIONS
Based on their radiographic appearance,
the most common complications can be categorized in three groups: periprosthetic lucencies,
sclerosis and bone proliferation and component failure/fracture.
PERIPROSTHETIC LUCENCIES
The challenge in evaluating lucencies around hip prosthesis is to be able to differentiate pathological from nonpathological causes.
In non-cemented arthroplasties,
a lucency with <2 mm of thickness delineated by a thin sclerotic line with no progression after 2 years is considered normal,
representing a segment of fibrous bony ingrowth and providing enough stability.
In cemented arthroplasty,
a fibrous reaction to cement at the bone-cement interface appears as a < 2 mm lucency also limited by a thin sclerotic line.
This is interpreted as a stable fibrous membrane.
A thin radiolucent zone at the component-cement inferface can be considered as normal if stable.
A periprosthetic lucency wider than 2 mm and/or a progressive increase of thickness in sequential radiographs are signs of an abnormality.
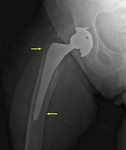
Osteolysis/aseptic loosening is a biological process causing an aseptic foreign body granulomatous reaction.
This causes the implant to become separated from the bone which results in mechanical loosening.
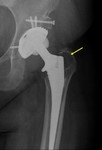
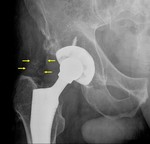
The radiographic feature of this pathological process is a periprosthetic lucency that slowly extends around the bone-cement or bone-prosthesis interface (Fig. 8 and Fig. 8 Fig. 9).
Infection is a devastating complication and,
just like aseptic loosening,
its radiographic features include a periprosthetic lucency around the bone-cement or bone-prosthesis interface.
The presence of soft tissue abnormalities,
periosteal reaction or a rapid progression of the disease favours infection.
There are other complications that may manifest as lucency in radiography but only in longstanding cases.
These complications include metallosis (Fig. 10),
aseptic lymphocytic vasculitis associated lesions and pseudotumours.
SCLEROSIS AND BONE PROLIFERATION
Just like lucencies,
there are some signs of sclerosis and bone proliferation associated with hip prostheses that are nonpathological.
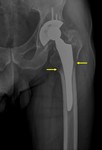
Spot welding is the formation of bone originating from the endosteal surface,
is more common in non-cemented femoral stems (Fig. 11) and is a strong indicator of stability.
Hip arthroplasty causes a shift of mechanical forces from the femoral neck and intertrochanteric region to the proximal femoral diaphysis.
This leads to bone reabsorption on the lateral side of the proximal femur and bone hypertrophy at the medial side.
This process is called stress shielding and is a sign of stability.
Bone pedestal is a bone bridge between the cortex and the tip of a non-cemented femoral stem.Its association with complications remains unclear.
Heterotopic bone formation is the process of bone development outside its usual location in the skeleton.
It occurs in about half of the patients but rarely limits movement.
Risk factors are infection,
posttraumatic arthritis,
ankylosing spondylitis and previous hip surgery.
The radiographic description of this finding is made according to the Brooker classification on an anteroposterior view: grade 0,
no heterotopic ossification; grade 1,
one or two foci of heterotopic ossification less than 1 cm each (Fig. 12); grade 2,
ossification or osteophytes occupying more than half the space between the pelvis and femur; grade 4,
ossification that bridges the pelvis and femur (Fig. 13).
COMPONENT FAILURE/FRACTURE
During the first years after surgery it may be normal for some types of prosthesis to migrate but any progressive movement more than two years after surgery or superior to 10 mm is abnormal.
Linear wear can occur in every arthroplasty that uses a layer of polyethylene and radiographically it appears as an asymmetric position of the femoral head within the acetabular cup.
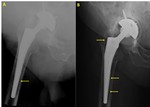
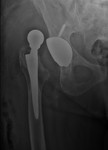
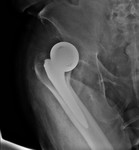
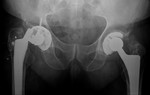
Dislocation most commonly occurs in the early posteroperative period due to the initial weight bearing (Fig. 14 ,
Fig. 15 and Fig. 16).
There are some factors that increase the likelihood of dislocation such as excessive lateral positioning of the acetabular component,
a >50º angle of acetabular inclination or acetabular retroversion.
Early dislocation is frequently treated with conservative treatment but dislocation after five years of surgery generally requires a new surgical intervention.
Periprosthetic fractures can be intra or postoperative and most often occur around the femoral component.
Intraoperative fractures are more associated with non-cemented components.
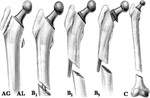
Postoperative fractures are associated with episodes of minor trauma and can be divided into three types according to the Vancouver classification (Fig. 17).
Type A fractures are peritrochanteric fractures (Fig. 18),
type B occur around or just below the tip of the stem and type C occur far from the femoral stem and their treatment is independent from the prosthesis.
Type B fractures are the most common (Fig. 19 and Fig. 20).
Prosthetic fractures also occur most commonly in the femoral stem and usually affect prostheses that are mobile proximally and fixed distally resulting in fractures through the middle or proximal third of the stem.
Risk factors for prosthetic fractures include anything that induces a metal-fatigue stress such as increased body mass index.
Varus malpositioning of the stem also predisposes to this type of fractures (Fig. 21).