Imaging features are variable,
depending on the age of the patient,
pathogenic agent,
disease severity and imaging modality performed.
It is always important to describe the location of the infection,
if there is a single focus or multiple foci of infection,
as well as the presence of drainable collections.
Signs of poor prognosis are also crucial to depict,
more importantly the presence of extensive subperiosteal abscess or bone marrow ischemia.
5
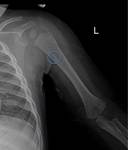
Conventional radiography should be the initial modality to evaluate bone abnormalities.
Bone disease can only be depicted on radiography 7-10 days after onset and radiographic studies have a low sensitivity in the diagnosis of acute osteomyelitis.6 However,
they are useful to plan further imaging studies and help to exclude other conditions such as trauma or tumors.
Soft tissue edema can also be seen,
but is non-specific.
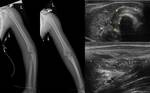
Ultrasound has an important role as it can identify extraosseus findings such as subperiosteal abscesses and fluid collections,
joint effusion,
and deep venous thrombosis.5 It is also the modality of choice to guide joint effusion aspiration and drainage of abscesses.
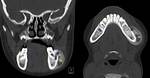
Despite having an excellent spatial resolution for bony structures,
CT importance is limited in childhood due to the amount of radiation involved.
CT is frequently reserved to cases of chronic osteomyelitis in order to depict bony sequestration,
cortical destruction,
and intraosseous gas.2
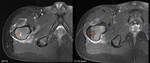
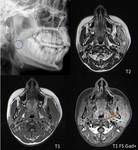
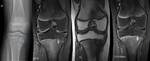
MRI can detect bone marrow edema 1-2 days after onset of infection and allows excellent delineation of bone and soft tissue abnormalities.
In acute osteomyelitis,
bone typically has low-signal intensity on T1W sequences,
with high signal on T2/STIR sequences and enhancement of subperiosteal bone and soft tissue.1 MRI also demonstrates involvement of the growth plate or epiphysis and joint effusion.
Ischemia within areas of infected bone marrow appear as areas with less enhancement than normal or with no enhancement at all on contrast-enhanced sequences.
Detection of reduced enhancement of the marrow is essential,
as it indicates increased disease severity and higher risk of complications such as pathologic fractures,
chronic osteomyelitis and the need for repeated debridement.5
MRI is also the most reliable imaging method for the evaluation of intraosseus collections.
They are seen as areas of high signal intensity on STIR and T2-weighted sequences.
After gadolinium,
the typical appearance is an area of nonenhancement with a rim of enhanced tissue.5
Although abscesses can be seen consistently on STIR and T2-weighted images,
the use of intravenous contrast increases the confidence for the detection of purulent collections.
Surgical drainage is usually performed for microbiologic diagnosis,
but it also helps to control infection and preservation of function.6 Therefore,
MRI plays a central role in the diagnosis of complications and planning of surgical treatment.
Chronic osteomyelitis is usually characterized by the presence of well-defined soft tissue and marrow abnormalities with cortical thickening,
which is low signal on all STIR,
T1 and T2-weighted images.
In addition,
MRI can illustrate active infection as high T2 signal within these areas of chronic osteomyelitis.
Furthermore,
it Is an excellent method to depict nonenhancing bone sequestrum,
involucrum,
and sinus tracts seen in chronic osteomyelitis.