Tuberculosis is a major public health consideration worldwide and within Europe.
Whilst globally the incidence is falling by 2% each year,
the World Health Organisation states this needs to accelerate to 5%.
[1]
Furthermore,
there is an increasing incidence of multi-drug resistant TB,
necessitating the requirement for early diagnosis.
Extra pulmonary tuberculosis accounts for 25% of disease,
with an estimated 1-3% of cases being musculoskeletal.
[2]
The most common form of skeletal disease is spondylodiscitis,
accounting for approximately 50% of musculoskeletal TB.
[ 3] Tuberculous arthritis of the knee and hip followed by osteomyelitis are the most common forms thereafter.
Isolated soft tissue disease is rare.
[4]
The clinical presentation of extra pulmonary tuberculosis can be indolent and non-specific.
The triad of clinical symptoms,
imaging and microbiology is required for efficient diagnosis.
Whist no imaging features are pathognomonic for musculoskeletal tuberculosis,
it is important for the radiologist to be aware of the imaging manifestations particularly as index of clinical suspicion is often low given that pulmonary and extra-pulmonary disease rarely co-present and clinical presentation can be non-specific.
Tuberculous Spondylitis /Spondylodiscitis
Potts’s disease,
tuberculous spondylodiscitis is the commonest manifestation of musculoskeletal TB.
The clinical presentation is indolent and consists of back pain and constitutional symptoms.
It has a predilection for the thoracic spine and the upper lumbar segments thereafter.
In most cases spread is haematogenous,
through the Batson venous plexus.
In adults,
the vertebral body corner adjacent to the endplate is the most vascular region,
therefore making it the most common site of initial infection.
Non- contiguous and multilevel involvement can help distinguish it from pyogenic spondylitis as the primary differential.
Imaging
Radiography and CT
Radiography is the initial investigation of choice.
Findings may vary according to the natural history of disease.
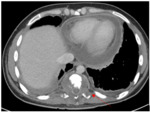
CT provides higher contrast resolution and can better delineate the extent of spinal lesions. It can also demonstrate calcification,
which is characteristic for TB.
Initial radiographs may be normal.
Early features include erosive change at the anterolateral endplate corners.
Commonest findings include vertebral body destruction,
loss of discovertebral height,
bone sequestration and paravertebral soft tissues masses.
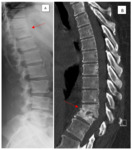
Gibbus deformity refers to short thoracolumbar kyphosis,
when collapsed vertebrae form a wedge.
This most commonly results from TB spondylodiscitis ( Figure 1,2).
Ankylosis is the most definitive hallmark for healing.
Reduction in soft tissue mass,
progression of calcification and recovery of vertebral body height are also features of healing.
MRI
MRI is the investigation of choice for spondylodiscitis.
It is sensitive,
can detect early changes of disease and can assess the spinal canal.
It is not specific.
The bone marrow demonstrates low T1W and high T2W and STIR signal.
The intervertebral discs will demonstrate high T2W signal and demonstrate avid contrast enhancement.
Paravertebral spread into the epidural fat and surrounding soft tissues will also return low T1 and high STIR signal.
Abscesses will return high T1 and low T2 signal and demonstrate contrast enhancement.
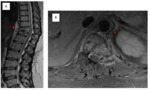
Contrary to this,
phlegmonous collections will appear heterogenous on both T1 and T2 sequences and will not enhance with contrast ( Figure 3,4).
Features of improving or treated disease include reduction in contrast enhancement,
increase in T1 bone marrow signal intensity and return to normal T2 signal ( Figure 5).
[ 3 ]
Tuberculous Osteomyelitis
Extraspinal osteomyelitis is insidious and non-specific in presentation.
Spread is haematogenous and may result from septic arthritis.
It has a predilection for the extremities,
most commonly affecting the hands and feet.
Long bone epiphyseal involvement and extension from the metaphysis can be seen in children.
Imaging features resemble those of bacterial osteomyelitis.
Infection may be multifocal.
Imaging
Plain radiograph and CT
Early imaging may be normal.
Soft tissue swelling is the most common finding.
Other features include cortical destruction,
sclerosis,
joint destruction,
periarticular osteopenia and periosteal reaction ( Figure 6,8,10).
In children,
a cystic form of disease may cause metaphyseal lucencies (termed cystic tuberculosis).
Spread across the epiphyseal plate helps distinguish TB from pyogenic infection.
Spina Ventosa describes cystic expansion of short bones,
such as in dactylitis.
MRI
Affected bone will return low T1 and high T2 and STIR signal.
Overlying inflammatory tissues or abscess formation will demonstrate contrast enhancement ( Figure 7,11).
[5]
Tuberculous Arthritis
Joint involvement has a predilection for the large joints such as the hip and knee and is usually monoarticular.
Direct haematogenous spread or changes secondary to osteomyelitis or septic arthritis result in joint erosion,
loss of the joint spaces and peri-articular osteopenia (Phemister triad).
Ankylosis will result if untreated.
Imaging
Plain Radiograph and CT
Changes may be non-specific.
All features of Phemister triad can be demonstrated on radiograph or CT.
Bone destruction and soft tissue changes may be better appreciated on CT.
Ultrasound
May demonstrate joint effusions,
which can also be seen on radiograph and MRI.
MRI
The synovium is optimally assessed with MRI.
Synovial changes occur in early disease,
with thickening and characteristic low or intermediate T2 signal.
T1 signal may be variable.
Contrast enhancement may occur with confounding infection.
MRI is also more sensitive to the detection of bone erosions,
appearing as low signal foci on T1W images.
Soft tissue
Isolated soft tissue TB is extremely rare and can include cold abscess formation within the soft tissues,
as well as tenosynovitis.
TB tenosynovitis most commonly affects the flexor tendons of the hand.
Spread is usually haematogenous.
Symptoms are non-specific,
presenting with soft tissue swelling and pain.
Imaging
Plain Radiograph and CT
These have a limited role however may demonstrate soft tissue swelling.
Ultrasound
This is the first line investigation for suspected tenosynovitis.
The tendons will appear thickened.
Contrary to a pyogenic tenosynovitis,
there are unlikely to be associated fluid collections.
MRI
MRI changes depend on the stage of disease.
The first stage,
the hygromatous stage,
involves fluid in the tendon sheath without thickening.
The second stage,
serofibrinous stage involves thickening of the tendons with associated high T2W signal within the synovium.
In the final fungoid stage,
a soft tissue mass develops along the tendon.
[ 6]
Myositis
TB myositis is uncommon,
particularly as primary infection.
Spread is usually from adjacent infected structures such as bones or lymph nodes or spread to the psoas muscle from spondylodiscitis.
[7]
Imaging
Plain Radiograph and CT
CT may be useful in assessing underlying bone lesions or collections.
Ultrasound
Ultrasound may demonstrate oedematous soft tissue and muscles.
MRI
MRI is the investigation of choice.
Affected musculature with return high T2 signal and low T1 signal,
with associated diffusion restriction.