The study of two cases with uremic TC in our department,
one rare case presenting with painful palpable soft-tissue masses surrounding multiple joints and one asymptomatic patient incidentally diagnosed with TC on routine CT examination,
generated a review of the literature concerning the imaging appearance of TC and its mimics.
Diagnosis of TC relies on imaging to a great extent [3].
Initial investigation with plain X-ray and ultrasonography is usually very effective.
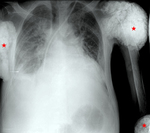
♦ Characteristic radiographic appearance is a multilobulated,
amorphous,
calcified periarticular lesion,
usually located along the extensor surfaces of large joints (Fig.1).
Lesion margins are usually well-defined due to the presence of a fibrous capsule [3,
4].
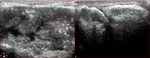
♦ Soft-tissue ultrasound (US) demonstrates characteristic signs of heterogeneously hyper-echogenic lobulated masses along the bursae of large joints,
with solid and cystic components as well as dense septations and/or fine internal echoes,
creating large acoustic shadows (Fig.2).
Masses are usually well-demarcated with an echogenic rim.
US can further detect associated loculated fluid collections and may also facilitate image-guided aspiration of liquefied material.
[5,
6]
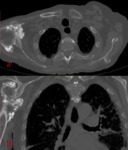
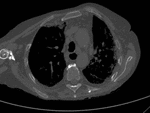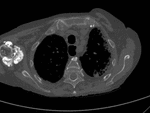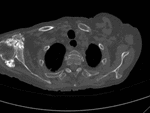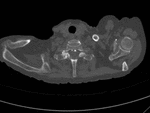
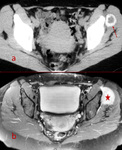
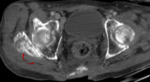
♦ CT scan is the key imaging modality for evaluating lesion size and density and assessing possible invasion into surrounding structures.
Pelvic lesions,
especially masses along the ischiogluteal or greater trochanter bursae,
are better depicted on axial images.
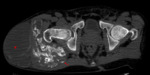
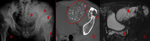
Common findings include para-articular tumorous calcifications,
appearing solid or cystic with fibrous septations,
occasionally exhibiting fluid-fluid layering,
due to the presence of a calcium-fluid interface with a pattern of “milk of calcium”,
known as the “sedimentation sign” (Fig.
3).
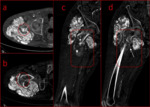
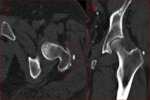
A hallmark of TC is the absence of osseous erosion by adjacent soft-tissue masses,
however intraosseous penetration has been reported,
almost exclusively in non-familial cases (Fig.4).
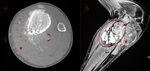
Differential diagnosis of intramedullary invasion encompasses abscess,
osteomyelitis,
chondrosarcoma (Fig.5) and other neoplasms.
[3,
4,
7]
♦ MRI appearance depends mainly on mass composition,
often presenting with interspersing areas of hyperintensity and signal void.
Lesions usually demonstrate inhomogeneous low T1-signal,
corresponding to the amount of calcium,
fibrous tissue and edema,
while fatty or hemorrhagic components may increase T1-signal intensity.
Cystic spaces containing blood or fluid,
as well as internal septations appear “bright” on T2-WI,
whereas calcified material demonstrates low T2-signal.
Fluid-fluid layering on T2-WI presents as high signal in the upper part of the cyst and decreased signal in the lower (most dependent) aspect,
owing to the calcium sediment.
Contrast-enhanced TI-WI may show peripheral wall enhancement of the cystic spaces and absence of internal enhancement,
creating an oval-shaped pattern of grape-like clusters or “chicken wire” pattern.
MRI is considered more useful in assessing the superior thoracic aperture and pelvic region,
especially the hip joints.
[4]
♦ Scintigraphy using technetium-99m-labeled phosphate compounds is valuable for depicting multiple masses and detecting new and/or active lesions.
Due to the considerable variation in imaging appearance,
other entities associated with dystrophic or metabolic periarticular soft-tissue calcifications that may confuse the differential diagnosis of TC,
mainly include:
Calcinosis universalis,
calcinosis circumscripta,
calcific tendonitis,
synovial osteochondromatosis,
synovial sarcoma,
osteosarcoma,
myositis ossificans,
tophaceous gout,
and calcific myonecrosis.
♦ PEARLS IN DIFFERENTIAL DIAGNOSIS [3]:
- Calcinosis universalis: The characteristic “sheet-like” distribution and involvement of muscle and fascial planes usually facilitates an accurate diagnosis.
- Calcinosis circumscripta: Lesions are usually less extensive than in TC,
typically located in the subcutaneous tissues rather than in the bursae.
Osseous erosion might be present,
when calcific masses are associated with rheumatic disorders.
- Calcific tendonitis: Characteristic location within a tendon and lack of sedimentation,
make this entity distinguishable from TC.
(Fig.6)
- Synovial (osteo)chondromatosis: Presence of “rings-and-arcs” calcifications, characteristic of cartilage,
intraarticular location of the lesions and related bone erosion,
are imaging features useful in differentiating this condition from TC. (Fig.7,
Fig.8)
- Synovial sarcoma: Characteristic depiction of a poorly defined and infiltrative non-calcified soft-tissue mass,
is more indicative of sarcoma than TC.
- Osteosarcoma: Presence of a non-calcified soft-tissue mass and adjacent bone involvement helps dissociate the two entities.
(Fig.9)
- Myositis ossificans: Lesion progression from mild calcification to organized cartilage/bone and lack of contour lobularity are more specific for myositis ossificans.
Late lesions (heterotopic ossification),
are discernible from TC due to their forming into bone with a distinct cortex and medullary cavity.
(Fig.10,
Fig.11)
- Tophaceous gout: Calcified tophi are typically less dense than TC and do not exhibit sedimentation.
- Calcific myonecrosis: The key imaging features promoting differentiation from TC are the intramuscular lesion location with absence of mass effect.
Despite the distinctive imaging characteristics of TC and its mimics,
there are cases with non-typical appearance that may raise doubt,
leading to erroneous or deferred diagnosis.
Biopsy is usually reserved for ambiguous cases,
mostly because of its infectious complications.
A characteristic histopathological feature is compartmentalization; clusters containing liquid chalky exudate along with calcifications.
[1]