Keywords:
Education and training, Normal variants, Education, Ultrasound, MR, CT, Musculoskeletal soft tissue, Musculoskeletal joint
Authors:
J. S. Wong, V. Cassar-Pullicino; Oswestry/UK
DOI:
10.26044/essr2019/P-0115
Imaging findings OR Procedure Details
Origin of loose bodies
- Intra-articular loose bodies can result as sequelae of a wide range of pathologies,
including osteoarthritis,
trauma,
neuropathic arthropathy and inflammation.
- These can migrate from the ankle joint into the FHL tendon sheath.
The concept of migration between compartments is established and is well-documented particularly between knee joint with popliteal cyst,
hip joint with iliopsoas bursa and more.(3,4) Floating fat in the FHL tendon sheath having migrated from the ankle joint after an intraarticular fracture has also been reported.(5)
- In our series,
all patients with loose bodies in the FHL tendon sheath have pre-existing osteoarthritic changes in the ankle joint.
Some patients also have imaging features of instability of the ankle joint,
indicating lateral ligament dysfunction.
Location – zones of FHL tendon sheath
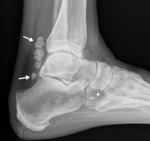
- All the loose bodies in the FHL tendon sheath in our series were present along zone 1 (behind ankle joint to sustentaculum tali),
or in zone 2 (from sustentaculum tali to knot of Henry) (Fig.
1)
- Lui had also described zone 3 of the FHL tendon sheath,
which spans from knot of Henry to its phalangeal insertion.(6) No zone 3 loose bodies have been reported in the literature to our knowledge.
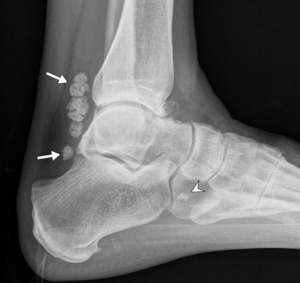
Fig. 1: Radiograph demonstrating several zone 1 loose bodies (white arrows) and a zone 2 loose body (arrowhead).
Radiographic appearances and interval change
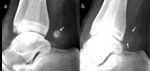
- Ossified loose bodies can demonstrate change in radiodensity on radiographs (Fig.
2).
They can change from a trabeculated structure to a lucent structure with a sclerotic rim.
This reflects presence of marrow fat which is a sign of maturation.
- Ossified loose bodies can change in size; they can either increase (Fig.
2),
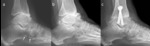
or decrease in size (Fig.
3).
- Zone 2 loose bodies are smaller than zone 1.
Zone 2 loose bodies generally measure 4 mm or less.
Loose bodies which are larger would generally be orientated longitudinally along the length of the tendon sheath (Fig.
3a,
arrow).
- In our experience,
ossified loose bodies remain in the location despite becoming smaller (Fig.
3c).
Their static location can be explained by presence of revascularisation,
which is a requirement for ossification.
MRI appearances of loose bodies
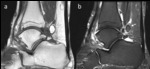
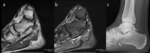
- Presence of fatty marrow in a loose body will demonstrate high T1 signal and low signal of fat-suppressed fluid sensitive signal,
as expected (Fig.
4).
- Ossified loose body with no fatty marrow will demonstrate low T1 signal and low signal on fat-suppressed fluid sensitive sequence,
and appear radiodense on radiograph or CT (Fig.
5).
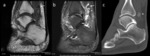
- Cartilaginous loose body will demonstrate low signal on T1 and fat-suppressed fluid sensitive sequences,
and appear unmineralised on CT or radiograph (Fig.
6).
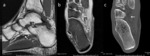
- Lipometaplasia can also occur in a truly loose body.(7) In the case of Fig.
7,
this loose body (which was not ossified on CT) demonstrates high T1 signal and heterogenous PD FS signal.
The use of ultrasound in diagnosing loose bodies
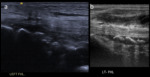
- Ultrasound can be utilised to visualise loose bodies.
Loose bodies will demonstrate focal areas of high reflectivity with posterior acoustic shadowing indicating presence of peripheral mineralisation (Fig.
8).
- Cartilaginous loose bodies can be identified as hypoechogenic structures with central area of hyperechogenicity,
reflecting internal calcification.(8)
- Understandably,
loose body visualisation will be made easier by the presence of fluid in the tendon sheath.
Pitfalls
- Loose bodies with high marrow fat content may be misinterpreted as a lipoma on MRI.
This pitfall can be avoided if there is a radiograph for comparison (correlating between Fig.
2b and Fig.
4,
same patient).
- Loose bodies in the FHL tendon sheath need to be differentiated from myositis ossificans.(9) In this instance,
we have found that appreciation of a migratory phenomenon,
together with understanding of the FHL tendon sheath anatomy will be helpful (Fig.
9).
- Misdiagnosing migratory loose bodies in the FHL tendon sheath as primary tenosynovial chondromatosis.
This has an implication on surgical management,
especially given the rare potential for malignant transformation in primary chondromatosis.