We enrolled 40 patients that underwent US guided infiltration with lithotripsy by a Philips EPIQ7 (Amsterdam,
The Netherlands) US device with a MSK default set 12-5Hz probe.
The data achieved included the amount (ml) of anesthetic and steroid drug injected and the eventually associated shoulder pathologies.
Every patient was given a Visual Analogue Scale (VAS) pain questionnaire and tested 3 weeks after the intervention.
The procedure was made up of a diagnostic step that evaluated the rotator cuff muscle and the following infiltration phases.
Pain VAS scale is one of the most common unidimensional and subjective measure of pain intensity.
It is a single-item scale self‐completed by the respondent.
The respondent is asked to indicate his painfulness from 0 (no pain) to 10 (worst imaginable pain).
Our VAS scale was supplemented with verbal descriptors to explain the significance of the score (e.g.
5 moderate pain,
but it doesn’t’ influence the routine activity) and the instruction were orally given by an operator.
(doctor or nurse).
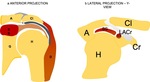
The Diagnostic phase analyzes all the muscles of rotator cuff following the ESSR checklist for a state-of-art shoulder examination.
Particularly relevance is given to Supraspinatus muscle,
which is the first site for calcifications.
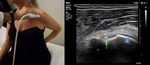
The supraspinatus (SSP) must be evaluated in “Crass position”: Placing the dorsum of the hand over the opposite back pocket to force the internal rotation and move the SSP more anterior.
We both exanimate the SSP in short and long axis with attention to its great tuberosity humeral insertion and the subacromial subdeltoid bursa (SASD).
The intervention phase is subdivided in the following steps,
performed with the patient lying on the ambulatory bed in a comfortable position to have more compliance and the operator sitting in front of his shoulder.
1. Cutaneous and probe disinfection: This phase is the most important phase in order to avoid septic complications and must be accurately performed.
We use a 70% isopropyl alcohol-based solution (IPA) plastic compatible spray for disinfecting the probe.
This act shall be carried out with gloves and sterile gauzes.
Some studies report that is as effective as using probe condom and there is a risk of infection from US transducer almost nil.
Then we disinfect the skin’s patient,
only in the area of intervention,
with Iodopovidone based antiseptic solution that need 3 minutes to perform its action and then the area is cleaned again with followed by a second cleaning with an uncolored disinfectant as alcohol ethylic.
We also recommend to equip the patient with a sterile hair cap and to isolate the interventional area with sterile pads.
Furthermore,
a sterile lubricant gel must be used to create an interface between transducer and skin’s patient.
The following operation must be performed by the first operator,
helped by nurse or second operator,
both covered with sterile gloves and mask.
2. Intrabursal and peritendinous injected anesthesia: we’d rather to inject mepivacaine chlorydrate (20mg/ml,
5-10ml max dose) which is a rapid onset and short duration local anesthetic,
considered very appropriate by Choo HJ et al for musculo-skeletal interventions.
First,
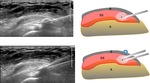
we introduce the needle in the subacromial-subdeltoidea bursa (SASD) and inject about half of the dose.
We will be sure of having it localized cause we will observe the distension of the bursa filled with liquid anechogen liquid.
Then we inject the remaining anesthetic in the subcutaneous tissue peripheral to calcification.
3. Introduction of 2 needles (16G) inside the calcification: In our institution we perform the operation with 16 Gauge Needles with flute beak tip,
that resulted suitable for every patient and to allow the calcium to flow out without obstruction.
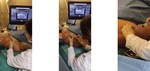
The needle must be introduced one by one with free hands,
by a single operator that holds both probe and needle and under continuous US probe supervision.
We recommend keeping the needle parallel to the probe beam to improve the visualization of all the needle.
The first needle is introduced caudal to the first to let a “free window” to localize the latter.
Afterwards the flute-beak tip of the first needle must given a rotation of 180° to create a continuous drainage pipe.
4. Lavage with saline; Saline physiologic solution must be injected at room temperature,
or,
as possible,
previously warmed (37°C) in a little oven.
Saline allows the dissolution of the calcium and we usually use an amount of about 250ml of solution.
In order to facilitate the procedure and avoid obstruction we alternate the needle we inject saline and the out-drainage needle.
Some calcifications may result very hard to be dissolved and could be helpful “needle it” rapidly piercing it more times.
Injection of low molecular weight ialuronic acid and methylprednisolone: In order to reduce local inflammation and to speed up the recover we inject in the SASD bursa 2ml of ialuronic acid and 1 ml of methylprednisolone.
This step must be also repeated 2 times after an interval of 3-4 weeks to complete a 3-injection cycle that helps to reduce bursitis and shoulder inflammation.
5. Application of a bandage,
ice and recommendation for physical therapy: Rest,
Ice and moderate compression remains the best method to recover.
Pain and range of motion limitation should get better after few days.
We also recommend the patient to consult a physiatry to assess a physiotherapy.