Keywords:
Musculoskeletal soft tissue, Musculoskeletal joint, Ultrasound, Diagnostic procedure, Treatment effects, Tissue characterisation
Authors:
T. V. Serebryak1, A. P. Trachuk2; 1Saint Petersburg /RU, 2Saint-Petersberg/RU
DOI:
10.26044/essr2019/P-0144
Results
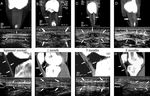
One month later all patients of the BTB group showed a thickening of the lateral and medial segments of the patellar ligament with preservation of the defect at the graft harvesting site (Fig.
6).
After 3 months,
the ligament was visualized as a whole with the restoration of the external and internal contours.
In 3 patients,
signs of inflammation in the form of moderate edema and echo-structure heterogeneity of the lateral and medial fragments with the development of tendinitis were revealed.
The regenerate was a formed scar tissue with signs of linear structure; in 3 patients anechoic zones were observed,
which testified to incomplete closure of the defect (Fig.
6).
The transverse scanning showed a ligament deformation – the «butterfly effect» due to edema and heterogeneity of the echo-structure of the lateral and medial ligament parts (18% - tendinitis).
After 6 months the deformation of the ligament is maintained by reducing the width of the defect and moderate edema of the lateral and medial parts; the regenerate is represented by an area of reduced echogenicity with a clear linear structure of collagen fibers.
Three patients (15%) had defects of the regenerate itself (Fig.
6).
In the study of bone defects after harvesting graft sites by 6 months there was a total completion of the sclerosis process in the donor area and filling the cavity with a mature scar tissue (Fig.
7).
In the ST group,
1 month after the operation,
all patients have retraction and violation of the structure of the belly of semitendinosus femur muscle (Fig.
8).
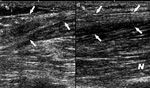
At the site of the anatomical location of the tendon of the femur semitendinosus muscle between the sheets of the superficial and deep fascia in 87% of the patients a 2 times thickened (in comparison with the contralateral side) hypo-echogenic formation with fuzzy edges (organized hematoma) was visualized (Fig.
9 A,
B).
After 3 months,
the donor site was represented by a regenerate ("neotendon") – a wide band of immature scar tissue reaching the articular slit of the knee joint.
The scar tissue was not visualized in 2 patients (Fig.
9 C,
D).
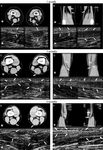
After 6 months,
the defect from the tendon-muscular part to the level of the knee joint in 87% of patients was filled with a mature scar tissue resembling the tendon structure.
The regenerate thickened twice as much as the opposite side (Fig.
9 E,
F).
In 2 patients,
no regeneration was observed,
and the maternal bed was represented by an uneven,
thick contour of "stuck together" sheets of the surface and deep fascia (Fig.
10).