The inflammatory arthritides,
of which rheumatoid arthritis (RA) is the most common,
are a group of chronic,
often debilitating,
disorders characterized by synovial inflammation and progressive joint destruction.
Early inflammatory arthritis may develop into established RA or another form of arthropathy,
may spontaneously resolve,
or may remain undifferentiated.
Common US findings in rheumatologic diseases – terms and definitions
The Outcome Measures in Rheumatoid Arthritis Clinical Trials (OMERACT) has standardized the imaging thecnique and defined the most common pathologic US findings of rheumatologic diseases in clinical daily practice and research:
Bone erosion
Defined as a discontinuity of the bone surface that is visible in two perpendicular planes ( Fig. 1 Fig. 2 Fig. 3 ).
Articular erosions can be scored by size criteria (small ≤ 2 mm,
moderate 2 - 4 mm,
large ≥ 4 mm).
US can depict early articular erosions,
before they become evident in conventional radiograph studies.
However,
owing to the anatomic disposition of digits,
there are some areas with poor US accessibility: carpal and tarsal joints,
radial and ulnar sides of the third and fourth metacarpophalangeal (MCP) joints,
radial side of the fitfth MCP joint,
ulnar side of the second MCP joint,
second,
third,
and fourth metatarsophalangeal (MTP) joints.
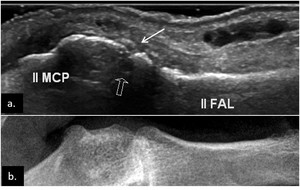
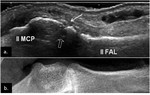
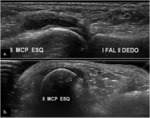
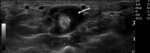
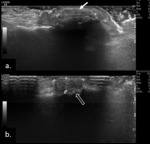
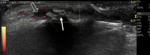
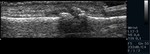
Fig. 1: Small bone erosion (arrow) of the 2nd MCP joint in a RA patient, seen on US image (a.) as a discontinuity of the bone surface (arrow), not depicted on the plain radiograph. Also note the small subchondral cyst (open arrow).
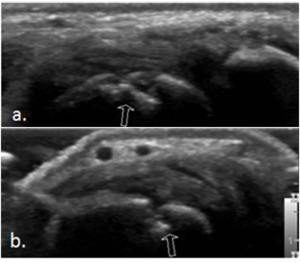
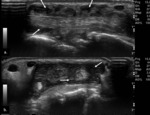
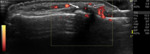
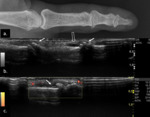
Fig. 2: Small bone erosion on US-images (open arrows) seen as a discontinuity of the bone surface visible in two perpendicular planes (a.) and (b.)
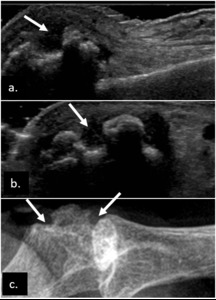
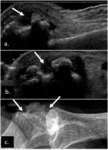
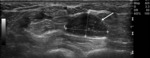
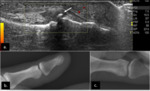
Fig. 3: Bone erosions (arrows) of the 3rd MCP joint in a RA patient. Longitudinal (a.) and transverse (b.) plane US image. Plain radiograph of the same joint (c.).
Tenosynovitis
Abnormal anechoic or hypoechoic material within the tendon sheath,
that can be related either to fluid or synovial hypertrophy.
It can be further characterized by color Doppler,
which allows the detection of increased vascularization within the tendon synovial sheath Fig. 4 .
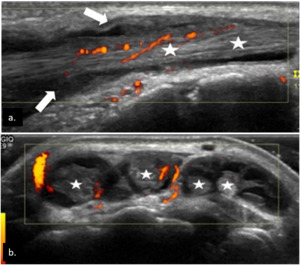
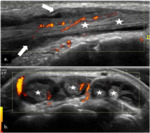
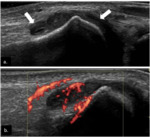
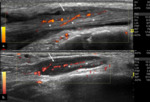
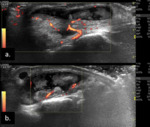
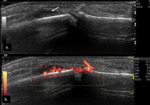
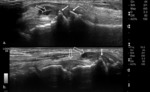
Fig. 4: Tenosynovitis depicted by hypoechoic material (arrows) within the tendon sheaths (stars) on longitudinal plane (a) and transverse plane, associated with Doppler signal on power-Doppler (b.).
Enthesitis
Thickening,
with hypoechogenecity,
of the attachment of ligaments or tendons to bone.
The presence of color Doppler signal is a marker of active inflammation.
Joint effusion
Abnormal hypoechoic or anechoic intra-articular,
displaceable and compressible material,
that does not exhibit color Doppler signal Fig. 5 .
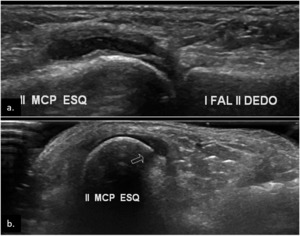
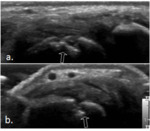
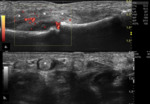
Fig. 5: Joint effusion (arrow) of the 2nd MCP joint. Longitudinal (a.) and transverse (b.) plane US image shows anechoic, compressible, intra-articular material.
Also note small bone erosion depicted on image b. (open arrow).
Synovitis
Synovial hypertrophy,
seen as an abnormal hypoechoic,
intraarticular,
nondisplaceable and poorly compressible tissue that may or may not exhibit color Doppler signal Fig. 8 .
The presence of Doppler signal in the synovial tissues at color Doppler or power Doppler US indicates hyperemia and implies active inflammation.
Therefore,
US examination allows differentiation between the joint effusion and active or inactive synovial proliferation.
The EULAR/OMERACT group for musculoskeletal US has agreed on the use of a four-grade semiquantitative scoring system for synovitis for both B-mode US and Power-Doppler detected synovitis,
that have demonstrated good intra- and inter-observer reliability in RA patients.
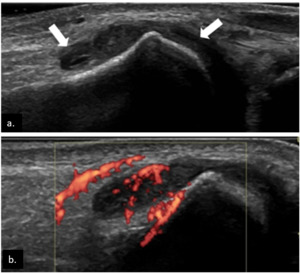
Fig. 8
Synovitis – B-mode/Gray scale US Fig. 6
0 = normal (no synovial thickening)
1 = mild (minimal synovial thickening filling the angle between the articular bone surfaces,
without bulging over the interarticular line)
2 = moderate (synovial thickening bulging over the interarticular line,
but without extension along the bone diaphysis)
3 = marked (synovial thickening bulging over the interarticular line,
with extension to at least one of the bone diaphysis)
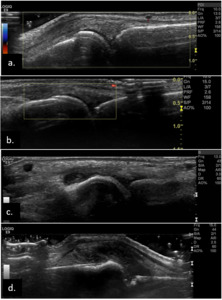
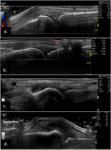
Fig. 6: EULAR/OMERACT group four-grade semiquantitative scoring system for synovitis in gray-scale: (a.) 0 = normal (no synovial thickening ), (b.)
1 = mild synovial thickening , (c.) 2 = moderate synovial thickening and (d.) 3 = marked synovial thickening.
Synovitis – Power-Doppler
0 = normal (no flow in the synovium)
1 = mild (single vessel or up to 3 spot signals in the affected area)
2 = moderate (confluent vessel signals in less than half of the area of the synovium)
3 = marked (vessel signals in more than half of the area of the synovium)
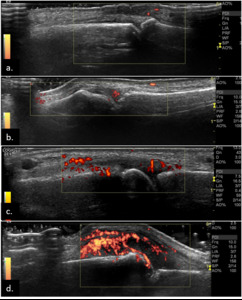
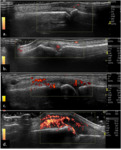
Fig. 7: EULAR/OMERACT group four-grade semiquantitative scoring system for synovitis in power-Doppler: (a.) 0 = normal (no flow in the synovium), ), (b.) 1 = mild signal, (c.) 2 = moderate signal (<50 % of the synovium) (d.) 3 = marked signal (>50 % of the synovium).
Rheumatoid Arthritis (RA)
RA is a chronic progressive systemic inflammatory disease characterized by persistent,
usually symmetric,
polyarthritis.
It affects approximately 1% of the adult population,
increasing with age and peaking at 45 - 65 years.
It is 2 to 3 times more common in women.
The hallmark feature of this condition is synovial inflammation,
affecting any of the synovial joints as well as tendon sheaths.
In the course of the disease,
adjacent structures such as bones,
tendons,
bursae and ligaments can be involved.
Over the last 20 years,
the prognosis of RA has been significantly improved with the introduction of new disease-modifying antirheumatic drugs (DMARDs) and biologic therapies and the generalized use of standardized guidelines for evaluation of disease activity including the American College of Rheumatology (ACR) and EULAR 2010 criteria.
There is now a substantial body of evidence to support the very early use of agressive therapies such as anti-TNF agents and IL-1 inhibitors,
preferably before the first radiographic evidence of erosions,
to prevent subsequent joint destruction and disability.
High-resolution US,
alongside with MR imaging,
have demonstrated greater sensitivity in detecting synovitis and articular erosions when compared to either clinical examination or conventional radiography,
theferefore it is considered a useful tool in establishing an early diagnosis of RA (<12 months duration) and/or in undifferentiated (with normal radiographic findings) arthritis.
Furthermore,
patient’s response to treatment can be assessed by monitoring the degree of synovial thickening and hyperemia.
Imaging findings in RA
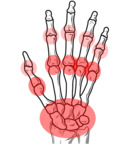
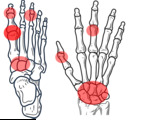
A bilateral and symmetric disease distribution with involvement of the small joints of the hands and feet is characteristic of most RA patients,
with predominant involvement of the metacarpophalangeal (MCP) joints,
proximal interphalangeal (PIP) joints,
and wrist.
The metatarsophalangeal (MTP) joints are also frequently implicated.
Involvement of large joints (knees,
ankles,
elbows,
hips,
and shoulders) although common,
often occurs later in the course of the disease.
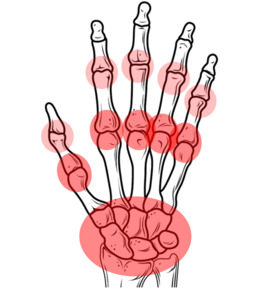
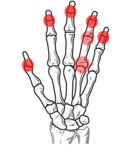
Fig. 9: RA: Usual pattern of joint involvement in the hands and wrists
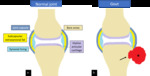
Synovial inflammation and proliferation is the primary pathologic process,
resulting in marginal erosions at the “bare areas” of the involved joints.
Cartilage loss further results in symmetric joint space narrowing.
Long-term disease progression leads to fibrous and osseous ankylosis,
as well as ligamentous laxity and ruptures,
with subluxations and dislocations of the affected joints.
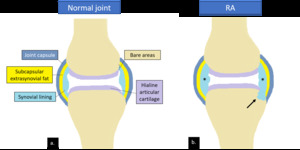
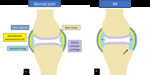
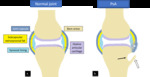
Fig. 10: Drawings of a normal synovial joint (a) and a synovial joint with RA-associated synovitis (*) and erosive change (arrow) in (b).
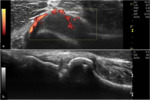
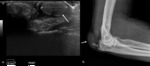
Synovitis (Fig. 11) occurs early in the natural history of RA and is considered a strong predictor of bone erosion development.
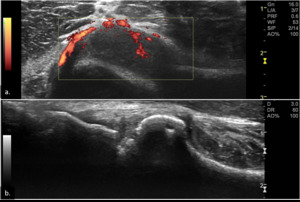
Fig. 11: Transverse PD US scan of the anterior recess of the elbow (a) shows synovial proliferation with positive PD signal, indicating active inflammation. In a lateral approach to the same joint, gray-scale US scan (b) depicts bone erosion
US may also be used to identify soft-tissue rheumatoid nodules,
which usually demonstrate heterogeneous echogenicity.
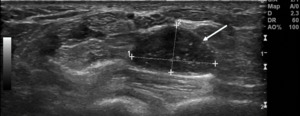
Fig. 16: Rheumatoid nodule in a patient with known RA. Long-axis gray-scale US image at the dorsal aspect of wrist shows a heterogeneous nodular mass (arrows), consistent with a rheumatoid nodule.
The major disadvantage of high-resolution US with respect to MR imaging is the inability to “see” beyond the bone surface and to diagnose bone marrow edema,
which is known to be an important prognostic indication for disease progression.
Crystalline Arthropathies
Crystal deposit diseases are a group of methabolic disorders characterized by the intra and extra-articular deposition of crystals.
Monosodium urate (MSU) crystals as a consequence of raised serum uric acid levels in gout,
and calcium pyrophosphate dihydrate (CPPD) crystals in pseudogout,
are the most common forms.
Gout affects 1%–2% of the population and represents the most prevalent form of metabolic arthritis in men,
affecting particularly older men. Gout is a disorder of purine metabolism and results from MSU crystal deposition in and around the joints,
particularly in the peripheral joints,
periarticular soft tissues and tendons.
Only about 10 % of hyperuricemic individuals with cumulative crystal deposition will develop clinical manifestations of gout disease,
with recurrent acute arthritis that may lead to chronic arthropathy,
tophus deposition,
and renal disease.
CPPD is a metabolic arthropathy characterized by deposition of calcium pyrophosphate dihydrate crystals in the articular and periarticular tissues,
that clinically mimics a gout attack.
Chondrocalcinosis is a pathologic and radiographic term denoting the presence of intra-articular calcifications with involvement of the hyaline articular cartilage and fibrocartilage.
CPPD can be classified as sporadic,
hereditary,
or secondary.
The sporadic idiopathic forms occur in middle-aged or elderly patients with equal frequency in men and women.
Hereditary forms are more frequent in women and commonly result in more severe arthropathy.
Imaging findings in Gout and CPPD
Crystal-induced tissue reaction in gout is different from that of inflammatory arthritis,
where synovial inflammation is thought to be the primary cause of tissue damage.
Nonetheless variable degrees of synovitis with associated hyperemia at power Doppler US may be associated with crystalline arthropathies ( Fig. 17 ).
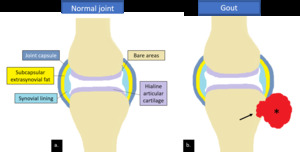
Fig. 17: Drawings of a normal synovial joint (a.) and a synovial joint in gouty arthropathy (b.) which shows para-articular tophus (*) eroding into the adjacent bone (arrow).
In the majority of cases,
gouty arthropathy begins in the lower limb joints (85%–90% of cases),
involving the first MTP joint,
where it is termed podagra.
The other frequent locations are the tarsal joints,
ankles,
and knees.
With disease progression it tends to also involve the elbows and hands ( Fig. 23 ).
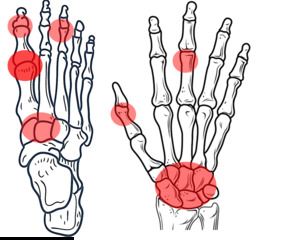
Fig. 23: Gout: Tipically involves the first MTP joint. Other frequent locations are the tarsal joints, and to a lesser degree the interphalangeal. In the hands, there is not a typical pattern, however the carpal joints tend to be involved.
Distended joints have a variable appearance,
ranging from simple homogeneously anechoic synovial fluid to heterogeneously hyperechoic synovial-fluid complexes containing numerous mobile hyperechoic stippled aggregates,
which create a snowstorm appearance.
Echogenic intra-articular aggregates are also seen in CPPD arthropathy.
In gout,
MSU crystals deposit on the surface of the hyaline articular cartilage,
resulting in the US appearance of a hyperechoic line at the outer margin of the cartilage,
termed the double-contour cartilage line ( Fig. 20 ).
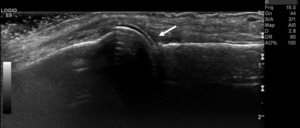
Fig. 20: Double contour sign in gouty arthropathy: Gray-scale US scan of the 2nd MCP joint shows intra-articular hyperechoic cartilage line (arrow) related to urate acid crystal deposition, which is also characterized by angle of insonation independency (not demonstrated).
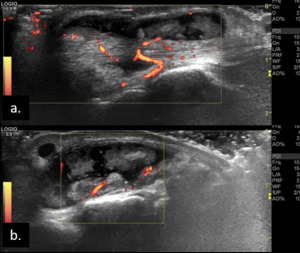
Fig. 22: Longitudinal (a) and transverse (b) US scans show tenosynovitis of the fourth extensor compartment
in a patient with gouty arthropathy
Thirty percent of untreated patients develop tophaceous gout within 5 years,
characterized by painless soft-tissue masses composed of MSU crystals,
most often seen as a heterogeneous masses with intermittent hyperechoic foci (allowing the differentiation from rheumatoid nodules which are more homogeneous) and peripheral hypo- or anechoic halo ( Fig. 18 ) .
Tophi can occur anywhere throughout the musculoskeletal system,
frequently developing about joints,
tendons,
and bursae.
Typical tendon targets include the Achilles tendon,
knee extensor mechanism,
popliteal tendon and the olecranon region at the elbow.
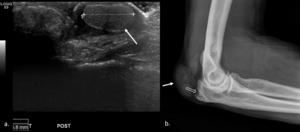
Fig. 18: Gray-scale US image (a.) at the dorsal aspect of the olecraneon shows a large nodular echogenic mass, with surrounding anechoic halo (arrows) consistent with tophaceous gout. Corresponding plain radiograph shows tophaceous gout (arrow) with erosive changes on the olecraneon surface (open arrow).
At US,
gouty erosions may appear deeper and more destructive when compared with erosive changes in RA ( Fig. 19 ).
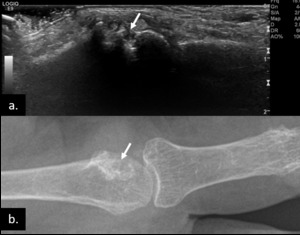
Fig. 19: Gray-scale US scan of the 2nd MCP joint (a.) and corresponding plain radiograph (b.) in patient with gout disease, shows erosive bone changes (arrows), with sclerotic borders in (b.).
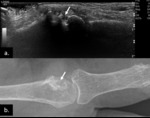
Extra-articular tophaceous bone deposits are associated with destructive bone changes with areas of cortical disruption,
which can also be seen at US ( Fig. 21 ).
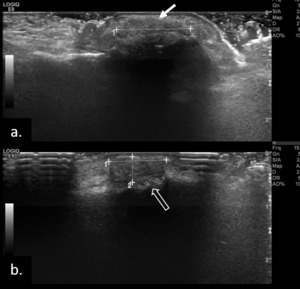
Fig. 21: Gray-scale US scan of the DIP joint of the 5th (a) and 4th (b) digits showing heterogeneous nodular material consistente with tophaceous gout (arrows). Note the associated erosive bone changes in b (open arrow).
The most common sites of involvement of CPPD include the knee,
wrist,
hand,
pubic symphysis and hip joints.
The ankles and feet are infrequently involved.
In the wrist,
chondrocalcinosis is typically seen in the triangular fibrocartilage and about the proximal carpal row joints in the region of the lunotriquetral and scapholunate ligaments.
In the hand,
there is a predilection for involvement of the second and third MCP joints with chondrocalcinosis and frequently associated advanced degenerative changes.
The other MCP and hand interphalangeal joints are infrequently involved.
In contrast to gout,
in CPPD disease,
calcium pyrophosphate crystals tend to form aggregates within the hialine cartilage rather than on the surface,
and appear as hyperechoic irregular and dotted line embedded in the anechoic-appearing hyaline cartilage.
This intra-articular crystal deposition in CPPD predisposes to cartilage degeneration and development of osteoarthritis.
In addition,
calcium pyrophosphate crystals deposit in the fibrocartilage,
such as the triangular fibrocartilage of the wrist and menisci,
and appear as round or amorphous hyperechoic foci.
Psoriatic arthritis
Psoriasis is a cutaneous disease that affects approximately 1%–2% of the population,
while Psoriatic arthritis (PsA) is an inflammatory arthritis occurring in 10%–15% of people with psoriasis,
that can take place at the same time or precede skin disease.
The usual age of onset is 30–50 years,
and it is equally common in men and women.
Psoriatic arthritis (PsA) belongs to the family of seronegative spondyloarthropathies that share common clinical and laboratory features,
including association with HLA-B27 positivity and entheseal disease with secondary joint involvement ( Fig. 24 ).
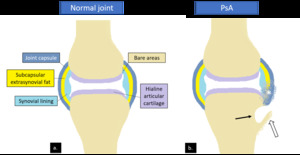
Fig. 24: Drawings of a normal synovial joint (a) and a synovial joint in PsA (b.) which shows indistinctness of the enthesis at the capsular attachment site (*) consistent with enthesitis, with associated para-articular erosion (arrow) and proliferative new bone formation (open arrow).
The hallmark of PsA,
and that distinguishes PsA from RA,
is the combination of erosive change with bone proliferation.
PsA may manifest in various forms from monoarthritis to polyarthritis,
and as mild to severely destructive disease (arthritis mutilans).
Imaging findings in PsA
The asymmetric joint distribution helps in the differentiating PsA from the typically bilaterally symmetric RA,
as well as the predominance of synovitis in DIP joints compared with that in RA patients,
which is tipically more proximal ( Fig. 25 ).
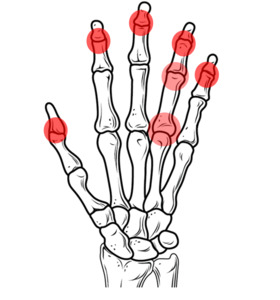
Fig. 25: PsA: Usual pattern of joint involvement in the hands, with predominance of synovitis in DIP.
There are several nonspecific US findings in peripheral joints in PsA that may also occur in patients with other inflammatory arthropathies,
including synovitis,
joint effusion,
and bone erosions,
as well as extra-articular findings such as bursitis,
tenosynovitis and enthesitis.
Flexor tendon tenosynovitis is the most common pathologic process associated with dactylitis or sausage digit ( Fig. 29 ).
US reveals a characteristic nodular/irregular appearance of the tendon sheath,
with associated increased tenosynovial fluid and solid hyperemic nodules at power Doppler US.
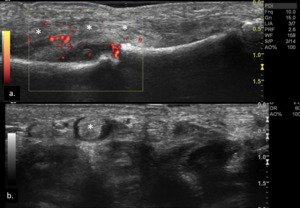
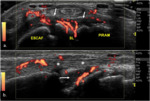
Fig. 29: Dactylitis in a patient with PsA: longitudinal power-Doppler US (a) and transverse gray-scale US (b) scans of the volar aspect of 4th digit, shows thickening of the flexor tendon sheath (*) with associated hyperemia (Doppler signal), consistent with flexor tendon tenosynovitis, resulting in the clinical appearance of sausage digit.
Symptomatic enthesitis is seen in up to 40% of patients with PsA,
corresponding to hypoechoic entheseal thickening,
with hyperemia ( Fig. 27 and Fig. 28 ).
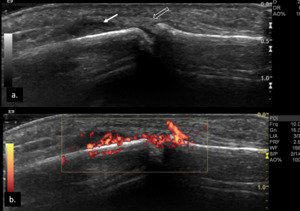
Fig. 27: Longitudinal gray-scale US (a) and Power-Doppler US (b) scans of the 4th DIP in a patient with PsA, shows synovial hypertrophy (arrows) and thickening of the enthesis (open arrow) with hyperemia (Power-Doppler signal).
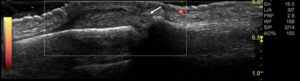
Fig. 28: Gray-scale and power-Doppler US scan of the 2nd PIP joint of patiente with PsA, shows thickening of the extensor tendon and its enthesis (arrow), consistent with enthesistis, without Doppler signal.
Different scoring systems have also been suggested for enthesisitis,
however,
a recent systematic literature review by the OMERACT Ultrasound Task Force concluded that there remains a lack of consensus of how to define and score enthesitis.
Because bone proliferation of psoriatic arthritis may at times appear similar to other forms of bone proliferation,
such as osteophytes in degenerative joint disease,
it is critical to correlate the ultrasound finding with radiographic studies,
which can assist in this distinction.
The presence of hyperemia,
often seen in psoriatic arthritis,
is another distinguishing feature ( Fig. 26 and Fig. 30 ).
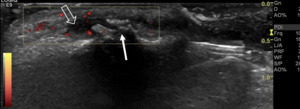
Fig. 26: Gray-scale and power-Doppler US scan of the 3rd DIP joint, shows proliferative bone changes (arrows) and synovitis (open arrow) with mild active inflammation (Doppler signal), in a patient with PsA.
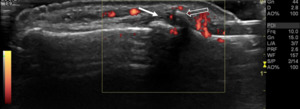
Fig. 30: Gray-scale and power-Doppler US scan of the 2nd DIP joint, shows proliferative bone changes (open arrow) with hyperemia (arrow) at the enthesis, in a patient with PsA.
Osteoarthritis
An extensive description of osteoarthritis US findings is beyond the scope of this poster,
however we consider it to be an important differential diagnosis of inflammatory and metabolic arthropathies due to it’s high prevalence and the overlap of clinical and US findings.
Osteoarthritis diagnosis is usually made based on clinical findings and radiographs,
especially in advanced stages.
MR imaging is superior to US,
as it allows complete visualization of articular cartilage and can depict bone marrow edema.
The hallmark of osteoarthritis is cartilage loss and osteophyte formation.
Synovial hypertrophy is often relatively mild,
with hypoechoic,
minimally compressible tissue distending the joints,
such us the interphalangeal joints of the hands.
In contrast to other arthropathies,
increased flow on power-Doppler is uncommon,
and the presence of synovial hypertrophy does not necessarily correlate with patients symptoms.
Osteophytes appear as a well-defined bone excrescence at the margins of the involved joints.
Joint effusion may also be present ( Fig. 31,
Fig. 32,
Fig. 33 and Fig. 34 ).
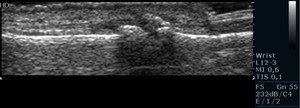
Fig. 31: Gray-scale US scan of the 2nd DIP joint, shows joint space narrowing and marginal osteophytes, as well as absence of synovial hypertrophy, in a patient with osteoarthritis.
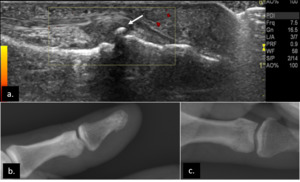
Fig. 32: Gray-scale US scan of the 1st IP joint (a) shows mild synovial hypertrophy without active inflammation (no Doppler sign) and marginal osteophytes (arrow), consistent with osteoarthritis. Note that in the correspondent radiographs (b and c) the osteophytes are not yet perceptible
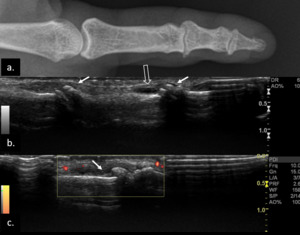
Fig. 33: Radiograph of the first digit (a) shows signs of osteoarthritis of the PIP and DIP - joint space narrowing and marginal osteophytes. Gray-scale US scan of the same joints (b and c) clearly depicts the marginal osteophytes (arrows) and also demonstrates mild synovial hypertrophy and joint fluid (open arrow) without active inflammation (no Doppler sign).
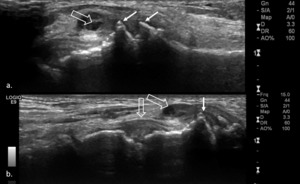
Fig. 34: Gray-scale US scan of the intertarsal (b) and tarsometatarsal joints (a and b) shows synovial hypertrophy (open arrows) and marginal osteophytes of the tarsometatarsal joint (arrows), consistent with osteoarthritis.
Common sites of involvement include the first metatarsophalangeal joint,
the interphalangeal and first carpometacarpal joints of the hand and wrist and the acromioclavicular joint.
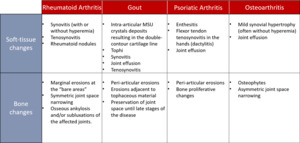
Fig. 35: Table 1 – Summary of the most common US findings in RA, Gout, PsA and Osteoarthritis. MSU = Monosodium urate