A total of 1319 consecutive CTPA studies were performed during the study period,
yielding a total of 202 positive studies (110 male,
92 female) for further analysis.
The rate of positive studies was 15.3%.
The cohort comprised subjects from emergency,
inpatient and outpatient settings.
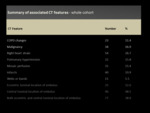
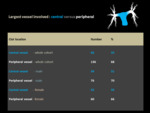
A summary of associated CT features are presented in Table 1 .
The mean age of patients included in the study was 59.4 years (median 61,
range 18 – 97).
Twenty-three patients (11.4%) demonstrated CT changes of established COPD.
Thirty-four patients (16.9%) had a history of malignancy from imaging records.
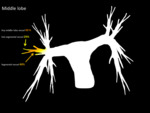
Emboli were most likely to involve the right lower lobe, occurring in 162 patients (80.2%) ( Fig. 3 ).
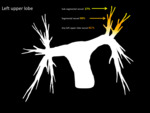
Emboli were least likely to involve the left upper lobe,
occurring in only 84 patients (41.6%) ( Fig. 6 ).
Sixty-six patients (32.7%) had central pulmonary emboli ( Table 2 ).
Only 9 patients (4.5%) had pulmonary emboli limited to subsegmental arteries.
One-hundred-and-eighty-one patients (89.6%) demonstrated right-sided emboli and 144 (71.3%) demonstrated left-sided emboli,
noting 123 patients (60.9%) with bilateral emboli.
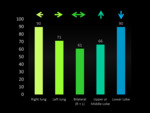
While 181 patients (89.6%) demonstrated lower lobe emboli,
only 134 patients (66.3%) demonstrated upper and/or middle lobe emboli ( Fig. 9 ).
Both the right-sided and lower-lobe trends were present in the male and female cohorts.
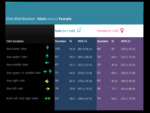
No statistically significant difference was demonstrated between males and females in terms of location of vessel involvement ( Table 3 ).
In patients with a history of malignancy,
the highest frequency was found in the left lower lobe,
followed closely by the right lower lobe.
There was no statistically significant difference in emboli location demonstrated in patients with either CT established COPD changes ( Table 4 ) or imaging evidence of malignancy ( Table 5 ),
and those without,
however,
subgroup analysis was limited by the low numbers of patients with such features.
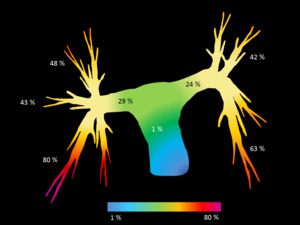
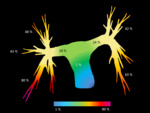
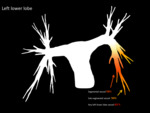
Fig. 2: Diagramatic representation of the percentage prevalence of emboli within the pulmonary arterial system. The shaded pulmonary arterial map uses a graded colour scale from blue (areas of lowest embolic burden) to purple (areas of highest embolic burden).
References: Yuranga Weerakkody
Discussion
The data from our institution demonstrated a 15.3% positive CTPA rate, comparable to a large study of 7077 subjects by Mountain et al which reported a 14.6% positive CTPA rate in Western Australian emergency patients.4 Our study’s population,
however,
included not only emergency patients but also subjects from inpatient and outpatient populations.
Overall,
the highest frequency of emboli occurred in the right lower lobe.
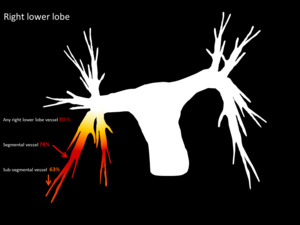
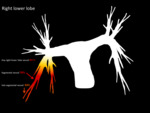
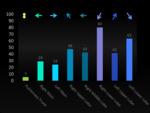
Fig. 3: Segmental and subsegmantal distribution of embolic burden in right lower lobe pulmonary arteries
References: Yuranga Weerakkody
It is interesting to note that this is the same region in which aspiration may preference and perhaps is a reflection of bronchovascular orientation.
This finding is concordant with the right-sided predominance reported by Deng et al who in their study of 149 emergency patients with positive CTPA studies reported 89.7% of patients with emboli within the right lung.5 This finding was reportedly significantly higher than that found in the left lung (42.6%).5 Deng et al also found the proportion of patients with pulmonary emboli within the right lung was significantly higher in the male cohort than in the female cohort.5 This trend was not observed in our study,
with no statistically significant gender difference demonstrated in terms of location of emboli.
Only a very small proportion (4.5%) of patients in our cohort had pulmonary emboli isolated to subsegmental arteries,
for which there is current controversy with regards to the appropriateness of anticoagulant treatment.3
Within the subset of patients with CT established COPD changes,
the highest frequency of emboli occurred in the right lower lobe.
The subset of COPD patients counted in this study may be an underestimate given that visible established architectural changes of COPD are a late sign of the disease.
Although the number included in this sample is small and therefore underpowered to demonstrate small statistically significant differences from the cohort without CT established COPD changes,
the predilection for emboli to occur in the right lower lobe may be intuitive. There is an altered distribution of ventilation/perfusion ratios due to the pathological changes that occur in COPD.1 With preferential upper zone architectural destruction in COPD it is postulated that this may result in greater perfusion of the lower lobes.
Therefore,
it is conceivable that pulmonary emboli may be more prevalent within the lower lobes in those with established COPD changes compared to patients without established changes.
In patients with a history of malignancy,
the highest frequency was found in the left lower lobe,
closely followed by the right lower lobe.
Haematogenous metastases are known to have a lower lobe predominance,
perhaps a similar mechanism may account for this finding with pulmonary emboli.
Noting also there may be a subset of patients within this group who have tumour thrombus.