Introduction
- Fungal infection may occur in any immunocompromised patients.
- It occurs most commonly in patients undergoing aggressive chemotherapy and hematopoietic stem cell transplantation (HSCT).
It is seen in 12-45% of cases of pneumonia occurring in patients with HSCT
Pathogens
- The frequent pathogens are Aspergillus fumigatus and Candida albicans,
especially,
about 60 % of fungal infections in the immunocompromised patients is due to Aspergillus infection.
Common radiologic findings
- n Fungal infection usually shows nodules or masses.
- Mori et al.
reported that,
among 21 patients of fungal infection occurring in bone marrow transplant patients,
17 cases and 20 cases showed nodular opacities in chest radiograph and CT,
respectively [1].
Pulmonary Aspergillosis
Aspergillosis is a mycotic disease caused by Aspergillus species,
especially A.
fumigatus.
- The patterns of pulmonary aspergillosis are mainly determined by the patient’s immune status.
- Furthermore,
more than one form of aspergillosis can sometimes co-exist.
- Aspergillus species tend to colonize cavities in the lung; especially local host defenses are impaired.
- Quantitative or qualitative neutrophil impairment can allow hyphal growth and tissue invasion.
Patterns of pulmonary aspergillosis
- Aspergilloma (almost normal immune system condition)
- Allergic aspergillosis (normal immune system condition)
- ABPA
- Hypersensitivity pneumonitis
- Semi-invasive aspergillosis (moderate immune suppression)
- Invasive (marked immune suppression)
- Acute tracheobronchitis
- Airway-invasive aspergillosis
- Angio-invasive aspergillosis
Aspergilloma
- Aspergilloma is characterized by Aspergillus infection without tissue invasion.
Etiology
- The most common underlying causes are tuberculous and sarcoidosis,
however,
any cavitary lesions within the lung may be a potential focus for the development of aspergilloma.
- It is reported that 11-20% of tuberculous patients with cavities of 2.5 cm or greater in size had radiographic evidence of aspergilloma [2].
- It is also reported that up to 53% of patients with sarcoidosis was supposed to have radiological evidence of aspergilloma [3].
Mechanisms of aspergilloma formation
- Initially,
pleural or cavitary wall thickening occurs,
followed by the protrusion of the cavitary wall into the cavities,
breaking away from the cavitary wall to form a fungus ball.
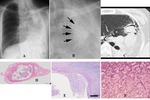
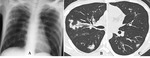
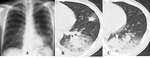
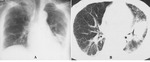
Chest radiographic findings
- Rounded mass within the cavity usually with thickened wall.
- Typically,
the mass is separated from the cavitary wall by an crescent-like airspace,
resulting in the “air crescent sign” or “Monad sign”(Fig.
1A and B).
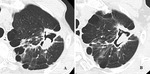
HRCT findings
- CT is superior to chest radiography in demonstrating the mobility of the intracavitary mass after a position change of a patient and in the detection of the foci of increased attenuation within the mass which reflects calcium (Fig.
1C and Fig.
2).
Semi-invasive aspergillosis (Chronic necrotizing aspergillosis)
- Semi-invasive aspergillosis is characterized histologically by the presence of tissue necrosis and granulomatous inflammation similar to that seen in reactivation tuberculosis
Etiology
- Conditions associated with the development of this entity include diabetes mellitus,
alcoholism,
malnutrition,
advanced age,
prolonged steroid therapy,
tuberculosis,
collagen vascular diseases,
pneumoconiosis and chronic obstructive pulmonary diseases.
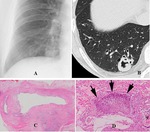
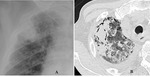
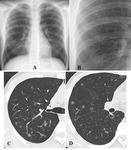
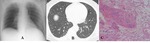
Radiographic findings
- Frequent findings include upper lobe-predominant consolidation and pleural thickening,
which slowly progresses to cavitation over weeks to several months or years.
The cavity often resembles that of aspergilloma or pulmonary tuberculosis (Fig.
3A and 4A).
HRCT findings
- Frequent CT findings include irregular upper lobe consolidation that slowly progresses to cavitation (Fig.
3B and 4B).
CT can sometimes depict high attenuation material (calcium) within the opacity.
The existence of this high attenuation material is characteristic of Aspergillus infection.
Invasive pulmonary aspergillosis (IPA)
- Invasive pulmonary aspergillosis (IPA) is characterized by tissue invasion by Aspergillus organisms,
usually accompanied by tissue destruction.
Aspergillus hyphae firstly invade the bronchial wall and subsequently the accompanying arteries or arterioles.
- Invasive aspergillosis includes two main forms; airway invasive aspergillosis (airway-IPA) (Fig.
5 and 6) and angioinvasive (angio-IPA) (Fig.
7 and 8) and Due to the anatomic proximity of the bronchi and arteries,
it is not surprising that these two forms co-exist in the same patient and it is often difficult to distinguish between the two types (Fig.
9).
- According to the report of Althoff Souza,
et al.,
the frequency of airway-IPA among all IPA accounts for 44%,
angio-IPA 25%,
and co-existence of two forms 31% [4].
Therefore,
airway-IPA ends up accounting for 75% of IPA patients,
which shows that the frequency of airway-IPA is more frequent than has been reported.
- Invasive aspergillosis occurs almost exclusively in severely immunocompromised patients,
especially those with neutropenia,
after hematopoietic stem cell transplantation,
solid organ transplantation,
intensive chemotherapy,
and patients with AIDS.
- The risk for infection increases when WBC count is less than 1000/mm3.
- Mortality rate may be around 40% when treated immediately,
however,
it will rise up to 90% when the treatment starts after more than 10 days.
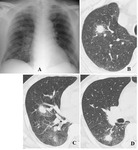
Airway-invasive aspergillosis (airway-IPA)
- The pathological definition of airway invasive aspergillosis is the presence of Aspergillus organisms deep to the basement membrane of the airways.
- Airway-IPA is identical to Aspergillus bronchopneumonia.
Chest radiographic finding
- It is nonspecific,
and frequent findings include patchy consolidation or ill-defined nodules (Fig.
5A and 6A).
Sometimes no abnormal finding is seen.
HRCT findings
- CT findings may show small centrilobular nodules,
tree-in-bud pattern,
and peribronchial airspace consolidation,
which reflect the pathological findings of bronchopneumonia (Fig.
5B,
5C,
6B,
and 6C).
- These CT findings are non-specific,
and it is difficult to differentiate this entity from other infectious diseases.
Angioinvasive Pulmonary Aspergillosis(angio-IPA)
- Angio-IPA is characterized histologically by invasion and occlusion of small to medium-sized pulmonary arteries by Aspergillus hyphae,
which causes hemorrhagic infarction: central necrosis and surrounding hemorrhage (“target lesion”).
It also causes pleural based wedge-shaped infarction.
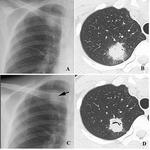
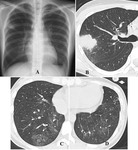
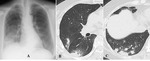
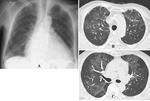
Chest radiographic findings
- Frequent findings are solitary or multiple nodules or masses (Fig.
7A and 8A).
- It should be noted that up to 10% of patients with IPA show normal chest radiograph.
HRCT findings
- The characteristic CT findings in the early phase include nodules surrounded by a halo of GGO (“CT-halo sign”) or pleural based wedge-shaped opacities (Fig.
7B,
7C,
7D,
and 8B).
- CT halo sign is no longer a characteristic finding for only aspergillosis and may also be seen in other entities,
including candidiasis,
viral pneumonia,
Wegener’s granulomatosis,
lymphoma,
and hemorrhagic metastasis,
however,
it is still an important finding as an early sign of IPA.
- In the later phase (2-3 weeks after the onset),
separation of necrotic center from adjacent lung parenchyma results in crescent-like airspace (“air crescent sign”) which is similar to that seen in aspergilloma,
due to the recovery from neutropenia (Fig.
8C and 8D).
- Nodules with air crescent sign are more characteristic for IPA than CT-halo sign.
- These two signs are supposed to be hallmarks of good prognosis.
CT-halo sign and Air crescent sign: the association with the prognosis
CT-halo sign
- Patients with a halo sign,
in the initial examination,
had significantly better responses to treatment and greater survival than patients who had other imaging findings,
including consolidations,
infarct-shaped nodules,
cavitary lesions,
and air-crescent signs [5].
Air crescent sign
- One report showed that patients with air crescent sign showed significantly better prognosis (survival rate 67%) than those without this sign (survival rate 8%).
This sign does not appear in patients without a recovery of white blood cell count from neutropenia [6].
- This sign usually appears 2-3 weeks after CT-halo sign; therefore,
it is not important as an early sign,
but a good indicator of the prognosis.
The differentiation of IPA from bacterial pneumonia in patients with neutropenia
- In the report of Bruno et al,
who compared the HRCT findings of IPA with those of bacterial pneumonia (BP),
CT-halo sign was significantly more frequent in IPA (17/68 cases) than in BP (2/56 cases) [7].
- The frequency of cavitary lesion was not significantly different (IPA: 22/68 cases,
and BP 31/56 cases),
and air crescent sign was rather more frequent in BP (24/56 cases) than IPA (6/68 cases).
Candidiasis
- Candidiasis is seen in immunocompromised patients,
especially in those with malignancy,
diabetes mellitus,
AIDS,
and those treated with broad-spectrum antibiotics.
- Candidiasis frequently occurs concomitantly with bacterial infection; therefore,
it is difficult to mention the characteristic radiographic findings for pulmonary candidiasis.
Pathology
- According to Dubois et al,
the lesions of candidiasis are divided into hematogenous and endobronchial spread [8].
- In the former,
hemorrhagic nodules are the characteristic pathologic finding.
Central areas of necrosis and surrounding hemorrhage are observed and this feature is almost identical to that of angio-IPA.
- In candidiasis,
invasion and occlusion by Candida organisms of smaller-sized arteries than IPA.
- In the latter type of endobronchial spread,
the pathologic finding is bronchopneumonia,
which is identical to that of airway-IPA.
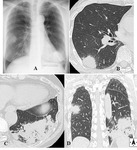
Chest radiographic findings
- Chest radiographic findings include patchy consolidation,
focal cavitation,
and multiple nodules,
which is a nonspecific finding (Fig.
10A,
11A,
and 11B).
HRCT findings
- In the hematogenous spread,
typical findings are nodules with halo sign.
This feature is almost identical to that of IPA and it is often difficult to distinguish (Fig.
10B,
10C,
11C,
and 11D).
These nodules seen in patients with candidiasis,
however,
are usually smaller than those in IPA.
- In the endobronchial spread,
centrilobular nodules,
tree-in-bud pattern,
and peribronchial consolidation (bronchopneumonia) are seen.
- In the report of Franquet et al who evaluated 17 HSCT recipients with proved pulmonary candidiasis,
while consolidation was predominant in 6 cases,
multiple nodules were predominant in 11 cases.
This feature is almost identical to that of IPA [9].
The difficulties of Differential diagnosis between IPA and candidiasis
- Althoff Souza,
et al.
evaluated 32 patients with IPA and 22 cases with candidiasis [4].
- They found that nodules were equally frequent in IPA (84%) and candidiasis (95%),
however,
nodules with centrilobular distribution were more frequent in IPA (96%) than in candidiasis (52%) and those with random distribution were more frequent in candidiasis (48%) than in IPA (4%),
which probably means that hematogenous and endobronchial spread are more common in IPA and in candidiasis,
respectively.
Concerning the size of nodules,
there was no significant difference between the two groups.
- They found that airspace consolidation was more frequent in IPA (84%) than in candidiasis (50%),
however,
there was no difference in the frequency of GGO.
There was also no difference in the frequency of halo sign and cavity.
Cryptococcosis
- Cryptococcus neoformans is found world-wide,
especially in soil contaminated by bird droppings.
- Cryptococcosis occurs in immunocompromised patients when the CD4 count is less than 100 cells/mm3 (secondary cryptococcosis),
as well as in healthy subjects (primary cryptococcosis).
This is a common disease in AIDS patients.
Pathology
- Nodules consist of a fibrous or fibrocaseous center surrounded by an airspace collection of macrophages and proteinaceous eosinophilic fluid.
Chest radiographic findings
- Chest radiographic findings are diverse,
and include multiple nodules or airspace consolidation,
GGO,
and reticulonodular pattern (Fig.
12A and 13A).
HRCT findings
- The characteristic HRCT findings differ between primary and secondary cryptococcosis.
- In secondary cryptococcosis,
cavitation within nodules is more common and pulmonary involvement tends to be more extensive compared with primary one (Fig.
12B and 12C) [10].
- Diffuse or extensive miliary nodules are seen only in severe immunocompromised patients,
such as AIDS patients [10].
- In primary cryptococcosis,
solitary or multiple nodules or airspace consolidation was predominant.
Nodules with halo sign are sometimes seen (Fig.
13B,
13C,
and 13D).
Mucormycosis
- Mucormycosis occurs in patients with diabetes mellitus,
renal failure,
or hematological malignancies,
and those who have undergone organ transplantation or intensive chemotherapy.
Pathologic and radiological findings
- Both findings of mucormycosis are almost identical to those of IPA.
- The frequent radiographic and HRCT findings include multiple airspace consolidation or nodules with halo or air crescent sign which,
based on the pathologic findings,
consist of hemorrhagic infarction caused by intravascular invasion of fungal organisms (Fig.
14A and 14B).
- It is difficult to distinguish this entity from IPA or candidiasis.
Unusual and particular conditions of fungal infection
- Due to the angioinvasive nature of fungus,
the following two severe condition can be caused by fungal infection; diffuse pulmonary hemorrhage (Fig 15) and intravascular fungal emboli (Fig.
16).
Diffuse pulmonary hemorrhage
- This entity seldom occurs in patients with fungal infection or in the immunocompromised patients with cytomegalovirus infection.
It probably occurs due to the disruption of pulmonary microvasculature due to the invasion of fungal organisms.
Intravascular fungal emboli
- Hypoxemia without apparent abnormal parenchymal CT findings may sometimes be observed in patients with fungal infection.
This condition seems to be induced by intravascular fungal emboli.
This mechanism is the same as that observed in patients with pulmonary thromboembolism,
intravascular lymphomatosis,
and leukostasis occurring in patients with leukemia.
Pneumocystis jirovecii pneumonia (PCP)
- Pneumocystis pneumonia (PCP) is caused by pneumocystis jirovecii which is now categorized as a fungus species.
- PCP frequently occurs in patients undergoing immunosuppressive therapy,
in recipients of solid organ or hematopoietic stem cell transplantation,
and in AIDS patients.
In AIDS patients,
the risk level increases significantly when CD4 + cell count falls below 200 cells / mm3.
- The mechanisms of onset of this entity have been regarded as a reactivation of latent infection,
however,
recent studies have also shown the possibility of an airborne route transmission or human-to-human transmission [11,
12].
- There is a possibility of a combined infection with CMV in 10% of cases.
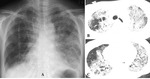
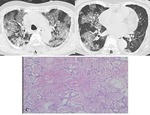
Pathology
- Characteristic pathologic findings include foamy intraalveolar exudates associated with the thickening of alveolar septa,
which is supposed to be very characteristic for PCP (Fig.
18C).
DAD may be the next frequent finding.
Chest radiographic findings
- The classic chest radiographic finding of PCP is a bilateral perihilar or diffuse symmetric ground-glass,
fine granular,
or reticular pattern (Fig.
17A).
- The chest radiography may have normal or nonspecific findings at the time of initial examination in as many as 40% of cases.
In the study of 51 cases with a high clinical suspicion of PCP in which chest radiography showed normal,
equivocal or nonspecific findings by Gruden et al,
PCP was detected in six of 51 cases and HRCT showed abnormal findings in all six cases [13].
It is evident that HRCT will be needed in the detection of early lesions of PCP when it is strongly suspected in the clinical settings.
HRCT findings
- Widespread GGO,
which distributes typically at the perihilar regions,
is the frequent and characteristic HRCT finding (Fig.
17B and 17C) [14].
- Extensive GGO is usually observed with sparing of adjacent secondary pulmonary lobules,
termed as mosaic or geographic pattern (Fig.
18A and 18B). Occasionally,
reticulation or intralobular and interlobular septal thickening within GGO may be recognized (crazy-paving appearance),
presumably reflecting a combination of fluid and cellular components within the alveolar space as well as thickening of the alveolar septa.
- Centrilobular opacities or tree-in-bud pattern are rarely seen.
- In AIDS patients,
cystic lesions,
upper lobe distribution,
lung nodules or masses,
lobar consolidation or interstitial fibrosis may be seen [15].
These findings are rare in non-AIDS immunocompromised patients.
- According to the report of Kuhlman JE,
et al.,
pleural effusion and hilar lymphadenopathy was seen in 18%,
which has been reported as rare findings in the assessment of chest radiography [14].
Differential diagnosis between other infections
- According to the report of Reittner et al.
who compared HRCT findings of PCP with bacterial,
other fungal,
viral,
and mycoplasma pneumonia,
GGO was significantly more frequent in PCP (95% of cases) than others,
while airspace consolidation was less frequent.
Centrilobular nodules were not observed in patients with PCP [16].
They concluded that the presence of extensive areas of GGO with absence of air-space consolidation is highly suggestive of PCP.
- According to the report of Hidalgo et al.,
who compared HRCT findings of PCP in AIDS patients,
the useful HRCT finding for the differentiation from other pneumonias was a diffuse or predominant GGO in the upper fields,
associated or not with reticulations and small cystic lesions [17].