Non-invasive disease
Subdivided into saprophytic (aspergilloma) and allergic bronchopulmonary aspergillosis (ABPA).
Aspergilloma
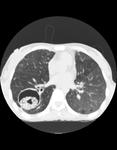
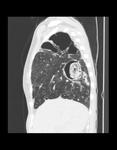
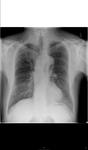
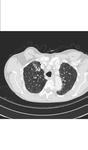
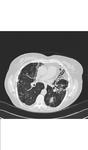
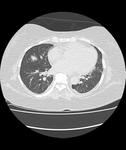
Aspergillomas appear as a mobile and rounded soft tissue nodule surrounded by a ring of air within a lung cavity synonymously with the air crescent sign.
These are the most common radiographic manifestation of aspergillus infection (Figures 1 and 2).
The differential diagnosis for the air crescent sign includes echinococcal cyst,
TB,
Rasmussen aneurysm,
lung abscess,
bronchogenic carcinoma,
haematoma or pneumocystis infection.
The aspergilloma classically moves when a patient changes position.
Associated with thickening of the cavity wall and pleura which is reversible.
ABPA
ABPA is caused by an immune response to aspergillus and causes mucoidimpaction in segmental or sub segmental airways.
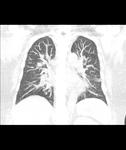
At imaging there is central bronchiectasis and with mucoid impaction which is known as the classic ‘finger in glove’ appearance (Figures 3 and 4).
These appearances are predominantly in the segmental or subsegmental bronchi of the upper lobes.
The differential diagnosis includes other causes of bronchiectasis or other endobronchial lesions causing mucoid impaction.
Invasive pulmonary aspergillosis
Most frequently seen in immunocompromised or critically ill patients as well as those with underlying lung disease,
invasive pulmonary aspergillosis is further subdivided into semi invasive (chronic necrotising),
airway invasive and angioinvasive disease.
Chronic necrotising pulmonary aspergillosis (CNPA)
Typically manifests as a peripheral bronchial mass resulting in bronchial wall thickening or bronchus obstruction and progressive uni- or bilateral segmental consolidation with nodularity (figures 5 and 6).
It can cause cavitation and is distinguished from aspergilloma by local invasion and constitutional symptoms.
Differential for narrowing of a central bronchus would include mucormycosis,
TB,
amyloidosis and sarcoidosis.
Airway invasive aspergillosis
This is characterised by the pressence of aspergillus organisms deep to the basement membrane on histology and occurs in immunodeficient patients.
The spectrum of imaging appearances results from tracheobronchitis and includes bronchiolitis characterised by tree-in-bud nodularity and bronchopneumonia (figures 7 and 8).
These radiological findings are usually in the peribronchial areas or more rarely in a lobar distribution.
Angioinvasive aspergillosis
The most commonly encountered invasive form is angioinvasive aspergillosis.
A central nidus of infection surrounded by haemorrhage and thrombosis giving rise to the halo sign appearance of a nodule surrounded by ground glass opacification.
When found early in the clinical course the halo sign can signify better clinical response to treatment (figures 9 and 10).